Do I Need Surgery for Cervical Stenosis? Will I Become Paralyzed?
One of the questions that I get asked often is “Do I need surgery for cervical stenosis?”. I often hear from my patients with cervical stenosis that some spine surgeon told them that the risk of becoming paralyzed with a routine fall means they need surgery right now! This is personal for me, as I have tight cervical stenosis and have chosen not to have surgery. So can cervical stenosis cause paralysis and what are the odds of this really happening? Let’s dig in.
What is Cervical Stenosis?
Your spinal cord goes through the neck bones. That hole for the spinal cord is called the central canal and it can get smaller making it a tight fit for the cord. That can happen due to disc bulges, bone spurs, arthritic facet joints, or enlarged and swollen ligaments. You can even be born with a tight central canal. See my video below for an explanation of how that works:
This tightness can irritate the spinal cord and lead to all sorts of symptoms. Everything from numbness, tingling, weakness, or aches and pains elsewhere. When this happens, this is called symptomatic spinal stenosis. This is when patients begin to ask the question, “Do I need surgery for cervical stenosis?”
Selling Surgery
I don’t know how many patients I have seen through the years who have told me that a spine surgeon claimed that if they didn’t get neck surgery sooner rather than later, they could become paralyzed from a simple fall. Yesterday, I had a patient who recognized me at our local Whole Foods. He relayed that a surgeon at a famous Colorado sports medicine clinic told him that this is why he needed surgery. Despite everything I know, what ran through my mind in a split second was that I have stenosis in my neck and could this happen to me? After all, I was about to get into my car! Meaning this stuff is scary, even for a physician. So I thought to myself, do I need surgery for cervical stenosis? Have I been fooling myself by avoiding surgery? Can cervical stenosis cause paralysis often enough for me to want neck surgery?

What are the Odds of Paralysis?
My sense from practicing medicine for several decades and never having seen one of my own severe cervical stenosis patients become a quadriplegic from a fall was that this risk was very small. However, despite searching this in the past a few times on the US National Library of Medicine, I had never seen a study that directly addressed this issue. However, yesterday I finally found a few that answered this question. So can cervical stenosis cause paralysis, or just a surgical sales pitch?
First, in 2006, someone actually attempted to calculate the risk of becoming paralyzed from an injury just because there was severe spinal stenosis. After an extensive review of multiple demographic and medical databases, they put that “worst case scenario” (likely overestimate) risk at 1:2100 (1). However, the risk of surgical neck decompression is far worse (2). In fact, serious complications vary from approximately 1 in 200 for spinal cord or nerve root injury to 1 in 100 for infection to 1 in 7 for “Adjacent Segment Disease”. Hence, you are about 10-20 times more likely to be seriously injured by neck surgery than you are by falling and becoming paralyzed! As a result of this, the authors of a recent analysis on the topic concluded that there was no evidence to support surgery to decompress the spinal cord to prevent possible paralysis from a fall. (3). Meaning, the answer to the question, “Do I need surgery for cervical stenosis?” in this analysis was a resounding “No”.

How Do Other Real World Odds Compare?
If the odds of cervical stenosis causing paralysis are generously 1 in 2,100, how does that compare to common risks? Below is a table that shows all of the things you’re more likely to die from in your life time than get paralyzed from a fall (4):
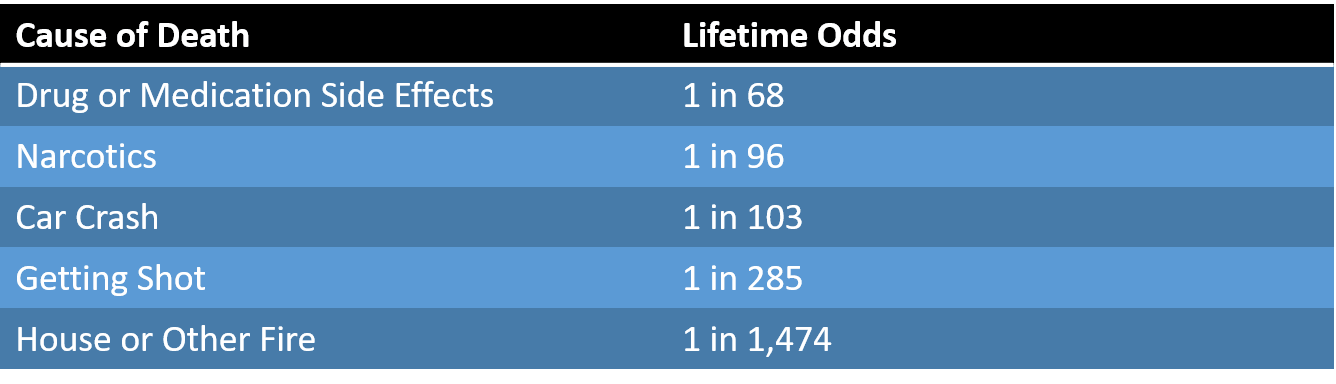
Again, you are 20 times more likely to die in a car crash than become paralyzed from a fall!
The upshot? The idea that you need neck surgery to decompress your spinal cord if you have neck stenosis because you may become paralyzed in a fall is ridiculous. This assertion is NOT supported by any scientific review of the data. As shown, you are far more likely to get killed by all sorts of stuff, including driving to the grocery store than becoming paralyzed this way. More importantly, the risk of the surgery making you paralyzed or seriously injuring you is far greater than the risk from a fall. Hence, note to my surgical colleagues, please STOP the surgery scare (sales) tactics! In addition, note to patients, if you’re asking the question, “Do I need surgery for cervical stenosis?” and your reasoning (like my patient) is to avoid becoming paralyzed, you don’t need surgery.

_____________________________________
References:
- Lauryssen, C., K. D. Riew, and J. C. Wang. “Severe cervical stenosis: Operative treatment of continued conservative care.” Spine Line 8.1 (2006): 21-5. https://www.ncbi.nlm.nih.gov/pubmed/22082636
- Cheung, Jason Pui Yin, and Keith Dip-Kei Luk. “Complications of Anterior and Posterior Cervical Spine Surgery.” Asian spine journal vol. 10,2 (2016): 385-400. doi:10.4184/asj.2016.10.2.385
- Murphy, Donald R et al. “Cervical spondylosis with spinal cord encroachment: should preventive surgery be recommended?.” Chiropractic & osteopathy vol. 17 8. 24 Aug. 2009, doi:10.1186/1746-1340-17-8
- Insurance Information Institute: https://www.iii.org/fact-statistic/facts-statistics-mortality-risk
If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.