The Blind Leading the Blind… We Have an Academia Regen Med Problem
We have a big problem looming in regenerative medicine. There is a serious lack of knowledge in academia about the science, and more importantly a lack of clinical experience. This means that much of the published research studies in this area often have rookie mistakes that negatively impact the field. I’ll give a few examples this morning and a few suggestions on how this gets fixed.
Some Concrete Examples: The Mayo Clinic Knee Arthritis Trial Debacle
We have two randomized controlled trials (RCTs) on the use of bone marrow concentrate (a same-day stem cell injection procedure) to treat knee osteoarthritis, one published by a Mayo clinic author and one published by our group. The first one didn’t find that it worked better than saline and ours showed that our same day stem cell procedure was superior to the control group. However, if you look at the two trials, they are completely different and the Mayo Clinic research suffered from a fatal flaw.
Why is the Mayo Clinic knee stem cell study bad? We’ve known since the 90s and early 2000’s due to studies by Hernigou that the dose of bone marrow concentrate is incredibly important in determining the outcome of the treatment. Meaning if you don’t have a high enough dose of stem cells in the mix, the therapy fails. In our RCT we made sure that the processing would maximize the dose of stem cells. In the Mayo trial, they diluted the dose severely and reported cell numbers that would be a fraction of what we found was needed to help knee arthritis. Why did they do this? My guess is that whoever designed the study had never read Hernigou’s or our work.
Poisoning Tendons with Lidocaine
Here’s another example from just this past week. A new tendon study was making the rounds on Linkedin. It compared a lidocaine injection versus a platelet-rich plasma injection to treat elbow tendinitis. Despite a prior and much larger randomized controlled trial showing efficacy for this PRP procedure, this one didn’t show that PRP was better than just lidocaine. However, there was likely a reason for that result based on another academic bone head move. Let me explain.
We’ve known for quite a while that common local anesthetics like lidocaine and marcaine can kill cells. Our research group published the most comprehensive study of its kind on this topic focusing on mesenchymal stem cells. What it found was that lidocaine, which is a common local anesthetic, kills stem cells dead. For example, at half of full strength (0.5%), it killed 95% of the stem cells (graph C below). Even at quarter strength (0.25% or graph B below), it killed approx. 70% of stem cells!
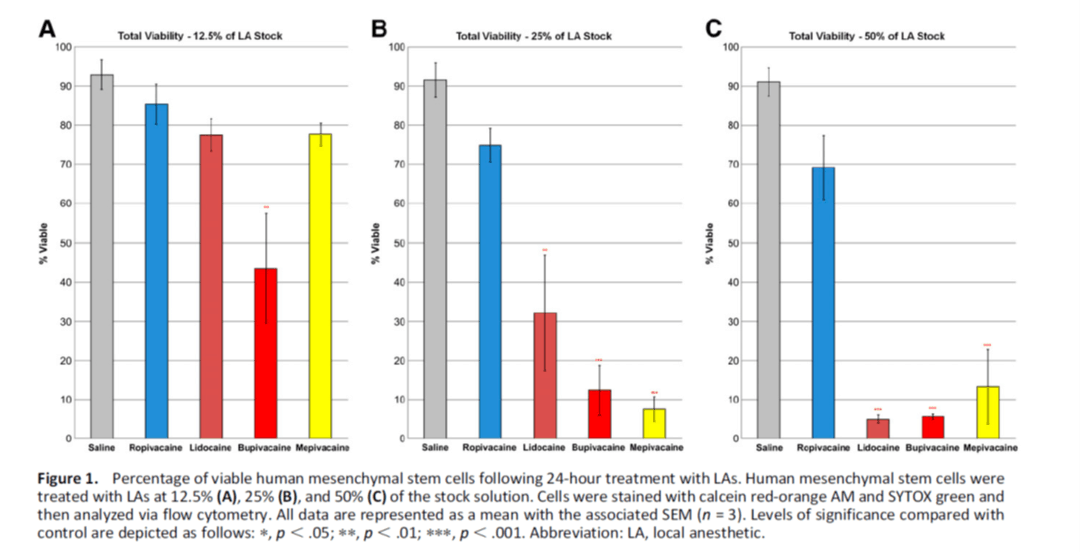
So what was the bone head move in this new study? They used lidocaine to numb the tendon in the PRP group! That means that they killed off the stem cells in that tendon before applying the PRP. How does PRP work? By stimulating local stem cells to repair tissue. Hence, they created a non-working PRP study arm by mistake, all because some academic physician never got the memo that lidocaine kills stem cells. What could they have used? Dilute Ropivacaine would have done the trick (see graphs above).
Houston, We Have a Regen Med Academia Problem…
The problem we have is that there is no formal medical school, residency, nor fellowship training in regen med. Hence, whatever these academic physicians learn about this topic is what can be found at courses. However, most of those weekend courses are “pay for play”, meaning that the content is often controlled by or at least heavily influenced by vendors trying to sell something. Hence, the science presented is often filtered through the lens of sales and not what really works.
There’s another HUGE issue. Because these procedures are not yet covered by insurance, many academic physicians can’t use them in their daily practices or if they do, that use is few and far between. Hence, they lack the basic clinical experience that provides an observational evidence base. That’s critical for knowing which therapy likely works best for which condition. Despite this, they are often asked to design clinical trials, which is truly the blind leading the blind. For example, how would you know which therapy to use in a randomized controlled trial if your sum total of experience with that technology is 20 cases over two years? Worse yet, when you have never before used that technology in patients! In fact, you would only be qualified to design that trial if you had treated hundreds of patients with that technology.
How do we fix this? We need to get regen med training in medical schools. In addition, everyone from students to professors must take these courses to catch up with the what’s been published. We need this ASAP.
The upshot? These are just a few of the problems I’ve seen that are caused by a lack of understanding by academics of “which end is up” in regenerative medicine. Before we have a slew of bad studies published with rookie mistakes that destroy the promise of the field, we desperately need to make sure that academic physicians learn what they don’t know.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.