Is This the Truth About Knee Replacement Surgery?
I consulted Dr. Google this morning to find out what it said about knee replacement results. What I found was interesting and disturbing:
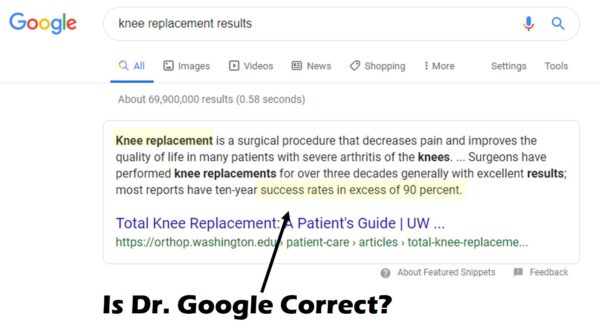
So what’s the truth about knee replacement surgery? Most people believe that it’s like just going to your mechanic and getting a worn-out part replaced in your car. Is that true? Not so much. Let’s review.
Dr. Google and The Truth About Knee Replacement?
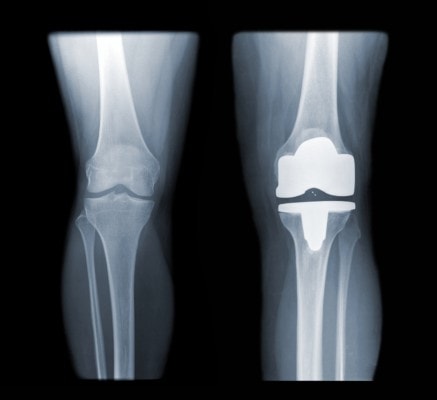
The knee on the right has been replaced. Skyhawk X/Shutterstock
Google made some huge search algorithm changes last year that seem to have prioritized health content from University websites. The good news was that the content was supposed to be vetted through the lens of medical research. The bad news is that university medical schools are businesses no different than the hospital down the street. Meaning, the average university orthopedics department offers many surgeries we know don’t work or where we have little high-quality research.
So does a 90% success rate as reported by the University of Washinton website (see the screenshot above) really represent the truth about knee replacement surgery? While this page was authored by an academic orthopedic surgeon, regrettably, there isn’t a single research citation on the page. Near as I can tell this is just his personal opinion. So is this accurate?
What is the Actual Success Rate of Knee Replacement Surgery?
To understand the truth about knee replacement surgery, we need to dive deeper than Dr. Google. While the source in the Google snippet quotes a very high success rate, the problem is that it’s not actually based on high-level evidence. What’s that? Research that uses the gold standard randomized controlled trial (RCT) study design or other tried and true methods. Let’s dig in.
The best study to date performed on knee replacement is a 2015 RCT that compared knee replacement to physical therapy. This showed some interesting things, none of which really support that 90% number (1):
- 3 in 4 patients in the physical therapy group decided not to get a knee replacement
- About half of the knee replacement group reported some sort of serious complication
- While the knee replacement group had better functional improvement than physical therapy in some tests, in others there was no difference
- You needed to perform 6 knee replacements before one person reported that they had at least 15% better function (this is called an NTT of 6)
So the results weren’t stellar and certainly nothing close to what Dr. Google tells us. Let’s dig deeper.
More Knee Replacement Success Rates
Another way to find out the truth about knee replacement is to look at whether it’s cost-effective. A study based on a government-funded arthritis database did just that (2). The result? Knee replacement wasn’t cost-effective for the majority of people studied. Why?
In this research, the results were better for patients who were more disabled before the surgery. Meaning if the patient couldn’t walk far due to knee arthritis pain, they benefitted from knee replacement. However, the procedure wasn’t cost-effective in more active patients.
So given this study, we’re still nowhere near 90% effective. Let’s look at success another way to see if we can get there. In this case, we’ll look at the percentage of people who still have pain after knee replacement. After all, our university-based orthopedic surgeon on this UW website page wrote, “The large majority (more than 90 percent) of total knee replacement patients experience substantial or complete relief of pain once they have recovered from the procedure.” Does the research back this up?
In one recent study, about a year after knee replacement, 4 in 10 patients still reported a 3-5/10 pain in the knee (3). In another study, 44% of knee replacement patients reported persistent pain with 15% of those patients having severe pain (4). The graph below from one of these studies shows this information nicely:
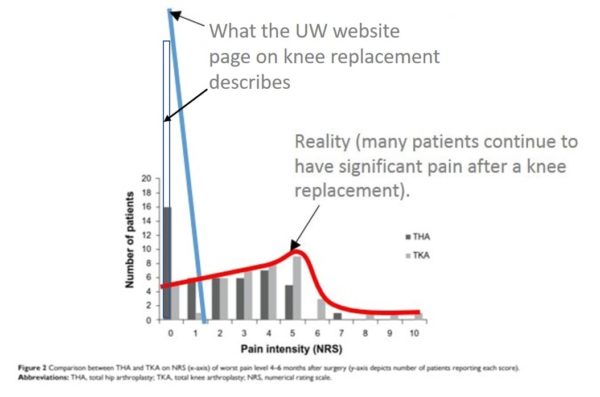
So what does this graph show? The Y-axis is the number of patients at each 1-10 pain number and along the bottom, you have the pain numbers. If you look at the graph, if what the UW orthopedic surgeon said were true and verified by this study, then we would see a huge bar at 0/10 representing 90+% of the patients (which I drew here as the blue hollow bar). So if we drew a line representing that trend, it would go straight down (like the blue line I drew). However, what was really reported by actual knee replacement patients is represented by the red line. Meaning lots of people were still in pain despite the knee replacement.
How about if we look at a return to activity? After all, most knee arthritis patients want to become active again. A review of another government database showed that only 5% or less of patients go back to normal activities (8). Yet another study showed that after knee replacement, patients were only able to accomplish less than 1/2 of the hours of physical activity they had expected. For example, patients expected to be physically active 23 hours a week and in reality, it was 11 hours (11).
So our quest to find the truth about knee replacement and support that 90% success rate quoted online is a bust. The success rate of knee replacement is nowhere near that high.
Is a Total Knee Replacement Painful?
Well given that the success rate is much lower than 90%, this becomes an important question. Research shows that about half of knee replacement patients will have their worst pain in the first two weeks after surgery (5). About half of those patients will have severe pain some of the time and about a quarter will have that level of pain most of the time.
What are the Risks of Knee Replacement?
If the actual results of knee replacement were as good as described by Dr. Google, maybe the risks wouldn’t come into play as much. However, now that you know what the actual research says, a discussion of risks becomes more important. The risks can be broken down into the following categories:
- Infection (12)
- The need for a second surgery (revision), which happens in about 6% of patients (13)
- Knee replacement patients are 9 times more likely to have a heart attack (6). The risks go up from there with almost 20% of patients with a prior serious cardiac history having heart side effects after the surgery (7).
- A build-up of toxic metal ions in the blood (9, 10)
Is There a Knee Replacement Alternative?
Our clinics have been using an image-guided bone marrow concentrate injection technique (that contains stem cells) for 15 years to help patients avoid knee replacement. This is called Perc-TKA. We recently published a similar RCT to the one described above where the less invasive injection-based technique was compared to physical therapy. More than 2/3rds of the patients met the functional criteria for success at 2 years out (14). So that procedure has helped many patients avoid big surgery.
A Non-Surgical Success Story
The UW web-page quoted above has a video of a surgery patient skiing which is an unabashed advertisement for knee replacement. So here’s a success story for our Perc-TKA on a patient who was living in the Seattle metro area:
This was Paul Lyon’s post on Facebook in 2017 (4 years out) about how he was doing at that point (he now lives in Hawaii)::
“Paul Lyon Regenexx I believe uses and supports the use of prp. Had stem cell procedure done on both knees done 4 years ago at Regenexx. I had 2 separate orthopedic doctors prior to having stem cell procedure done said I need to replace both knees. I’m leaving Saturday for helicopter ski trip…. my knees are not perfect, put seldom any pain. I’m 70, plan on hitting 100, pretty sure I won’t need my knees replaced.
Feel free to contact me about my experience.
Helicpter Skiing was Fantastic. ..I was the oldest, next day, no pain at all…others, very sore. Aloha,”
Two years later in 2019: Yes..6 years ago couldn’t hardly walk, ski, bike…… I ski hard, bike hard and live life…oh, and I’m 73. Don’t go to your “neighborhood stem cell doctor”…Regenexx started stem cell therapy…the leaders.
Then we have this on Facebook, yet another Perc-TKA patient who lives in UW’s backyard who is 9 years out from the procedure:
______________________________________
References:
(1) Skou ST, Roos EM, Laursen MB, Rathleff MS, Arendt-Nielsen L, Simonsen O, Rasmussen S. A Randomized, Controlled Trial of Total Knee Replacement. N Engl J Med. 2015 Oct 22;373(17):1597-606. doi: 10.1056/NEJMoa1505467
(2) Ferket Bart S, Feldman Zachary, Zhou Jing, Oei Edwin H, Bierma-Zeinstra Sita M A, Mazumdar Madhu et al. Impact of total knee replacement practice: cost effectiveness analysis of data from the Osteoarthritis Initiative BMJ 2017; 356 :j1131 https://www.bmj.com/content/356/bmj.j1131
(3) Sakellariou VI, Poultsides LA, Ma Y, Bae J, Liu S, Sculco TP. Risk Assessment for Chronic Pain and Patient Satisfaction After Total Knee Arthroplasty. Orthopedics. 2016 Jan-Feb;39(1):55-62. doi: 10.3928/01477447-20151228-06.
(4) Wylde V, Hewlett S, Learmonth ID, Dieppe P. Persistent pain after joint replacement: prevalence, sensory qualities, and postoperative determinants. Pain. 2011 Mar;152(3):566-72. doi: 10.1016/j.pain.2010.11.023.
(5) Chan EY, Blyth FM, Nairn L, Fransen M. Acute postoperative pain following hospital discharge after total knee arthroplasty. Osteoarthritis Cartilage. 2013 Sep;21(9):1257-63. doi: 10.1016/j.joca.2013.06.011.
(6) Lu N, Misra D, Neogi T, Choi HK, Zhang Y. Total joint arthroplasty and the risk of myocardial infarction: a general population, propensity score-matched cohort study. Arthritis Rheumatol. 2015;67(10):2771–2779. doi: 10.1002/art.39246
(7) Feng B, Lin J, Jin J, Qian W, Cao S, Weng X. The Effect of Previous Coronary Artery Revascularization on the Adverse Cardiac Events Ninety days After Total Joint Arthroplasty. J Arthroplasty. 2018 Jan;33(1):235-240. doi: 10.1016/j.arth.2017.08.011.
(8) Kahn TL, Schwarzkopf R. Does Total Knee Arthroplasty Affect Physical Activity Levels? Data from the Osteoarthritis Initiative. J Arthroplasty. 2015 Sep;30(9):1521-5. doi: 10.1016/j.arth.2015.03.016.
(9) Savarino L, Tigani D, Greco M, Baldini N, Giunti A. The potential role of metal ion release as a marker of loosening in patients with total knee replacement: a cohort study. J Bone Joint Surg Br. 2010 May;92(5):634-8. doi: 10.1302/0301-620X.92B5.23452.
(10) Friesenbichler J, Maurer-Ertl W, Sadoghi P, Lovse T, Windhager R, Leithner A. Serum metal ion levels after rotating-hinge knee arthroplasty: comparison between a standard device and a megaprosthesis. Int Orthop. 2012;36(3):539–544. doi: 10.1007/s00264-011-1317-4
(11) Jones, Dina L. et al. Differences Between Actual and Expected Leisure Activities After Total Knee Arthroplasty for Osteoarthritis. The Journal of Arthroplasty, Volume 27, Issue 7, 1289 – 1296. https://www.arthroplastyjournal.org/article/S0883-5403(11)00579-1/fulltext
(12) Peersman G, Laskin R, Davis J, Peterson M. Infection in total knee replacement: a retrospective review of 6489 total knee replacements. Clin Orthop Relat Res. 2001 Nov;(392):15-23. https://www.ncbi.nlm.nih.gov/pubmed/11716377
(13) Pabinger C, Berghold A, Boehler N, Labek G. Revision rates after knee replacement. Cumulative results from worldwide clinical studies versus joint registers. Osteoarthritis Cartilage. 2013 Feb;21(2):263-8. doi: 10.1016/j.joca.2012.11.014.
(14) Centeno C, Sheinkop M, Dodson E, et al. A specific protocol of autologous bone marrow concentrate and platelet products versus exercise therapy for symptomatic knee osteoarthritis: a randomized controlled trial with 2 year follow-up. J Transl Med. 2018;16(1):355. Published 2018 Dec 13. doi:10.1186/s12967-018-1736-8

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
