My Calf Muscle Tear Was Caused by My Low Back
This week I had what I call my first “old man” injury, a calf muscle tear while climbing the stairs. Really? Climbing the stairs? What am I, 80? In addition, I should have known that I was high risk for something like this as I had warning signs screaming for the last several weeks. In fact you may have warning signals blaring right now, but you’re likely ignoring them, just like I did. Let me explain.
Our Understanding of the Orthopedic System Is Stupidly Simplistic
The body is one connected machine, yet we have broken it into systems. I think we’ve done this so that we can comprehend how it works? Or maybe we do it so it’s easier to give tests in medical school? Not sure. However, what I am certain about is that our oversimplification and compartmentalization of the orthopedic system has harmed patients.
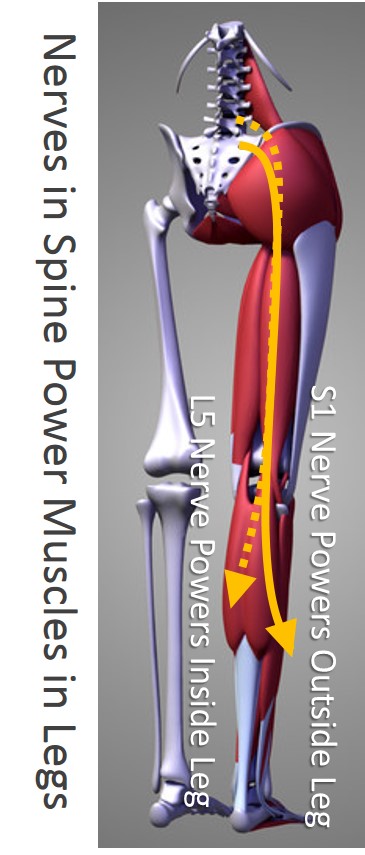
Why Did My Calf Muscle Tear?
I have a degenerated disc in my low back that sometimes irritates my S1 nerve. I can tell when it’s active because parts of my calf muscle will begin to very subtly rapid fire—a phenomenon known as “fasciculations.” I’ll also get pain in my outside ankle where the S1 nerve travels, and my calves will get tight. Notice I didn’t say my back hurts very much when this nerve is irritated. In fact, that’s much more rare.
So why did my calf muscle tear when I was just bounding up the stairs in my office as I had done many, many times before? Remember above when I said the nerve and the muscle are one and the same? For example, what happens to the nerve impacts the muscle. So pressure on the nerve in my low back led to my calf muscle getting tight and firing abnormally, and years of intermittent nerve irritation also likely led to the muscle being structurally weaker. Hence, I hit the step in just the right way and while the S1 spinal nerve signals telling the muscle what to do were delayed just enough so that the muscle tore.
What Were the Warning Signs I Missed, and What Should I Have Done to Prevent My Calf Tear?
Man did I have warning signs for my calf tear. Given that I knew how to interpret them, it was as if my body had painted a big red sign on the back of my eyeballs that read, “Dude, your back nerves are messed up and you’re going to injure something!” So what were the warning signs?
- The jumping of my calf muscles
- Tightness in my calves
- On and off low back pain—remember I noticed my leg issues more than my back.
- A sense that the small muscles that stabilized my back were “off-line.” I knew this because small innocuous movements, especially in the morning, would cause me to get small pains in my back that I would immediately prevent by reminding my body, “Don’t do that.” In essence, I could tell that at any minute, if I moved the wrong way, my back could “go out.”
- Pain on the outside of my ankles
- Pain in the outside of my hips
Notice that with many of the symptoms above, the average person would assume there was an issue where it hurt or was tight (e.g., in my hips, ankles, or calves). However, because I know what the S1 nerve can cause and I know my body, I knew how to interpret this constellation of symptoms and connect it to my back.
Now if I had actually been smart enough and less busy, I should have had one of my partners inject some of the growth factors from my blood platelets around my irritated S1 nerve. It would have taken all of 20 minutes and likely prevented my calf muscle tear by calming down the nerve and reducing the tension in the muscle. I could have also had a physical therapist dry needle my low back muscles and calf, which would have likely prevented the tear.
Understanding How to Be ProActive…

The upshot? The body is one big connected machine. We have compartmentalized it to make it easier to understand, but we’ve done a great disservice to patients by doing so. It also comes as a shocker to patients that their low back may be causing a problem in the hip, knee, or ankle when their back doesn’t hurt much, but take my word for it, it’s much more common than you think. So take an hour and read my book ProActive and be a bit smarter than I was this week—get your little issues fixed by noticing the status updates your body is giving you before a train hits you from left field and sidelines your active lifestyle!

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
