When Is PRP not PRP? It All Depends on Your Age
If you read this blog, you know quite a bit about PRP now. However, there continue to be studies performed that say they use PRP, but it’s really not PRP. Today we’ll review that issue so you can learn what to avoid. Let’s dig in.
What Is PRP?
PRP stands for Platelet-Rich Plasma. This is a mix of concentrated platelets that are often injected to help damaged musculoskeletal tissues heal. This works through the growth factors contained in the platelets which help act as espresso shots for the local repair cells to do more work.
As you have read here, injectable PRP comes in two flavors: red leukocyte rich (LR) and amber leukocyte poor (LP). The red stuff contains lots of red and white blood cells and tends to be pro-inflammatory and the amber stuff lacks red and white blood cells and is less inflammatory. Hence, most doctors now favor using amber PRP and this is mostly supported by the research out there as being more effective.
Yet another property of PRP you need to understand is concentration or dose. This is less of an issue if you’re young and a much bigger deal if you’re middle-aged or older. For example, our published research shows that as you age, your cells respond much better to high-dose PRP. Let’s dig in on that concept.
High-Dose PRP
Way back in 2005, we began using Platelet Lysate to help grow stem cells in culture. A Platelet Lysate is made from PRP by breaking open the platelets to get all of the growth factors out. One of the things we quickly noticed was that for young patients, it didn’t matter how concentrated we made the Platelet Lysate, as those cells grew well with low or high dose (made with fewer or more platelets). However, for middle-aged and older patients, we observed that high-dose Platelet Lysate caused much more cell growth. We confirmed this phenomenon with our own in-house studies and then published on this phenomenon (1).
Why does it work this way? That younger people don’t need lots of platelets to spark cell activity while older people need more? Let me explain why this likey happens with a bunch of illustrations I drew for you this morning.
First, let’s learn how growth factors work to promote cells to grow or repair. We all have growth factors (GFs) in our blood. We have more of these when we’re young and fewer of these molecules when we’re older. This is why you see that most NFL athletes retire by their mid-30s. This is because their bodies can no longer naturally keep up with the wear and tear from the game due to declining GF levels. These lower levels mean slower repair and an increased recovery time.
How Do GFs Help Cells Grow or Repair?
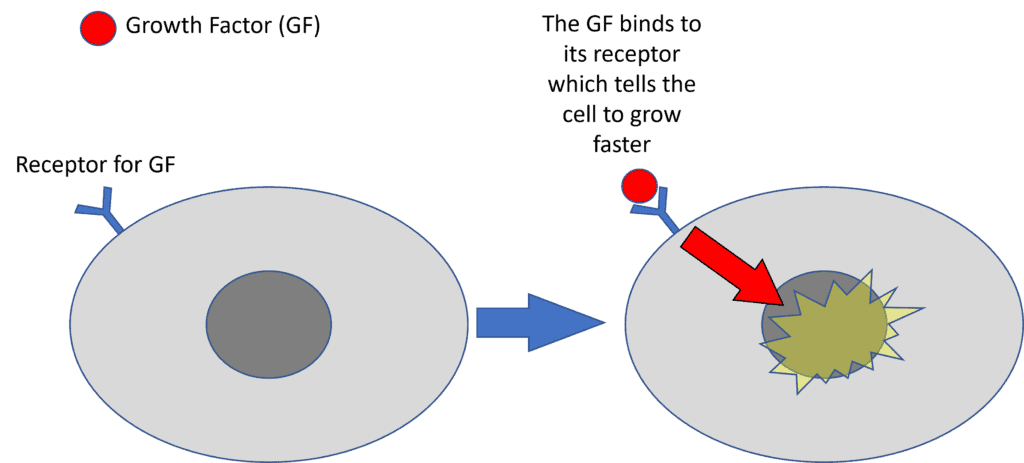
How does this work? In the illustration above, the GF needs to bind to the cell as shown above to signal it to grow faster or stimulate repair. I often explain this to patients using a Starbucks analogy. If I go and buy a bunch of espresso shots for a construction crew, they’ll get more work done. Hence, think of GFs like espresso shots.
Note that there are many different types of GFs that tell cells to do different things and each GF has its own specific receptor on a specific cell type. In the illustration above, note that the GF binds to the specific receptor (here shown as a “Y”) which gives the cell the message to grow faster or repair something.
Young Cells
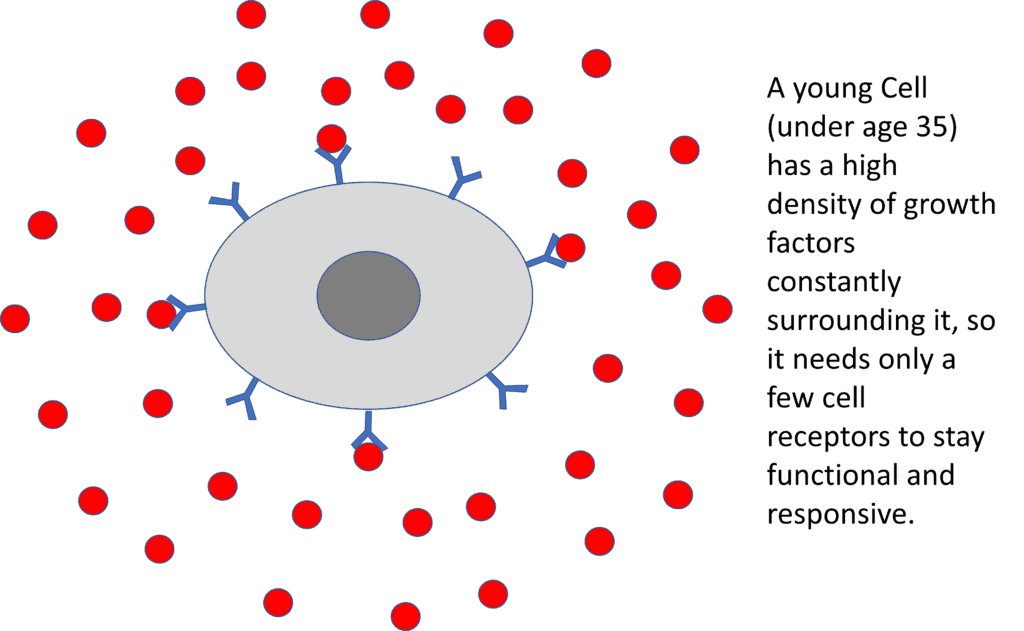
Getting back to our NFL player analogy, when we’re young, we have lots of GFs floating around, as a result, our cells need few receptors for them (see above). This is a well-known phenomenon in cell biology – that the cells downregulate receptors (make fewer) when they’re not needed (4).
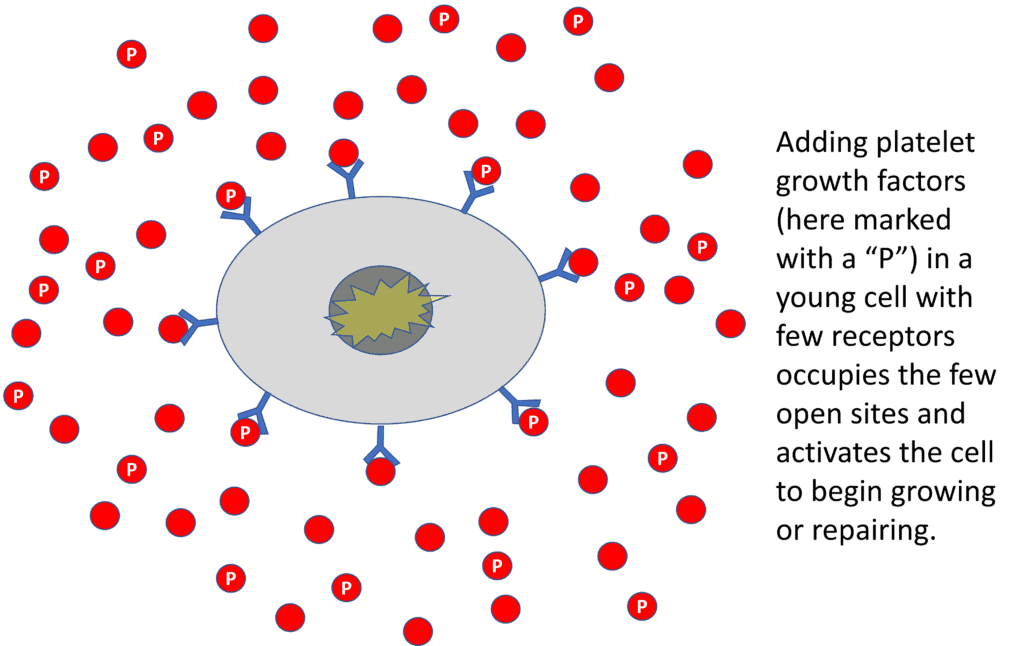
In that same young cell scenario, above I show what happens when you inject low-dose PRP. The few open receptor sites get occupied by the platelet GFs (here shown by a red circle with a “P”) and the cell is activated for growth or repair.
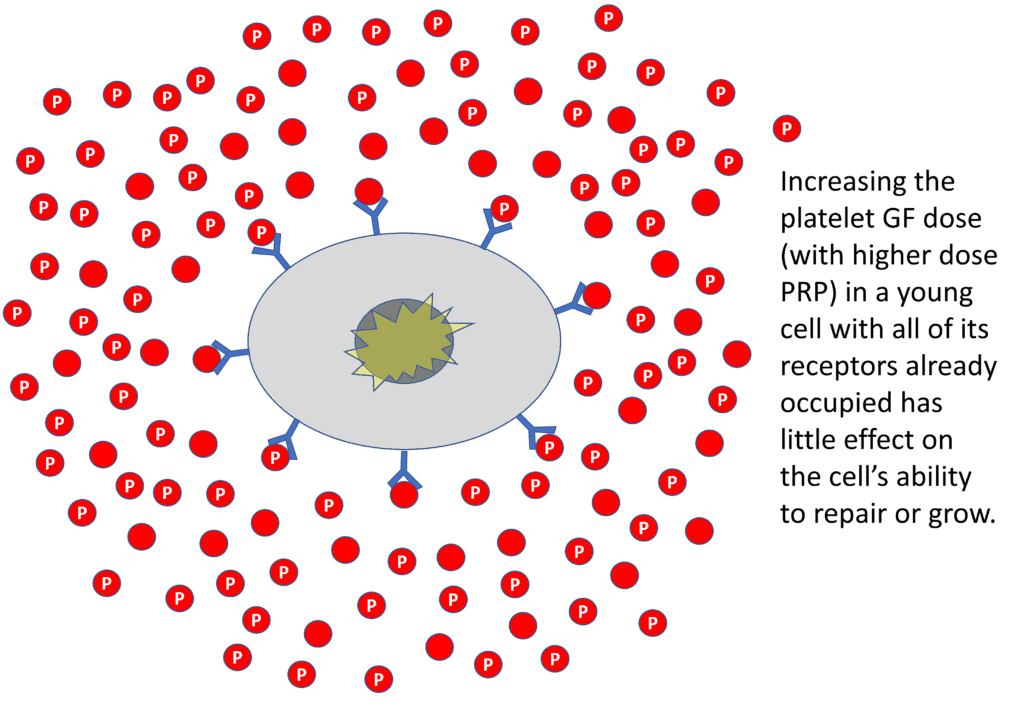
In the above illustration, I have now dramatically increased the number of platelet GFs by upping the platelet concentration in PRP (more red circles with a “P”). Again, since this is a young cell, I had already saturated the receptors with low dose PRP, so adding more platelet GFs doesn’t move the repair signal needle. Meaning, there are no more open receptors to be activated.
So what did we learn? Since young cells have few receptors for platelet growth factors, you can easily saturate them and get them to repair or grow with low concentrations of PRP. Upping the PRP concentration in this group of patients does little to further stimulate cell repair or growth.
Old Cells

Now let’s look at middle-aged and older cells. These live in a GF poor environment. Hence, the body up-regulates the number of GF receptors on the cell surface to be able to detect the rare natural growth factors. Note how many more receptors are on this old cell.
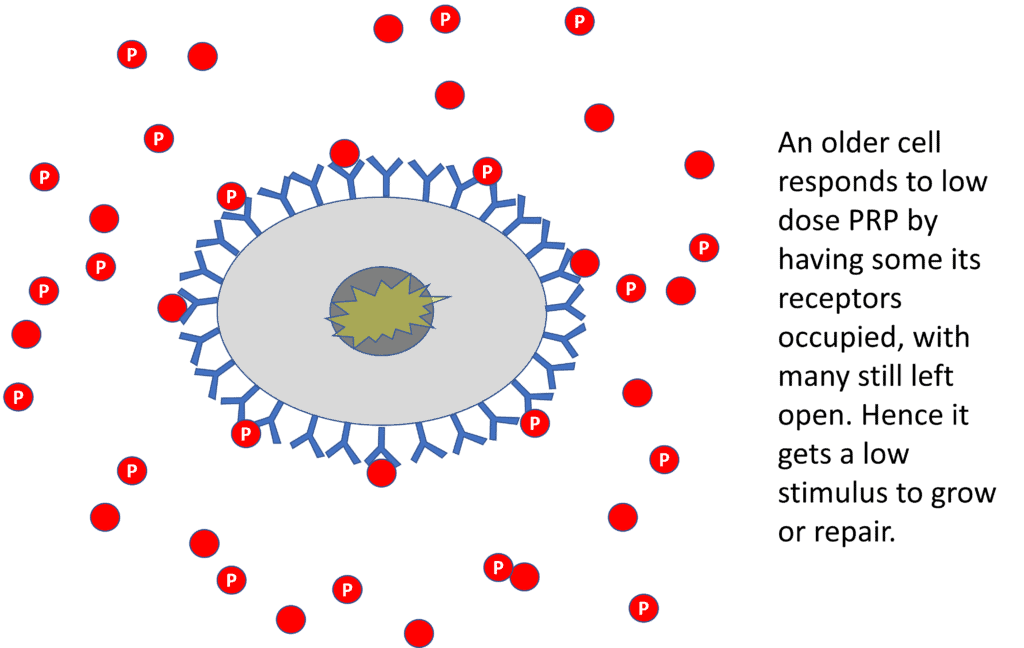
So what happens when we inject low-dose PRP around an old cell? Some of the many receptors get occupied and it provides a low-level stimulus for repair or growth.
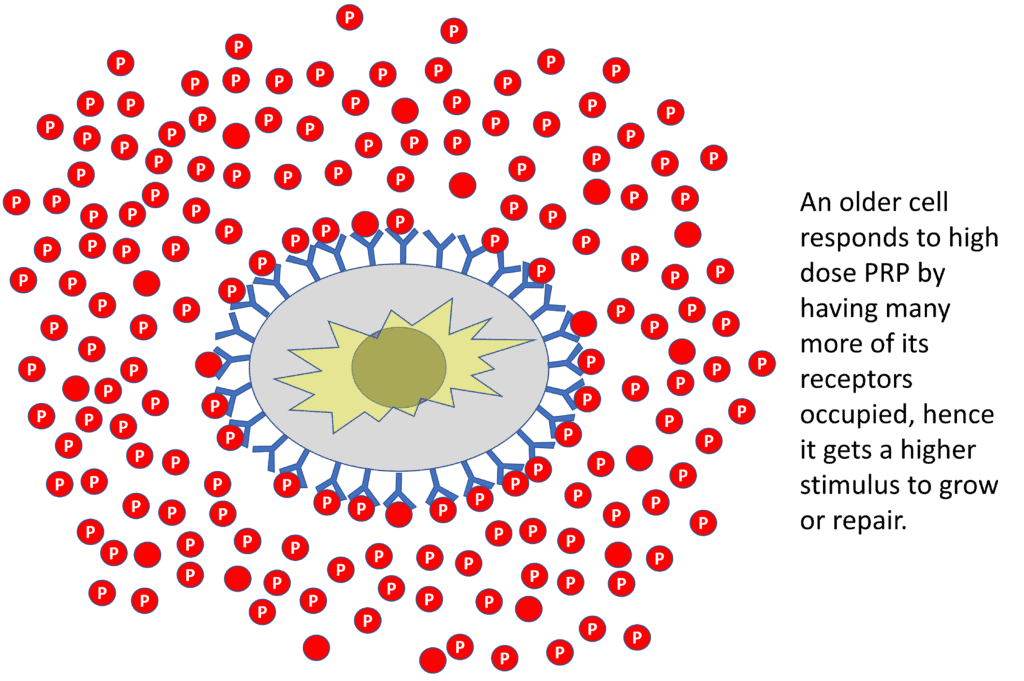
What happens when we inject high-dose PRP around older cells? Now, many more receptors are occupied and hence there’s a greater stimulus for repair or growth! In this scenario, we get way more bang for our buck.
So what did we learn? Old cells respond completely differently to high-dose PRP. There is a direct relationship between higher doses and more repair or growth because they have more receptors that can be stimulated. Hence, using low-dose PRP in these patients is a bad idea.
In fact, this figure from our recent publication on this phenomenon tells us that if you up the dose of PRP in older patients, you get a direct increase in cell activity, but that this doesn’t work in younger patients:
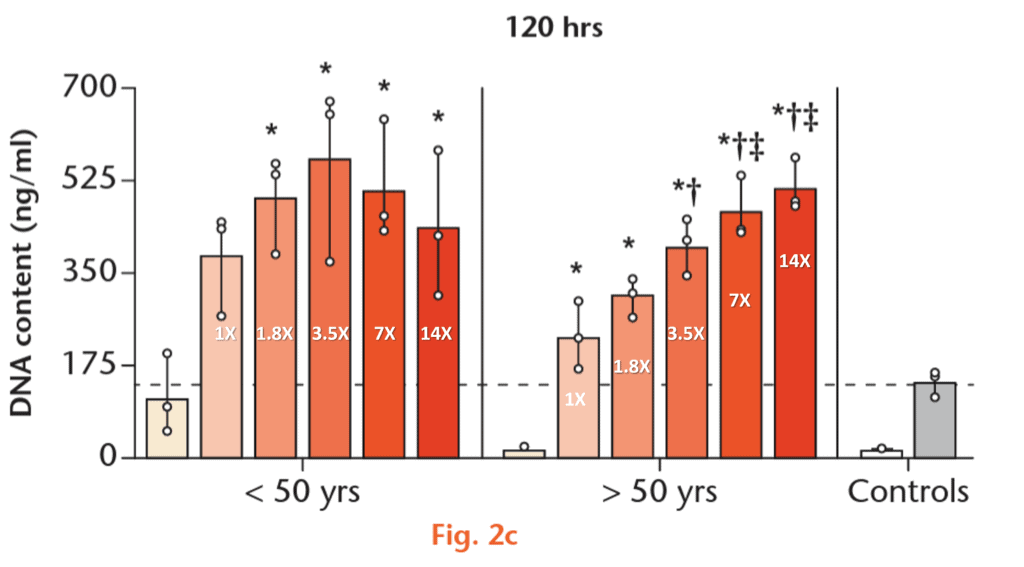
So When Is PRP NOT PRP?
As shown, for younger cells, it doesn’t take a high concentration of platelets to get an effect. In fact, based on our lab data, 2 times concentration (2X) will cause most cells to grow or repair. Hence, for a young person, PRP can be 2-3X and still help their injuries. However, in an older patient, all of that changes. Now, 2-3X PRP only produces a small effect. Hence, in middle-aged people (35-45), we commonly use 5-7X concentration. In older people (45-70), we’ll up that concentration to 10-14X. In the older elderly (75+) we’ll up that to 20X.
Hence, the answer to “When is PRP not PRP?” depends on the age of the patient. To illustrate that point let’s look at a recent study.
The New Flawed PRP Ankle Research
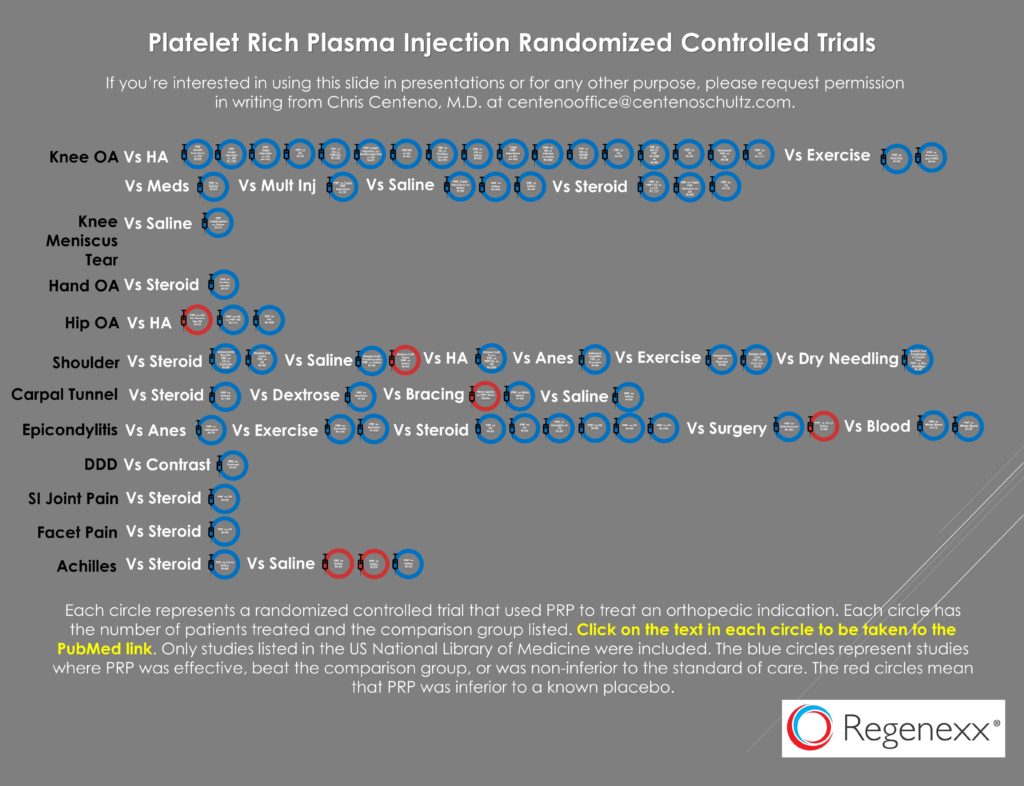
Recently, researchers in the Netherlands and the Middle East performed a Randomized Controlled Trial of ankle PRP injections to treat arthritis symptoms (2). They injected 100 patients with PRP or saline and then looked at the outcome in these groups and couldn’t find a difference between the two groups and thus concluded that PRP didn’t help ankle arthritis. However, that conclusion doesn’t square with all of the studies shown below:
Each circle here is a study. To see that study, click on the image to be taken to PDF with live links for each icon. The blue circles represent studies showing that PRP was better than what was tested in the same RCT format. Hence, lots of data show that PRP works to help various types of arthritis and other issues.
So why did it fail here? A closer look at the study shows that these patients were in their mid-fifties, prime candidates for needing high-dose PRP. What was injected? Regrettably, they used an Arthex ACP system which has been tested to produce to very low dose PRP (2-3X at best) (3). Hence, they severely under-dosed these patients and as a result, likely observed poor results.
What You Should Do as a Patient
You NEED to ASK your doctor about platelet-dose. If they can’t tell you exactly what platelet dose they’re using and why then you need to find another doctor. At Regenexx, our physicians all adjust the dose based on your age and can create much higher doses in their flexible in-house labs than almost all physicians out there that use simple bedside systems.
The upshot? Platelet dose matters. If you’re middle-aged or older, getting low-dose PRP is a prescription for poor results. This phenomenon of dose and age likely explains the few studies that show that PRP doesn’t work while most show it works well. Make sure you understand why you need a higher dose and make sure you discuss this with your doctor!
_________________________________________________
References:
(1) Berger DR, Centeno CJ, Steinmetz NJ. Platelet lysates from aged donors promote human tenocyte proliferation and migration in a concentration-dependent manner. Bone Joint Res. 2019 Feb 2;8(1):32-40. doi: 10.1302/2046-3758.81.BJR-2018-0164.R1. PMID: 30800297; PMCID: PMC6359887.
(2) Paget LDA, Reurink G, de Vos RJ, Weir A, Moen MH, Bierma-Zeinstra SMA, Stufkens SAS, Kerkhoffs GMMJ, Tol JL; PRIMA Study Group. Effect of Platelet-Rich Plasma Injections vs Placebo on Ankle Symptoms and Function in Patients With Ankle Osteoarthritis: A Randomized Clinical Trial. JAMA. 2021 Oct 26;326(16):1595-1605. doi: 10.1001/jama.2021.16602. PMID: 34698782.
(3) Magalon J, Bausset O, Serratrice N, Giraudo L, Aboudou H, Veran J, Magalon G, Dignat-Georges F, Sabatier F. Characterization and comparison of 5 platelet-rich plasma preparations in a single-donor model. Arthroscopy. 2014 May;30(5):629-38. doi: 10.1016/j.arthro.2014.02.020. PMID: 24725317.
(4) Science Direct. Upregulation. https://www.sciencedirect.com/topics/medicine-and-dentistry/upregulation Accessed 11/7/21

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.