Backs Can Cause Knee Pain: To Understand Your Knee You Have to Get to Know Mine
I’m going to begin with a little known secret that will make sense as you read on…backs can cause knee pain.
On the first day of medical school, my dean stood up and told us that almost everything they were going to teach us about medicine would be wrong. What he meant was that we were just really beginning to understand how the body really worked and that most knowledge would change over the next 20-30 years. He was right and now I realize that it was a courageous statement, as most physicians grip to that “reality” taught in medical school like a toddler’s security blanket. So this morning I will tell you that just about everything you think you know about your knee is wrong. Regrettably it’s based on a surgical conception of the orthopedic system. In fact, to really understand how your knee works and why it hurts, you need to get to know my knee.
In April I had the honor of speaking at the Vatican on stem cells. I also had the honor of spending many hours on a plane followed by my bright idea to take up running in a local park near the Rome hotel (to keep up with my active wife). By the time we took the train from Rome to Venice, the back outside of my knee, near the hamstrings, was a bit tight. This followed about 5 miles a day of walking in Venice for a week. By the flight home (Venice-Rome, Rome-New York, New York-Denver), every time I went to stand up from my seat, the back outside of my knee hurt. After subsequent lectures in Phoenix and Florida, I was limping for the first few minutes after getting up from being seated. By the next week, every time I bent my knee I could feel it swollen. By the week after that the whole knee hurt. Had I not understood what happened, I would have believed I had early knee arthritis. However I would have been very wrong.
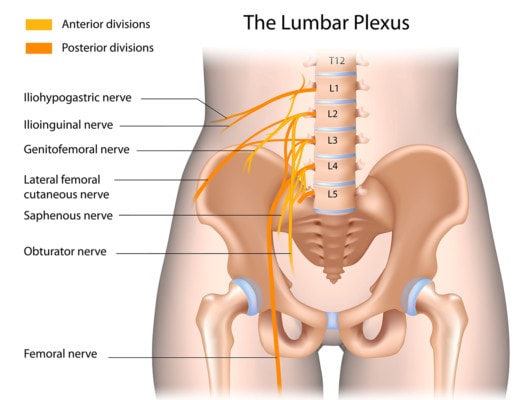
Alila Medical Media/Shutterstock
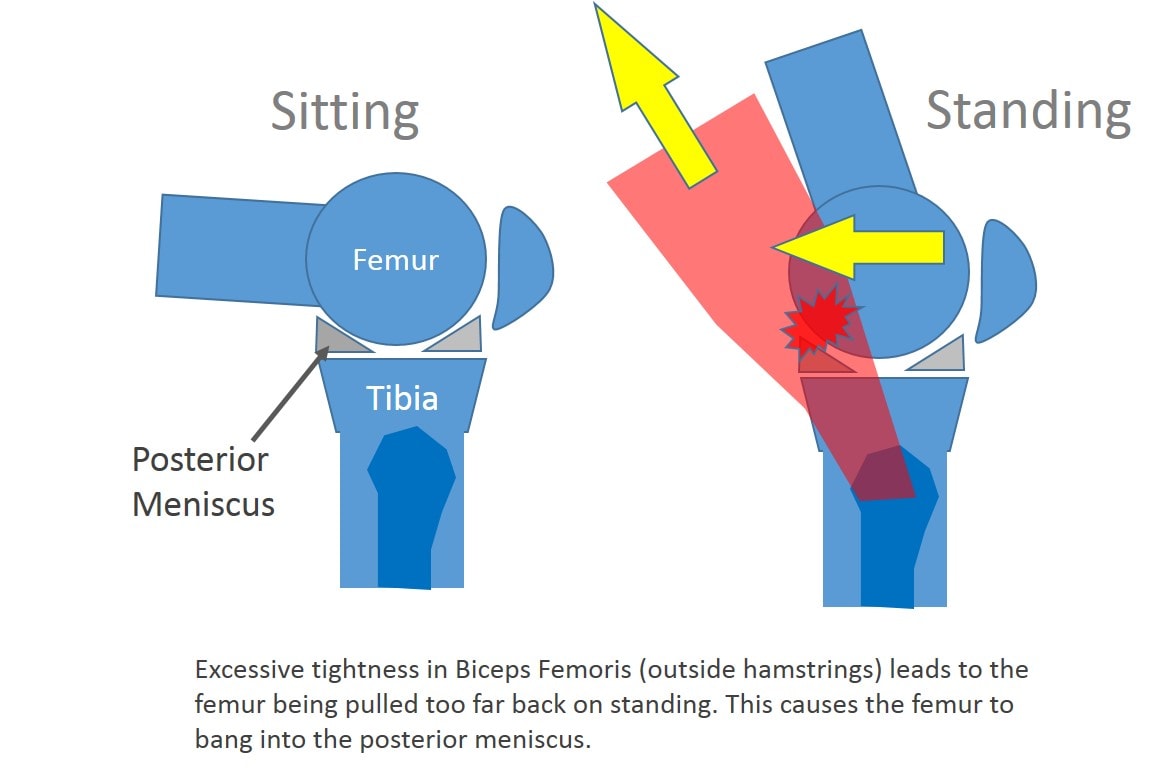
What happened and what does it have to do with you? The right L5 nerve in my back had been a smoldering problem for months. That’s not to say that I had huge amounts of back pain, I didn’t. How then did I know this? My right big toe was developing a small bunion on the outside. To better understand why, see my discussion of how nerves in your back can cause bunions. That same L5 nerve goes to the outside hamstring muscle also known as the biceps femoris. All that sitting on planes had caused a small disc bulge that I have at L5-S1 to irritate the exiting L5 nerve (sitting reduces the disc height and increases the bulge by pushing water out of the disc). This in turn made my lateral hamstrings tight (see above) which in turn impacted how my knee joint worked. When I went to stand up, the tight hamstrings muscle didn’t allow my femur to get out of the way of the back/outside meniscus, pinching the tissue. In effect, the tight muscle pulled my outside femur too far back (see below). After a few weeks of this, the meniscus began to complain and my body attempted to fix it by mobilizing the stem cells in my knee and other inflammatory cells. Since the trauma was ongoing, the swelling stayed.
How do I know for sure this was it? I have a few good clues other than the ones I discussed above. First, when I aggressively massaged the outside hamstrings before standing, I felt no pain in the knee on standing. Second, I purposefully had one of our Docs inject the lateral hamstring tendon and joint with Regenexx-SCP. It helped a bit, but didn’t change the overall picture as the hamstring tightness was still there. Finally, I had Dr. Schultz perform the Regenexx-PL-Disc procedure to treat that nerve and the issue let up substantially. Had I left it like this, I would have developed a nasty tear and cartilage defect in my lateral posterior meniscus and femoral condyle, leading a surgeon to cut out a chunk of that meniscus and debride my “lesion”. The focus would have been on my knee rather than on the true cause in my low back, so I would have had a series of failed surgeries ending in a possible knee replacement at some time in the future, because most docs don’t know that backs can cause knee pain.
In conclusion, I can break down our old orthopedic teachings as follows:
-The problem is always where it hurts. Wrong, it’s frequently caused elsewhere. However, once a secondary cartilage lesion starts from the primary problem, both now have to be treated.
-The musculoskeletal system is simple. Wrong, it’s an extraordinarily complex and delicate machine made of nerves, muscles, fascia, and joints. You can’t understand any part of it without understanding the whole. You can devote an entire career to understanding it all and still learn new things everyday.
-Removing parts and pieces of joints is a good idea most of the time. Wrong, it’s almost always a bad idea. There are no extra parts. When extra parts do grow like bone spurs, the clinician must ask himself the obvious question, why is that bone spur there? It almost always forms because of another problem that is the primary concern, the bone spur is almost always a secondary issue.
The upshot? In order to really understand how you can stay active at high levels as you age, you must understand how your body works. It specifically doesn’t work the way you’ve likely been taught. When one part hurts, it’s usually not that part that caused the problem!

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.