Should You Get Knee Arthritis Nerve Treatment?
The newest craze in knee pain treatment is a knee arthritis nerve treatment. This procedure has gone from 0 to 60 in the last few years, but is it a good idea? Does it work? How long does it last? Are there better options?
How the Knee Arthritis Nerve Treatment Works
This new knee arthritis nerve treatment works through radiofrequency (RF) energy. The doctor places a “cool” radiofrequency probe near the nerves that carry pain signals in an arthritic knee joint and then zaps these nerves with this type of electromagnetic energy. The treatment dulls the ability of the nerves to carry pain signals and provides relief for a time.
Does This Treatment Treat Arthritis?
Nope. In fact, it’s more likely than not that it may make arthritis worse over time as the normal instinct to protect the painful arthritic joint isn’t there anymore while the nerves are dulled. See below for the discussion on “Charcot” joints.
How Well Does the Treatment Work?
In one recent study, the procedure was able to reduce knee pain by 50% for only 35% of the knee arthritis patients who had the treatment. Another small randomized controlled trial showed 3–6 months of relief, but interestingly, the radiofrequency procedure wasn’t any better than a steroid and anesthetic injection. A different research investigation found that the injection of steroid anti-inflammatory and anesthetic into these nerves was no better than just local anesthetic at reducing pain.
The company that makes these expensive RF devices sponsored a recent study. This one showed that the procedure was better than steroid/anesthetic, but again, the results are not measured longer than 6 months. There was no randomization of these patients and no blinding, so they knew they were getting the more invasive therapy, potentially biasing results.
Finally, a study was just published out of Egypt that included 60 patients who were randomized to either the RF procedure or Tylenol and NSAIDs (acetaminophen). The study only showed differences between the two groups in the primary outcome measure (WOMAC functional scale) at 6 months. So in summary, none of these studies show that the procedure works all that well. None of them were high-level, double-blind studies where the patient didn’t know whether they got the real or a sham procedure. This kind of blew me away, because this is a very invasive procedure that destroys tissue!
Does This Therapy Kill or Hurt the Nerves?
“Cool” RF sounds like a more gentle version of radiofrequency. Why? Traditional RF works by heating the tissue and thus destroying it with thermal energy. In the case of a nerve, that means damaging the nerve. However, “cool” means lower temperatures. However, based on recent research, it’s the opposite.
Believe it or not, the standard way to check out the lesion size of an RF technique is to stick the probe in an uncooked chicken breast! A recent study checked the lesion size of cool RF in a chicken breast versus the higher temperature version. The result? Cool RF produced an even bigger lesion!
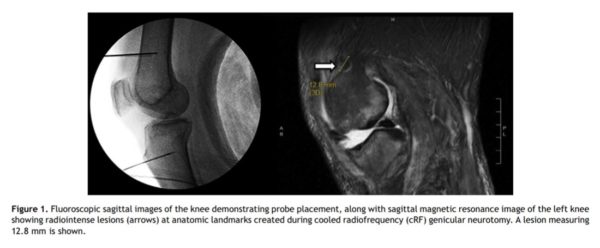
For example, a recent MRI case report showed that the lesions created by the procedure could be seen on MRI (see image below which also shows bone damage). This is not really a good thing as it would indicate that tissue damage beyond the nerve occurred.
©Regenexx
The white arrow above is pointing to a cool RF lesion that not only ablated the nerve but also damaged the bone.
What Happens When a Joint Can’t Feel?
When a joint can’t feel, in medicine, we call it a Charcot joint. These are commonly seen in diabetics whose nerves die off. What happens? The joints become horribly damaged and disfigured. Why? The patient loses the normal protective instinct because they feel no arthritic pain, so they just keep going and damaging the joint.
Is There a Better Way?
Obviously, if you had a choice between killing otherwise important nerves to help pain versus injecting something to spark repair, the latter would be the way to go. Platelet rich plasma (PRP) has growth factors that can help tissue repair and is a good cool RF alternative with solid research support to show that it helps mild to moderate arthritis. See my video below on the different types and quality of PRP:
If the arthritis is more severe, our research is showing that a precise same-day bone marrow stem cell procedure may help the pain for years at a time. See below for how that procedure is performed using best practices:
The upshot? Diving into the research on knee arthritis nerve treatment is a bit scary. If it were my knee, I would try to avoid getting my nerves nuked with “cool RF” and instead focus on on using my own platelets or stem cells to help knee arthritis pain.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
