Meniscus Surgery Alternative: Please Read This First
I have blogged extensively about pursuing a meniscus surgery alternative since research years ago began showing that this surgery was not helping patients and may be harming them. Now new research also shows just how poorly this procedure works and how it’s likely pushing patients toward an earlier knee replacement. Let’s dig in.
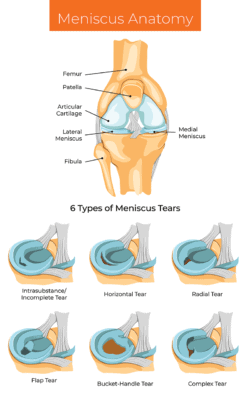
What is a Torn Meniscus?
The meniscus is a shock absorber that lives in the knee and protects the cartilage and bones. It has a figure-8 configuration and can be torn through wear and tear or trauma. A torn meniscus is usually found on an MRI, but there’s one problem about an MRI that shows a torn meniscus in someone who is 35 or older. We know from research that meniscus tears are very common in patients without knee pain, so simply seeing a meniscus tear on an MRI when someone has knee pain is not a valid way to diagnose that the meniscus tear is causing that pain (1).
The title of the above-referenced article, which reviewed the research on middle-aged meniscus tears said it all: “Degenerative meniscus tears should be looked upon as wrinkles with age–and should be treated accordingly”. Hence, one reason to pursue a meniscus surgery alternative is obvious, having a meniscus tear is about as common and meaningful as wrinkles on your face.
Can a Meniscus Tear Heal on its Own Without Surgery?
The meniscus has three zones, the red, red-white, and white. These are determined by the blood supply. Meniscus tears on the outer part of the tissue in the red zone which has a blood supply can heal. Those in the next deeper zone, the red-white, may or may not heal and the innermost white zone tears generally don’t heal on their own. However, as revealed above, for most patients, the fact that a meniscus tear was found on MRI shouldn’t be important.
Past Research Showing that Meniscus Surgery Doesn’t Work and Could be Harmful
The most common meniscus surgery is a partial meniscectomy. This means that the doctor removes the torn part of the meniscus. The New York Times puts this procedure into the “useless” category. Why?
A 2013 study demonstrated that meniscus surgery results couldn’t beat physical therapy (2). Then a study later that year demonstrated that meniscus surgery couldn’t beat a fake or sham surgery (3). Finally, a 2016 study put the final nail in the coffin for partial meniscectomy when it found that the surgery couldn’t beat placebo even for patients with locking symptoms due to a meniscus tear (4).
Then we have the research that shows that the surgery may be harmful to the knee. For example, we know that meniscus surgery alters the normal way a knee is built to move (5). We also know that the surgery is associated with more lost cartilage when MRI’s are taken one after the other (6). Finally, we know that knee arthritis is much more common in knees that have had meniscus surgery when compared to the opposite non-operated knee (7).
The New Research
In a 60-month study in persons over 45 years of age, the authors looked at how many patients went on to get a knee replacement (8). There were 351 randomized subjects who either had physical therapy or a partial meniscectomy to treat a meniscus tear. After 5 years, the meniscus surgery group was about 2 1/2 times more likely to get a knee replacement when compared to those patients who had physical therapy! If that’s not a reason to seek out meniscus surgery alternatives, I’m not sure what is…
Is There Anyone Who Should Get This Surgery?
As a physician who has seen hundreds of patients with meniscus tears over the last decade, I have referred only one for surgery. Why? His knee locking was very extreme and injecting orthobiologics didn’t work. Outside of that, all of our patients I have seen have been treated through injection without surgery. To understand what that’s about, see below.
Is There Another Option?
We have been treating meniscus tear patients with precise ultrasound-guided orthobiologics like their own platelets and bone marrow which contains their stem cells for more than a decade. This is a legitimate meniscus surgery alternative. Many of these patients recover without ever having considered surgery. Here’s what that procedure looks like:
The upshot? The research is very clear, you should be looking for a meniscus surgery alternative. We have a slew of high-quality research studies that show that meniscus surgery has been shown to be ineffective and likely leads to a more rapid progression of arthritis. There are newer injection-based techniques to help promote healing in the meniscus without surgery.
____________________________________________________
(1) Degenerative meniscus tears should be looked upon as wrinkles with age—and should be treated accordingly.
(2) Katz JN, Brophy RH, Chaisson CE, et al. Surgery versus physical therapy for a meniscal tear and osteoarthritis [published correction appears in N Engl J Med. 2013 Aug 15;369(7):683]. N Engl J Med. 2013;368(18):1675–1684. doi:10.1056/NEJMoa1301408
(3) Sihvonen R, Paavola M, Malmivaara A, Itälä A, Joukainen A, Nurmi H, Kalske J, Järvinen TL; Finnish Degenerative Meniscal Lesion Study (FIDELITY) Group. Arthroscopic partial meniscectomy versus sham surgery for a degenerative meniscal tear. N Engl J Med. 2013 Dec 26;369(26):2515-24. doi: 10.1056/NEJMoa1305189.
(4) Sihvonen R, Englund M, Turkiewicz A, Järvinen TL; Finnish Degenerative Meniscal Lesion Study Group. Mechanical Symptoms and Arthroscopic Partial Meniscectomy in Patients With Degenerative Meniscus Tear: A Secondary Analysis of a Randomized Trial. Ann Intern Med. 2016 Apr 5;164(7):449-55. doi: 10.7326/M15-0899.
(5) Netravali NA, Giori NJ, Andriacchi TP. Partial medial meniscectomy and rotational differences at the knee during walking. J Biomech. 2010 Nov 16;43(15):2948-53. doi: 10.1016/j.jbiomech.2010.07.013.
(6) Cohen SB, Short CP, O’Hagan T, Wu HT, Morrison WB, Zoga AC. The effect of meniscal tears on cartilage loss of the knee: findings on serial MRIs. Phys Sportsmed. 2012 Sep;40(3):66-76. doi: 10.3810/psm.2012.09.1983.
(7) Longo UG, Ciuffreda M, Candela V, Rizzello G, D’Andrea V, Mannering N, Berton A, Salvatore G, Denaro V. Knee Osteoarthritis after Arthroscopic Partial Meniscectomy: Prevalence and Progression of Radiographic Changes after 5 to 12 Years Compared with Contralateral Knee. J Knee Surg. 2019 May;32(5):407-413. doi: 10.1055/s-0038-1646926.
(8) Katz JN, Shrestha S, Losina E, Jones MH, Marx RG, Mandl LA, Levy BA, MacFarlane LA, Spindler KP, Silva GS; MeTeOR Investigators, Collins JE. Five-year outcome of operative and non-operative management of meniscal tear in persons greater than 45 years old. Arthritis Rheumatol. 2019 Aug 20. doi: 10.1002/art.41082.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.