Does Low Back Surgery Cause Damage to the Fascia? What Is the Fascia?
Your muscles are surrounded by something called fascia. This structure commonly gets injured in low back surgery. What is fascia and why should you care if yours is injured? Let’s dig in.
What Is Fascia?
Fascia covers our muscles and contains them. Look at the diagram above. The muscle is surrounded by a thick fascia. That is then made up of muscle bundles that are also surrounded by fascia. Those budles contain individual muscle fibers.
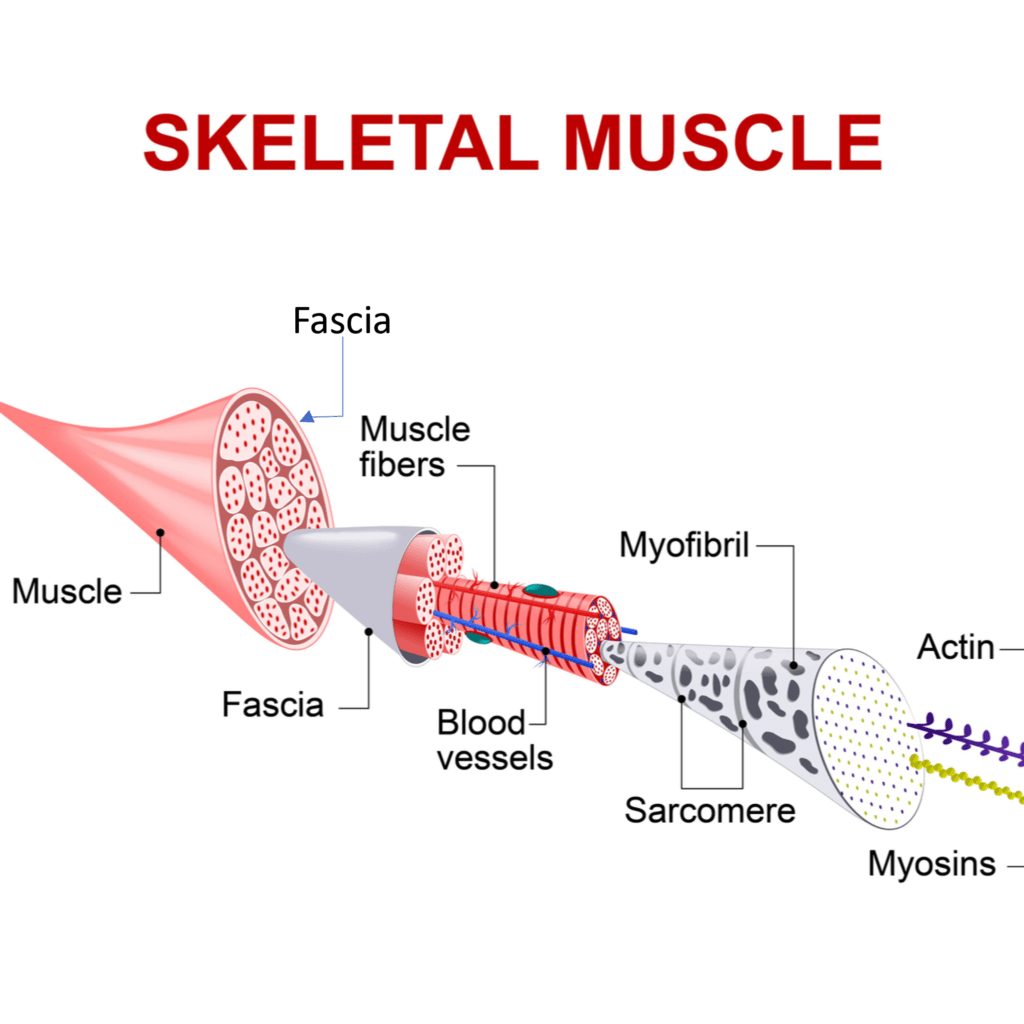
Credit: Shutterstock
Think of fascia as a way for the muscle to direct force. Given that a muscle has a tendency to bunch up as it contracts i.e. when you flex your biceps the muscle gets a bit bigger in the middle, if we can redirect that sideways force lengthwise, we can get more power out of the muscle.
The Thoracodorsal Fascia
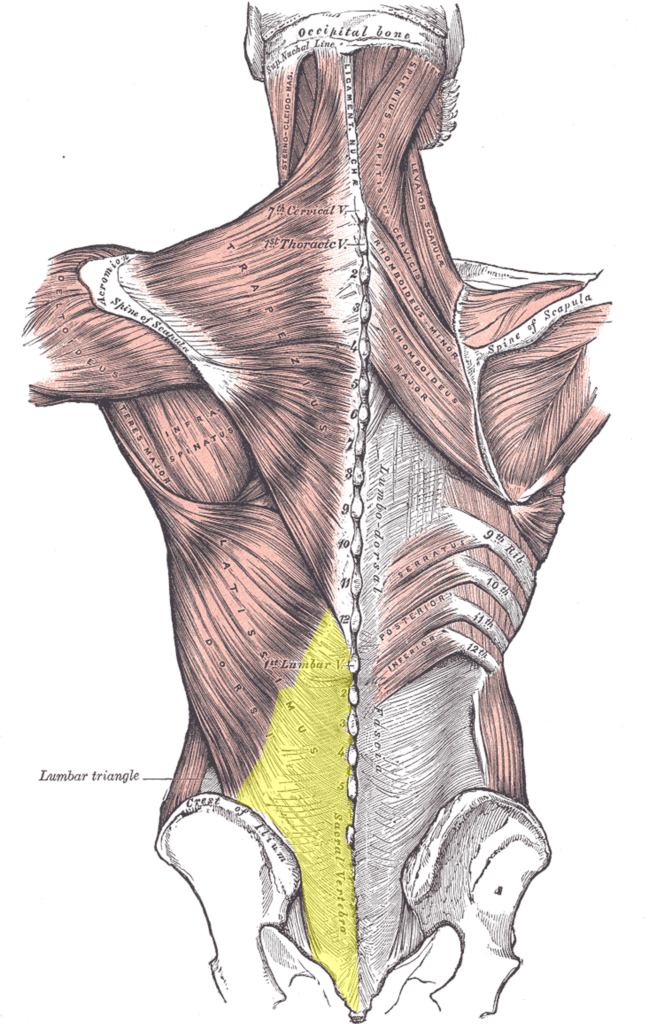
By Henry Vandyke Carter – Henry Gray (1918) Anatomy of the Human Body-Wikipedia Public Domain
The single largest piece of fascia in your body is the one covering the low back and is called the thoracodorsal fascia (TDF). In the diagram above, I’ve colored the TDF yellow (on the left). This is the main fascia that covers the low back muscles (along with the fascia around the individual muscles) that helps your low back muscles generate maximum force for lifting. It’s also a critical force transmitter between the arms (through the latissumus dorsi muscle) to the core.
The Normal versus Damaged TDF on MRI
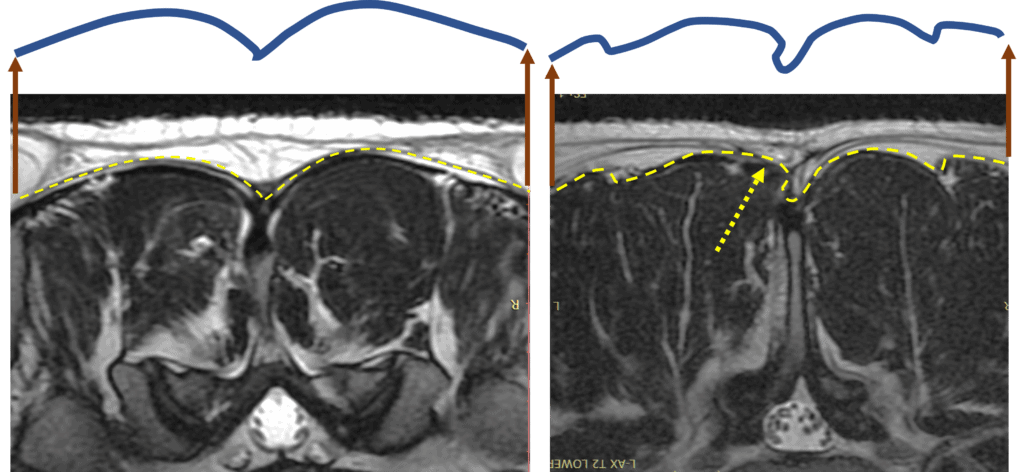
Now let’s look at some actual MRI images from a real patient. The image on the left shows the low back, with the dark being the muscle. This axial view kind of looks like a steak you buy in the grocery store. The yellow dashed line is the TFD, which I have traced again and have in purple above. Note how it’s asymmetrical from left to right of the spine. Now, look at the right image, which is a patient who had low back surgery (a micro-discectomy). Here the nice symmetrical yellow dashed line representing the TDF is downright squiggly on the left side of that MRI. The arrow points to a blowout in the fascia. This means that there’s a weakness here created by the surgery and the muscle fibers are poking out of that weak area. For another view, see my image below:
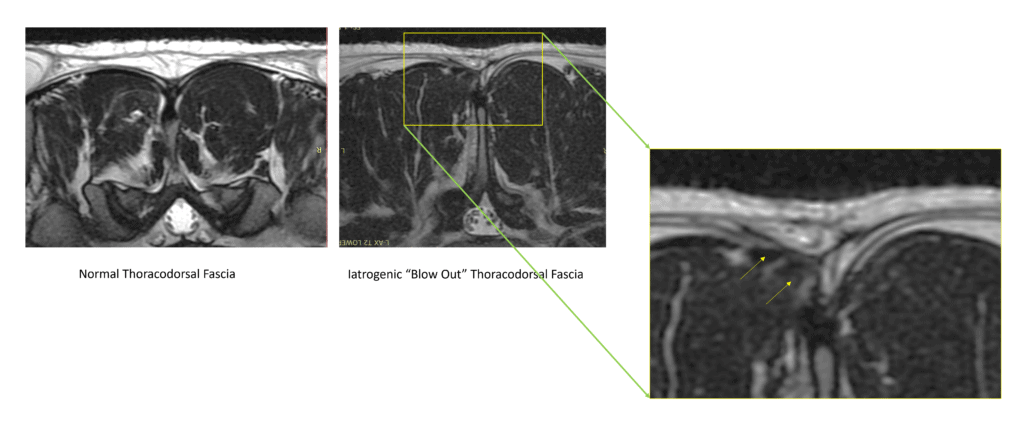
How Common Is this Problem?
In about 1 in 4 patients who have had back surgery, I can find a fascial blowout on MRI or on an ultrasound exam. Hence, this issue is more common than you might think.
What Impact Does a Fascial Blowout Have?
A fascial blowout means that the tight constraints on the muscle are gone, so the muscle contraction will be less efficient. In addition, these can be sites of pain all by themselves. Hence, identifying these areas is critical in helping patients with chronic low back pain or sciatica.
Can This Be Treated?
Yes, a fascial blowout in the TDF can usually be treated by injecting high-dose platelet-rich plasma (PRP) and/or bone marrow concentrate if the area is recalcitrant to PRP. The injection is performed precisely into the damaged area using ultrasound guidance. The goal is to stimulate the healing of the TDF.
The upshot? Fascial damage from back surgery is more common than you think. Finding and treating these areas either on MRI or using an ultrasound exam is an essential part of getting you back to normal!

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
