Headaches from Your Neck and Posture
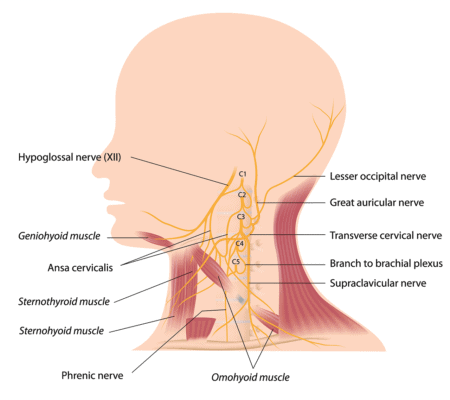
Alila Medical Media/Shutterstock
Cervicogenic headaches come from the neck and they can be caused by lots of things. However, some new research this morning shows that a simple issue like posture could be causing quite a few. Let’s dig in.
Cervicogenic Headache
Cervicogenic headaches start in the neck and are primarily felt in the head. They often follow an injury like whiplash or are associated with a cervical spine problem. They generally come from the upper neck.
Common causes of cervicogenic headache include:
- Irritation of one of the nerves that go from the neck to the head. These include the greater, lesser, and third occipital nerve (back of the head) as well as the superficial cervical plexus (front of the neck).
- Damage to or arthritis of the C0-C1, C1-C2, or C2-C3 facets.
- Trigger points in the upper neck muscles.
These are some of the damaged structures that can cause headaches, but what can cause these areas to become painful? Here’s that list:
- Craniocervical Instability. When the ligaments that hold the head on are loose.
- Direct trauma to any of the structures above.
There is a third, which is your posture. Posture in this case means the relative position of your head on your neck. Let’s dig into some new research on head position and headaches.
New Research
Researchers of a new study, published in Musculoskeletal Science and Practice, evaluated 3D images of 200 individual’s postural alignment — 100 individuals who’d had frequent headaches for at least 3 months and 100 control patients of the same age and gender.
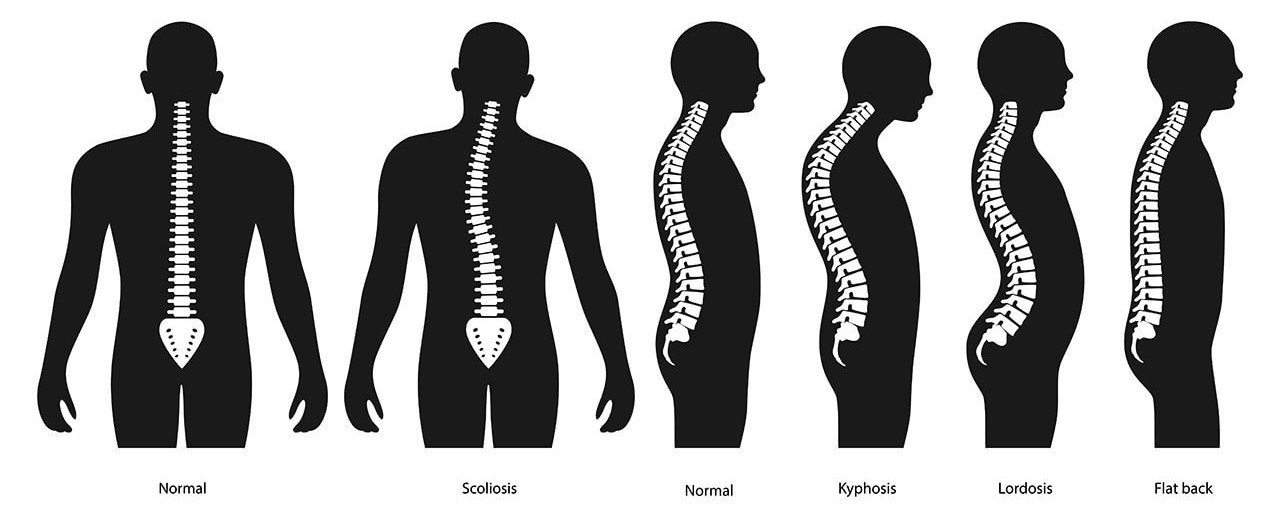
The results showed that increased thoracic kyphosis, increased coronal imbalance (scoliosis), and increased vertebral rotation were all associated with a higher risk of cervicogenic headache.
Digging into the Terms
Thoracic kyphosis means that your head is forward and the upper part of your back is also bent forward. Increased coronal imbalance means a side bent spine or scoliosis. See image below.
Vertebral rotation goes hand and glove with scoliosis as when the spine bends it also rotates.
What All of That Means and What You Can Do
All of this means that if the spine beneath your head is bent forward or sideways, that’s associated with more headaches. Why? The structures in the upper neck are getting irritated or damaged by that imbalance. Meaning forces are building up on one spot rather than being equally distributed.
What can you do? Get the kyphosis or scoliosis corrected. Fixing the kyphosis we all get as we age is easier if you start early. Click here to see my old man doorway stretch that can help. On what to do with scoliosis, click to learn more.
The upshot? At the end of the day, make sure your spine stays as young-looking as possible. That nasty forward head that we all get from age or looking down at our phones may well be causing your headaches. The same holds true with scoliosis. Just remember, starting to work on this stuff early is key.
RELATED
>> Everything You Need To Know About Cervicogenic Headaches
___________________________________
References:
Moustafa IM, Shousha TM, Harrison DE. An investigation of 3D spinal alignment in cervicogenic headache. Musculoskelet Sci Pract. 2020 Nov 2;51:102284. doi: 10.1016/j.msksp.2020.102284. Epub ahead of print. PMID: 33212363.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.