TMJ Stem Cell Therapy: Valerie’s Story
Every doctor sees patients who, right off the bat, he or she knows are a huge challenge. Valerie was one of those patients with one of the most severe cases of TMJ I have ever seen. She was unable to eat solid or soft foods at any level, and I was pretty sure she also had severe neck injuries that had gone undiagnosed. Ultimately she got her life back through highly precise TMJ stem cell therapy as well as a novel first of it’s kind therapy in her neck.

What Is the TMJ, and What Can Go Wrong?
The temporomandibular joint (TMJ) is the hinge joint at the jaw that you use to eat and chew. In mild TMJ syndrome, patients notice intermittent pain in the joint in front of the ear or in the muscles around the joint when talking or chewing. The joint has four key components with two that are often missed even by expert TMJ physicians, surgeons, and dentists.
First, like any joint, the TMJ has cartilage inside that serves as a protective cushion where the bones that make up the joint meet. In addition, like the knee, there is a natural spacer in the joint known as the “disc” (articular disc of the TMJ joint). This is a meniscus-like structure that moves in predictable ways as you open and close you jaw and that provides further protection for the joint due to the immense loads that can be generated with chewing. Like any other joint in the body, the cartilage or spacer can be injured or become damaged due to wear and tear leading to painful arthritis.
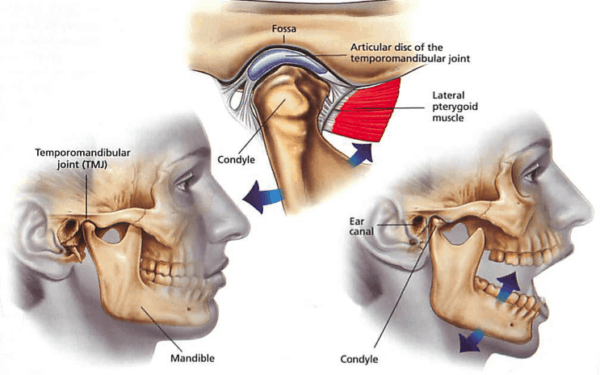
The next key component of the joint is the muscles that help to move it. There are many different ones including the masseter, the large temporalis that comes from the side of the head, the pterygoids, and strap muscles. The muscles work together in a symphony of millisecond-timed precision to open and close the jaw. These are powerful muscles that can develop trigger points like any other muscle—areas that are shut down and painful. These muscles also have tendons that attach to bone, so these areas can develop tendinopathy—or small tears and degeneration which can cause them to become painful.
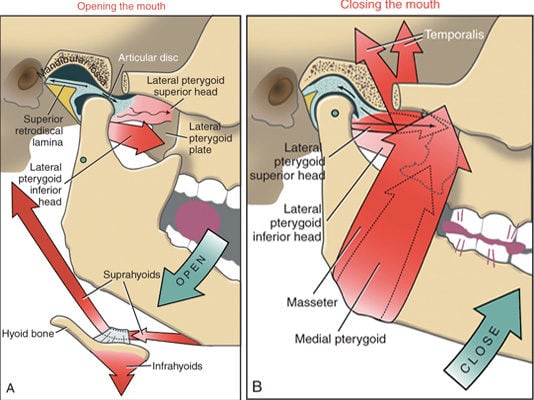
The final two key components are often overlooked by TMJ experts, and they’re key to why we were able to help Valerie with precise TMJ stem cell therapy. These are the ligaments that stabilize the joint and how the TMJ fits into its regional ecosystem in the body—the head and neck.
Ligaments stabilize joint by acting like pieces of duct tape that guide it and prevent motions for which it wasn’t designed. The TMJ has many ligaments that often get ignored by medical providers. These are the sphenomandibular, stylomandibular, and capsular ligaments. In addition, the tough covering of the joint (capsule) is further divided into collateral (lateral) ligaments, similar to the knee.
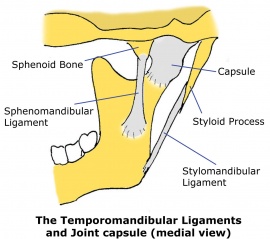
Finally, most TMJ providers focus on the bright shiny object of the TMJ itself, forgetting that it’s a joint that lives in the ecosystem of the head and neck and that it can’t work efficiently without it’s neighboring structures working well. So neck problems will place more pressure on the TMJ joint. In addition, if the neck is unstable because its ligaments have been injured or the small muscles that stabilize it are off-line, then the body attempts to use the TMJ muscles as accessory stabilizers of the neck. Given that the joint and its muscles aren’t designed to handle these extra loads, it eventually breaks down, and the muscles get overwhelmed. To learn more about how ligaments and muscles stabilize the neck and back, read our book Orthopedics 2.0.
Valerie’s Nightmare and Eventual TMJ Stem Cell Therapy
When I first evaluated Valerie, in December of 2014, she had a history of issues with her TMJ since age 18, and she was 60 at the time. It all began with having her wisdom teeth removed as a teenager, and then five years ago, her teeth got stuck on something and she felt intense and then progressive TMJ pain. In her past she had also suffered from whiplash and head injuries. More recent was a fall that fractured a low-back vertebra and injured her SI joint. In addition, a yawn earlier that year had dislocated the TMJ, further exacerbating her issues. She was on a liquid-only diet, forced to blend her meals and drink them. She had tried every TMJ treatment under the sun without much relief.
When I first met Valerie and looked at everything from her low back to her neck to her jaw, I have to admit, I was a bit overwhelmed. So I cautioned her that while I could treat the whole picture using ultra precise TMJ stem cell therapy injections under ultrasound and fluoroscopic guidance as well as platelet procedures in many areas, given that she couldn’t even chew soft foods, I didn’t know how far we would get. Over the ensuring year and a half, we treated the TMJ joint and discs; all of the TMJ ligaments above, including some on the inside of the joint; damaged facet joints in the neck; neck ligaments; her SI joint; bulging and painful spinal discs; and then finally her alar/transverse ligaments. The final treatment was really what I feel helped her recover the most, and this procedure to treat the ligaments that hold her head on (alar/transverse) was developed by me only a few months before she tried it.
The head is held on by strong ligaments. These connect the upper two neck bones to the head and are called alar and transverse ligaments. We know from a few studies that they can be stretched in whiplash injuries or when there’s a blow to the head. These patients often have headaches, a heavy- or tilted-head feeling or appearance, problems thinking and concentrating, and other symptoms. The surgery to fix this issue is an upper cervical fusion which is a huge and high-risk affair, with many patients avoiding the procedure due to fear of major complications./symptom/why-your-head-feels-heavy-weak-upper-neck-muscles-may-also-be-causing-your-headaches/
In Valerie’s case, while she was making progress with each successive procedure, I felt that laxity in these important head-stabilizing ligaments was causing her body to use the TMJ and its powerful muscles as secondary stabilizers, causing the joint to break down. In other words, we would never be able to fully get her better without also treating these upper neck ligaments. I ordered a moving stress X-ray of the cervical spine called a DMX, which did confirm that the alar/transverse ligament complex was lax and not protecting her upper neck.
Injecting into these ligaments with stem cells to help them heal and strengthen has been impossible until recently. They can’t be accessed from traditional ligament injections that come from the back of the neck as the spinal cord is in the way. I had been thinking for years that there had to be a way as we had many patients who had sought us out for our rare expertise in injecting upper neck joints (C0–C2) and posterior ligaments with fluoroscopy. Then one day, while staring at a model of the upper cervical vertebra and its ligaments that we have in the office, it hit me. There was a small hiatus (medical speak for hole) in the front of the spine between C1 and C2 that could allow a needle to be passed using fluoroscopic guidance through the front and into these ligaments. After about a year of planning and consulting with colleagues, in September of last year, Valerie was one of the first patients in the world to have her own stem cells injected into her damaged alar/transverse ligaments (or anything else for that matter given no physician had ever injected these structures).
So how did Valerie do? I recently pinged her via e-mail because I am giving a talk on this novel, ultraprecise injection of the alar/transverse ligaments in Florida next week. This is what she wrote back:
Hi!
Wow! Given Val was one of those patients who I really had my doubts I could help, what a great way to wake up on a Saturday morning! We all take for granted the little things that when they’re lost can be devastating—the ability to walk, talk, run, or chew.
Watch Valerie’s video testimonial.
The upshot? There’s more to TMJ stem cell therapy than injecting magic stem cells into the TMJ joint or starting an IV. Not only does it often take precise injections into the joint, but also into obscure ligaments and oftentimes the neck. For Valerie, it also took a new procedure that was developed based on the need to have a treatment for ligaments that had never before been injected!
————————————–
After I posted Val’s story, she sent this e-mail to elaborate on the results from all of the different body areas we treated:
“You might want to add that I have been completely rebuilt by your Regenexx treatments. I am straighter, sturdier and have much improved mechanics than I ever thought would be possible, even before I broke my back and dislocated my jaw. I barely even have a click in my jaw that I have had since age 16. And, I am taller :)

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.

