Living With a Subtalar Fusion: Do You Really Need Surgery?
On this page:
- What is the subtalar joint?
- What is subtalar arthritis?
- What is a subtalar fusion?
- Are ankle fusions successful?
- Can subtalar arthritis be treated without ankle fusion?
- Can you treat the subtalar joint with orthobiologics?
- How many patients can avoid a subtalar fusion?
The subtalar joint is sort of the red-headed stepchild of the ankle. Most of the focus is usually on it’s bigger brother, the main tibiotalar joint. However, arthritis in the smaller subtalar joint can cause loads of pain and disability. That pain can lead some patients to consider subtalar fusion. However, do you really need this surgery? Let’s dig in.
What Is the Subtalar Joint?
The joint below your main ankle joint (tibiotalar) is called the subtalar joint. This is a complex of three different small joints (facets) as shown here. The subtalar joint helps adjust the heel and foot side to side as you walk on uneven ground.
What Is Subtalar Arthritis?
Arthritis happens when the joint surfaces become damaged. The subtalar joint has cartilage that helps to cushion the joint and when that becomes injured, the joint can become painful and develop bone spurs. The pain is usually felt in the back of the foot on the outside, but it can also be felt on the inside. Normally this is an aching in the area of the joint (below the main ankle joint) after activity.
What Is a Subtalar Fusion?
Subtalar fusion is when the doctor takes screws or plates and makes the subtalar joint unable to move (fused). The goal is to get rid of the pain by not allowing any movement of the area (1).
How long are you non weight bearing after an ankle fusion? How long does it take for a subtalar fusion to heal? Can you run after subtalar fusion?
It will be 1 1/2 to 4 months before you can put full weight on the leg. Full healing and resuming normal activities will take about a full year.
Running after an ankle fusion is not advised. Why? Placing the forces on the ankle that will happen with running will overload the joints above and below. That means that joints like the main ankle joint (tibiotalar) and the talonavicular will get arthritis more quickly due to the fusion. This is called “Adjacent Segment Disease” (ASD). In fact, in many patients, over time, even without running, ASD will still happen (2).
Are Ankle Fusions Successful?
Will an ankle fusion eliminate pain? Are foot fusions successful? We have no high-level research that shows this procedure works. That means that the procedure hasn’t been compared to a faked surgery to see if it’s more successful than a placebo. But in one early study, the complication rate was a staggering 48% (3)!
In my clinical experience, while the subtalar joint usually stops hurting after the procedure, the biggest issue I see long-term is ASD. That usually takes the form of arthritis in the tibiotalar joint above or in the joints below (i.e. like the talonavicular).
Can Subtalar Arthritis Be Treated Without Ankle Fusion?
The short answer is usually “yes.” The key is often tightening lax ankle ligaments with an injection of stem cells or platelets. Why? Loose ankle ligaments allow too much motion in the subtalar joint which can chew up the cartilage in the joint. This is why they want to fuse the joint.
This problem of loose ankle ligaments is very common. It usually begins when you turn your ankle or sustain some other injury, usually when you’re younger. That ligament sprain heals and then things feel fine for years. However, during that time, the ankle joints (tibiotalar or subtalar) are taking significant small hits.
Eventually, that accumulated wear and tear catches up with the patient as they age and one day the joint begins to hurt. To learn more, see my video below:
The ankle ligaments that support the subtalar joint include:
- The deltoid ligament
- The sinus tarsi ligaments
The Deltoid
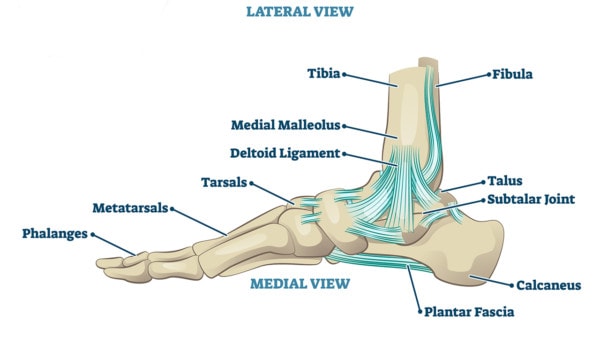
Ankle joint vector illustration. Labeled educational leg structure scheme. Physiological orthopedics explanation with isolated toe closeup. Cross section with phalanges, tibia, tarsals, ligament graph
The deltoid ligament is the duct tape on the inside of the ankle. As you can see from the picture above, it’s a complex of ligaments (see above). The inside of the sub-talar joint lives right under these ligaments.
Sinus Tari Ligaments

These are ligaments that live in a hole on the outside of the foot called the sinus tarsi. The picture above is a cross-section through the foot just in front of the heel. The subtalar joint is shown to the right. These ligaments also stabilize the subtalar joint.
Can You Treat the Subtalar Joint With Orthobiologics?
We have treated subtalar joint arthritis for years with injections of high dose platelets or bone marrow stem cells. To get that to work, you need to target the ligaments above using both precise ultrasound and x-ray guidance (fluoroscopy). The goal here is to prompt healing and tightening of those ligaments to stabilize the joint.
Then the joint and the bone are also targeted through precise injections to treat the toxic witches’ brew of chemicals in the arthritic joint and the surrounding swollen and often damaged bone. The bone must be injected through x-ray guidance.
How Many Patients Can Avoid a Subtalar Fusion?
We find that about 2 in 3 patients who are told they need a subtalar fusion can usually avoid it. Take for example Tracy, a Nepal trekking adventurer. She had severe bilateral subtalar arthritis and was told she needed a fusion.
She had stem cells injected into the ligaments, joints, and bones and then needed several additional ligament injections to further stabilize the joint. Her tendons surrounding the ankle were also generally torn up, so these were treated at the same time. She went from walking only a few hundred steps a day to walking miles at a clip and basic hiking.
The upshot? The subtalar joint is one of the more complex and forgotten joints of the ankle. Subtalar fusion is needed in a few patients, but most who are told they need this invasive surgery can likely avoid it with less invasive care.
———————————————–
References
(1) Yasui Y, Hannon CP, Seow D, Kennedy JG. Ankle arthrodesis: A systematic approach and review of the literature. World J Orthop. 2016;7(11):700–708. Published 2016 Nov 18. doi:10.5312/wjo.v7.i11.700
(2) Park JS, Shim KD, Song YS, Park YS. Risk factor analysis of adjacent segment disease requiring surgery after short lumbar fusion: the influence of rheumatoid arthritis. Spine J. 2018;18(9):1578-1583. doi:10.1016/j.spinee.2018.02.005
(3) Morrey BF, Wiedeman GP Jr. Complications and long-term results of ankle arthrodeses following trauma. J Bone Joint Surg Am. 1980;62(5):777-784. https://pubmed.ncbi.nlm.nih.gov/7391101/
(4) Maffulli N1, Longo UG, Locher J, Romeo G, Salvatore G, Denaro V. Outcome of ankle arthrodesis and ankle prosthesis: a review of the current status. Br Med Bull. 2017 Dec 1;124(1):91-112. doi:10.1093/bmb/ldx042

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
