Another ACL Stem Cell Injection Procedure Result
©Regenexx
This is a guest post written by Dr. Bashir (and edited by me) as yesterday we were going over this before and after MRI of a patient seen here in Colorado. He will be opening his own Regenexx practice in the Miami area sometime this winter. This is his take on the patient’s MRI above:
“There is a hint of art in the field of interventional orthopedics. Deciphering the varying hues of ultrasound waves reflecting off different body tissues, thinking 3-dimensionally correlating XR images with strokes of contrast dye outlining structures, there is a bit of a tapestry created with every patient treated. Whether it’s a touch of a needle against a bone to encourage tendon reattachment, or a deeper dive of its tip against a bone to free a painful spur, the play of imagery and tissue refinement go hand in hand. This is the story of how the above image showing the torn and then improving knee ACL of a gymnast came to be through the new art and science of interventional orthopedics.
Having a working framework of the body’s anatomy in your mind and being able to match it to the high-tech images that surround our procedure rooms is what drives this new field of medicine. Through the comradely of long hours filled with brief and sometimes long patient storytelling, the doctors at the Centeno-Schultz clinic are constantly inventing new strategies to optimize patient care. Over the past several months, we have been optimizing the precise method of targeting both bundles of the ACL (anterior cruciate ligament) that we invented several years ago. Let me explain, and hopefully in the process, give a glimpse of a day in the life of a regenerative-medicine practitioner.
The ACL in Your Knee Is Pretty Complex
The ACL is one of many ligaments that stabilize the knee. It lives in the middle of the joint and controls the motion of the tibia on the femur. It can be traumatically injured or torn, and one of the most common orthopedic surgeries in the U.S. is to remove the torn ligament and install an artificial one.
I’ll begin with first explaining a little anatomy and how a patient who walks into our clinic eventually ends up on the procedure-room table. The ACL originates from deep within the notch of the distal femur. Its proximal fibers fan out along the medial wall of the lateral femoral condyle. There are two bundles of the ACL—the anteromedial (AM) and the posterolateral (PL), named according to where the bundles insert into the tibial plateau. (The tibia plateau is a critical weight-bearing region on the upper extremity of the tibia)1.The AM bundle is tight in flexion and the PL bundle is tight in extension. The AM bundle is more prone to injury with the knee in flexion, whereas the PL bundle is more prone to rupture in hyperextension and internal rotation2.
How Our Groundbreaking ACL Stem Cell Injection Procedure Works
When a patient presents with an ACL tear, there’s quite a bit that goes into deciding if a stem cell injection into the ACL is the right treatment. First there is the physical exam, which when correlated with MRI imaging offers us an in-depth understanding of the extent of the injured ligament. Varying physical-exam techniques can actually help us understand which of the two bundles is primarily injured.
Once the decision has been made that the patient’s injury is a good fit for the new technology of our ACL stem cell injection procedure, the patient finds himself or herself in a procedure room surrounded by very high-tech imaging equipment. The use of musculoskeletal ultrasound and fluoroscopy guidance allows precise placement of needles into injured structures to deliver healing agents derived from a patient’s own body.
Going back to our recent advancements in the groundbreaking technique of our ACL stem cell injection procedure I was sharing with you earlier, the generation of this refined technique took time, and many minds. First, the positioning of the patient’s knee has to be perfect to re-create through X-ray imaging (which we use in our procedure rooms) the elaborate MRI imaging just reviewed in the examination room. Months of adjusting angles of the X-ray beam, coupled with subtle shifts of knee flexion and extension with the patient placed faceup on the procedure table, led to the ability to target needles directly into specific points in both of ligament bundles I just described.
Once the needle is in place, the radiographic contrast (a substance that we can see on the fluoroscopy X-ray) outlines the bundles on the imaging matching perfectly with those seen on one view of the MRI. Once outlined, and correct needle confirmation is obtained, the stem cells are applied to help repair the injured tissue.
But this is only half the battle, as additional sites in each ligament bundle also must be targeted. This time using lateral X-ray imaging that correlates to other knee MRI slices, two more needles are advanced to precisely target both origin sites, and again contrast flow is used to outline the upper positions of both bundles.
Helping a Gymnast Avoid ACL Surgery
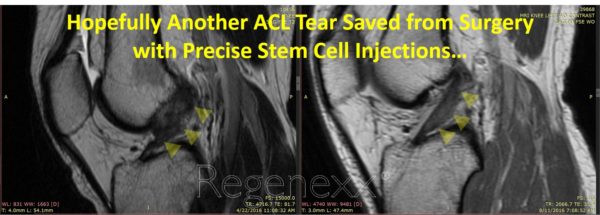
One of the earliest patients we used this groundbreaking ACL stem cell injection procedure on, JR a 30-year-old highly competitive gymnast, recently underwent a three-month MRI follow-up. The results as shown above are remarkable. Her original MRI, read as a complete tear, can be seen showing no clear demarcation of her ACL (which is outlined by the yellow triangles). To understand why the image on the left is abnormal, you need to look at the image on the right, taken several months after we precisely placed stem cells in the spots outlined above. Note that the ligament on the right looks taught compared to the image on the left. In addition, in the upper parts of the torn ACL on the left, you can see dark colors mixed with light. Those lighter tones on the image represent tearing in the ligament and a gymnastic career that may come to a screeching halt. Also note that in the image on the right the colors are now homogenously darker. All of this shows a ligament that’s moving in the direction of healing. Per her report she began feeling more stability and is walking without a brace over this past month. She is currently contemplating repeating the procedure to further increase tissue volume in the ACL, as her goal is to return to high-impact gymnastics once again.
The art of regenerative medicine is exciting for both patients and practitioners. One of the factors that facilitates our work is how intuitive the science is to both our patients and ourselves. Time and time again we hear our patients say, ‘This is the future of medicine, using the body’s own healing powers to generate repair.’ We couldn’t agree more. However, as you have seen above, the art of interventional orthopedics takes a great deal of cutting-edge science as well. Knowing exactly where to place stem cells to maximize the chances of recovery isn’t something you can learn from a YouTube video or that you learn in an orthopedic surgery or physical medicine residency; it takes years of dedicated study and practice.”
References:
1 https://en.wikipedia.org/wiki/Anterior_cruciate_ligament
2 http://www.wheelessonline.com/ortho/anatomy_of_acl
3 http://www.performanceorthosports.com/DOUBLEBUNDLEACL.html
4 http://www.ncbi.nlm.nih.gov/pubmed/17091538

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.