Are You Getting Ripped Off by Paying for a Low Dose PRP Shot?
One of the biggest issues for anyone getting a PRP injection is whether it’s the proper concentration to maximize the outcome. But how can you, as a patient, quickly check to see if you’re getting PRP that meets that spec? Today I’ll teach you how to quickly recognize if you’re getting ripped off.
My Conversation While Hiking
An older woman I know stopped me the other day while I was hiking my dogs because she wanted to know more about PRP treatment for her knees. She had been getting OK results from PRP injections through another clinic and wanted to know how to optimize those benefits. One of the things I quickly realized was that I had no good way to discuss a critical component of looking at the quality of the PRP injections she was getting.
As I’ve discussed in past blogs, there are many factors to consider when looking at the quality of a PRP injection. A few of these include:
- Locations treated
- Use of imaging guidance
- Type of PRP
- Dose
It’s that last part about the proper dose that was difficult to discuss, as she had no idea which bedside machine this clinic was using. Then it struck me that there was an easy way for her to measure whether she was getting the proper dose in her knees. She just needed to pay attention to how much blood they drew. Let’s dig into that concept.
What is PRP?
PRP stands for platelet-rich plasma. This is created by taking whole blood, commonly from a vein in the arm, and then centrifuging the blood. That process concentrates the platelets in plasma. These platelets contain healing growth factors and exosomes that can assist in tissue healing. For the treatment of knee arthritis, we have dozens of Randomized Controlled Trials showing that PRP is effective.
Does Concentration Matter?
Way back in 2005, long before the vast majority of providers had heard of PRP or stem cells as treatments for orthopedic problems, we began using autologous Platelet Lysate (PL) to help grow bone marrow mesenchymal stem cells in culture. PL is made from PRP by “lysing” (breaking open) the platelets to get all the growth factors out. One of the things we quickly observed was that for young patients, it didn’t matter how concentrated we made the Platelet Lysate; those cells grew well with low or high dose PL (made with fewer or more platelets). However, for middle-aged and older patients, we consistently noted that high-dose Platelet Lysate caused much more cell growth. We confirmed this phenomenon with our in-house studies on MSCs and then on tenocytes and then published on this phenomenon (3). Others publishing in the field of using PRP to treat knee arthritis have found the same dose-efficacy relationship (4).
To learn more about this topic of PRP dose and the existing research, see my video below:
PRP Dose and Age
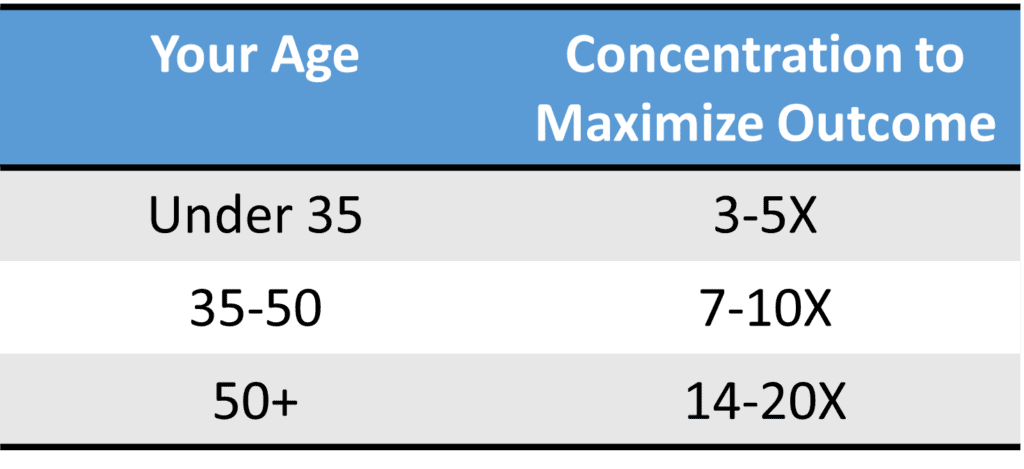
How high a PRP dose do you need as you age? The above table was created by my observations of our in-vitro data, our published work on young vs. old tenocytes, and my almost two-decade clinical experience. There is a more detailed discussion available of why I believe this direct PRP dose-response relationship happens as we age and why it doesn’t apply while we’re young.
If you’re young, you don’t need high-dose PRP. In fact, just 2-3X PRP will be fine (I have 3-5X above to account for the fact that most of our patients in this group are in their early 30s). Even if you get treated with one of the really bad PRP systems that produce blood products as low as 1.5X platelets (which doesn’t even meet the 2X definition of PRP), that will probably work in some young people. However, this totally changes for middle-aged and older people. Now dose becomes critical.
The above table shows estimates to maximize PRP outcome versus dose. Realize that some people will still respond at lower doses than listed, but most people would need the doses shown to maximize their response. The good news is that as you age, there is no scientific maximum that we have detected. Meaning if you treat a 45-year-old with 20X PRP, that will still provoke a more significant response than 10X, but not as big a response as you would see in a 60-year-old.
Having said that, there are some serious practical considerations here. Meaning that once you get to 14-20X, the amount of blood you need to draw to get 10-20 cc of injectate gets prohibitively large. Hence, for example, we often flex some of these concentrations down in older patients to make sure we’re not taking multiple blood bags from a single patient. For example, in my clinical experience, most of the time, 10X PRP works very well in older tendons.
Because of all of this, there’s another key quality metric here that you can look for in a clinic which is the use of a finger-stick hematocrit machine. That device takes a drop of blood to determine the patient’s blood concentration (hematocrit/hemoglobin levels). This allows the doctor to see how much is “in the tank” to ensure that too much blood is never drawn. At Regenexx, we have a blood loss calculator that our affiliates use to plug in weight, sex, hemoglobin levels, and the concentrations the doctor ordered to flag situations when too much blood is required.
Simple Math and a Table to Check the PRP Dose You’re Getting
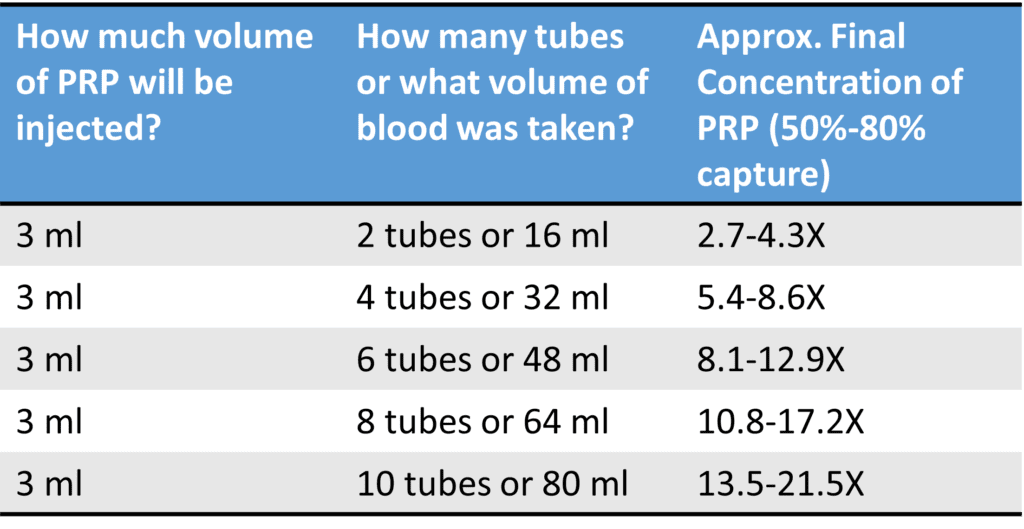
Credit: Author
The table above was created for a 3 ml injection of PRP to keep it simple. That would be enough to inject a single large joint like a knee, hip, or shoulder. Obviously, the final PRP volume may be higher if you’re getting more injected (like both knees, multiple areas, or tendons/ligaments) or lower if you’re getting just a small joint injection, like one or more fingers or spinal facet joints.
The math behind the table is also simple. You take the platelets in the volume of collected whole blood and then concentrate those down to your final volume. If there were 100% efficiency in collecting platelets, that would give you the final concentration. So 12 ml of whole blood concentrated down to 3 ml of PRP would be 4X or four times more concentrated platelets in the PRP than in the whole blood. However, the efficiency of the platelet capture is never 100%.
Figuring out the platelet capture efficiency of a specific bedside system used by your doctor requires homework. However, to get rid of the idea that you need to hunt this down for every machine, based on the existing peer-reviewed literature, a bad system is about 50% efficient, and a good system can be around 80% (1,2). Hence, I quoted that range of concentrations in the table, with the low end being 50% platelet capture and the high end being 80%.
How to Use this Table
This is where we get back to our older woman with knee arthritis on the hiking trail who wants to stay active. If she goes to the doctor to get a PRP shot in her arthritic knee, she would need to have about 3 ml of 14-20X PRP injected inside the joint (intra-articular). Looking at our table above, that means she needs to have ten tubes or 80 ml of blood drawn. So what happens if the doctor’s office only draws four tubes? Looking at our table, that would only produce about 5-9X PRP, reducing the likelihood of the maximum possible outcome for her money. Hence, she needs to find another doctor.
Obviously, if she’s getting more injected, she needs to get more blood taken. For example, she mentioned that she wanted both knees treated and that she usually gets various ligaments/tendons in her knees injected. Hence, let’s say that she is treated with 10cc of 14X PRP. To get that amount and dose, the doctor’s office would need to take 34 tubes or a little under 300 ml of blood. That’s just a little shy of the standard blood bag, like the type used if you donated blood at a qualified blood bank.
The upshot? While there are many things that go into researching whether or not you got a quality PRP injection, a simple one you can quickly figure out is the dose. This is critical for middle-aged to older patients and much less important for young people. Hence, if you’re older, pay attention to how much blood is being drawn and use the tables above to determine whether you’re getting a high-quality PRP injection for your money!
____________________________________________________________
(1) Magalon J, Bausset O, Serratrice N, Giraudo L, Aboudou H, Veran J, Magalon G, Dignat-Georges F, Sabatier F. Characterization and comparison of 5 platelet-rich plasma preparations in a single-donor model. Arthroscopy. 2014 May;30(5):629-38. doi: 10.1016/j.arthro.2014.02.020. PMID: 24725317.
(2) Degen RM, Bernard JA, Oliver KS, Dines JS. Commercial Separation Systems Designed for Preparation of Platelet-Rich Plasma Yield Differences in Cellular Composition. HSS J. 2017 Feb;13(1):75-80. doi: 10.1007/s11420-016-9519-3. Epub 2016 Aug 19. PMID: 28167878; PMCID: PMC5264574.
(3) Berger DR, Centeno CJ, Steinmetz NJ. Platelet lysates from aged donors promote human tenocyte proliferation and migration in a concentration-dependent manner. Bone Joint Res. 2019 Feb 2;8(1):32-40. doi: 10.1302/2046-3758.81.BJR-2018-0164.R1. PMID: 30800297; PMCID: PMC6359887.
(4) Bansal, H., Leon, J., Pont, J.L. et al. Platelet-rich plasma (PRP) in osteoarthritis (OA) knee: Correct dose critical for long term clinical efficacy. Sci Rep 11, 3971 (2021). https://doi.org/10.1038/s41598-021-83025-2

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.