Chronic Tennis Elbow? What Causes It and How Is It Treated?
Chronic tennis elbow pain can be disabling. You go to open a door or shake a hand and you’re in extreme pain. So what do you do when medication, braces, or physical therapy doesn’t work?
What is Tennis Elbow?
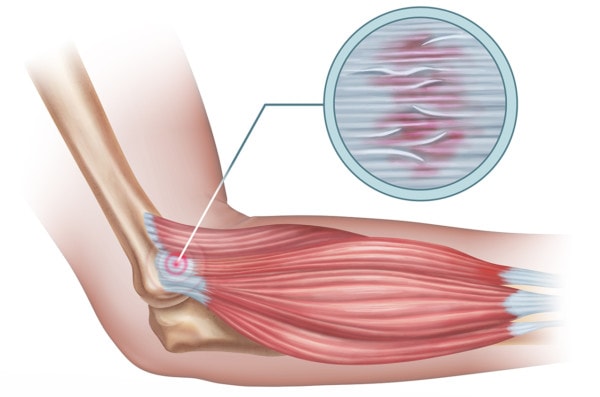
Andrea Danti/Shutterstock
Tennis elbow is also called lateral epicondylitis. This means that the forearm muscle tendons which originate on the outside of the elbow bone are damaged and degenerated. This causes the tendons to be painful and any use of those muscles that extend the hand is also painful. At any given time, about 1 in 100 people have tennis elbow with the problem peaking in middle age. Smoking is a risk factor. (1)
Does Tennis Elbow Go Away? What Happens if Tennis Elbow Goes Untreated?
Tennis elbow can last for 12-18 months if left untreated (5). If the problem gets worse over time, the tendons can progress from micro-tears to larger tears (13). Hence, it’s best to get treated if the problem is taking a long time to resolve or worsening to avoid chronic tennis elbow.
Why Is My Tennis Elbow Not Healing?
Traditionally it’s been thought that tennis elbow is caused by inflammation or swelling in the tendons, but research studies have shown this to be inaccurate. What they do show is that the tendon is degenerating (2). Other research has shown that the pain from the condition causes less use of the tendon which then causes more degeneration (3). In addition, it’s common that patients with tennis elbow have neck pain, so it’s been thought that irritation of spinal nerves in the neck may be one factor keeping the tendon from healing. Finally, steroid injections have been shown to be more harmful than helpful (4).
How Do You Treat Chronic Tennis Elbow?
A mainstay of treatment for chronic tennis elbow has long been physical therapy and exercises (5). However, when that doesn’t work, three main treatments have been traditionally used:
- Braces
- Steroid injections
- Surgery
Braces – The theory is that these make the tendon more efficient, regrettably, the research has shown this type of treatment is not very effective at reducing symptoms (6).
Steroid Injections – Even though they are commonly used, multiple studies have shown that injections of steroid anti-inflammatories are ineffective (4,7).
Surgery – A recent high-level clinical trial showed that surgery was no better than a sham procedure, meaning surgery doesn’t work (8).
Is There a Connection Between Tennis Elbow and the Neck?
Golfer’s elbow (a very similar condition on the inside of the elbow) has been shown to be related to pinched nerves in the neck (9). Irritated nerves are also related to tennis elbow (10). Finally, neck pain is more common in patients that have tennis elbow (11). As a physician, I have observed this connection for many years and we often treat the neck in conjunction with the elbow to enhance results.
Newer Treatments for Tennis Elbow
If surgery doesn’t work well, what does? We have used a procedure that we call Perc-Orthobiologic Fenestration (POF) which is a precise ultrasound-guided injection of the patient’s own super-concentrated healing platelets combined with “fenestration”. This means that the doctor numbs the area and then carefully pokes small holes in the degenerated tendon to get new tissue to grow into those spots, much like “aerating” your lawn in the spring.
Multiple studies have shown much better long-term results for this platelet based approach then steroid shots (12). Below is a video of an ultrasound guidance image that shows a needle (entering from the right) demonstrating how that procedure works. We also frequently treat the neck at the same time if that’s involved. If platelet based therapies are ineffective in chronic tennis elbow, then the next step is using stem cells from the patient’s own bone marrow.
The upshot? Chronic tennis elbow can be a pain, in that many of the traditional treatments like steroid shots and surgery don’t work well. However, there are newer treatments that work much better.
___________________________________________________
References:
(1) Shiri R, Viikari-Juntura E, Varonen H, Heliövaara M. Prevalence and determinants of lateral and medial epicondylitis: a population study. Am J Epidemiol. 2006 Dec 1;164(11):1065-74. https://www.ncbi.nlm.nih.gov/pubmed/16968862
(2) Doran A, Gresham GA, Rushton N, Watson C. Tennis elbow. A clinicopathologic study of 22 cases followed for 2 years. Acta Orthop Scand 1990;61:535-538. https://www.ncbi.nlm.nih.gov/pubmed/2149254
(3) Coombes BK, Bisset L, Vicenzino B. A new integrative model of lateral epicondylalgia. Br J Sports Med 2009;43:252-258. https://www.ncbi.nlm.nih.gov/pubmed/19050004
(4) Coombes BK, Bisset L, Vicenzino B. Efficacy and safety of corticosteroid injections and other injections for management of tendinopathy: a systematic review of randomised controlled trials. Lancet. 2010 Nov 20;376(9754):1751-67. doi: 10.1016/S0140-6736(10)61160-9.
(5) Vaquero-Picado A, Barco R, Antuña SA. Lateral epicondylitis of the elbow. EFORT Open Rev. 2017;1(11):391–397. Published 2017 Mar 13. doi: 10.1302/2058-5241.1.000049
(6) Bisset L, Paungmali A, Vicenzino B, Beller E. A systematic review and meta-analysis of clinical trials on physical interventions for lateral epicondylalgia. Br J Sports Med. 2005;39(7):411–422. doi: 10.1136/bjsm.2004.016170
(7) Claessen FMAP, Heesters BA, Chan JJ, Kachooei AR, Ring D. A Meta-Analysis of the Effect of Corticosteroid Injection for Enthesopathy of the Extensor Carpi Radialis Brevis Origin. J Hand Surg Am. 2016 Oct;41(10):988-998.e2. doi: 10.1016/j.jhsa.2016.07.097.
(8) Kroslak M, Murrell GAC. Surgical Treatment of Lateral Epicondylitis: A Prospective, Randomized, Double-Blinded, Placebo-Controlled Clinical Trial. Am J Sports Med. 2018 Apr;46(5):1106-1113. doi: 10.1177/0363546517753385.
(9) Lee AT, Lee-Robinson AL. The prevalence of medial epicondylitis among patients with c6 and c7 radiculopathy. Sports Health. 2010;2(4):334–336. doi: 10.1177/1941738109357304
(10) Fernández-de-Las-Peñas C, Ortega-Santiago R, Ambite-Quesada S, Jiménez-Garcí A R, Arroyo-Morales M, Cleland JA. Specific mechanical pain hypersensitivity over peripheral nerve trunks in women with either unilateral epicondylalgia or carpal tunnel syndrome. J Orthop Sports Phys Ther. 2010 Nov;40(11):751-60. doi: 10.2519/jospt.2010.3331.
(11) Berglund KM, Persson BH, Denison E. Prevalence of pain and dysfunction in the cervical and thoracic spine in persons with and without lateral elbow pain. Man Ther. 2008 Aug;13(4):295-9. Epub 2007 Oct 17. https://www.ncbi.nlm.nih.gov/pubmed/17942362
(12) Xu Q, Chen J, Cheng L. Comparison of platelet rich plasma and corticosteroids in the management of lateral epicondylitis: A meta-analysis of randomized controlled trials. Int J Surg. 2019 Jul;67:37-46. doi: 10.1016/j.ijsu.2019.05.003.
(13) Mackay D, Rangan A, Hide G, Hughes T, Latimer J. The objective diagnosis of early tennis elbow by magnetic resonance imaging. Occup Med (Lond). 2003 Aug;53(5):309-12. https://www.ncbi.nlm.nih.gov/pubmed/12890829

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
