Spontaneous Osteonecrosis Of The Knee (SPONK)

Medically Reviewed By:
Spontaneous osteonecrosis of the knee (SPONK) is a condition that primarily affects older adults, associated with sudden-onset knee pain and potential joint degeneration. This condition develops without a known cause and can progress rapidly, significantly impacting knee function and quality of life.
SPONK often presents with acute pain in one knee, restricting mobility and making daily activities challenging. If left untreated, SPONK can lead to further joint damage, highlighting the importance of early intervention.
What is SPONK?
SPONK is a condition in which bone tissue in the knee begins to deteriorate due to a sudden loss of blood supply. This weakening of the bone’s structure can make the knee painful and more vulnerable to damage.
Over time, as the affected bone loses integrity, nearby cartilage may also deteriorate, potentially leading to joint instability and arthritis. SPONK typically affects one knee and can progress quickly, making early detection and intervention important for preserving joint health.
Causes Of Spontaneous Osteonecrosis Of The Knee
SPONK arises from two main factors: chemical damage to bone cells and excessive force on specific knee areas. The body continually undergoes wear and tear, usually repaired during rest.
Stem cells play a crucial role in this repair process, residing in various tissues and restoring minor injuries. However, the body’s natural repair mechanisms become less efficient as it ages. When the bone’s stem cells weaken or when wear surpasses the repair capacity, bone cells may begin to deteriorate, leading to SPONK.
SPONK generally affects individuals over 60 and is more commonly seen in women, with the inner thigh bone (medial femoral condyle) involved in 94% of cases. Critical contributors to SPONK include:
- Subchondral insufficiency fracture: SPONK often results from a minor fracture in the bone just below the cartilage, known as the subchondral area. As damage accumulates faster than the bone can heal, particularly with age-related declines in repair capacity, bone cells may die, initiating SPONK.
- Reduced blood flow: A diminished blood supply to the knee joint contributes to bone cell damage. Factors such as steroid use and excessive alcohol consumption have been linked to SPONK because they can impair blood flow, reducing the oxygen and nutrients essential for bone health.
- Meniscal injuries and surgery: Knee surgeries, especially removing part of a torn meniscus (meniscectomy), can increase the risk of SPONK. The meniscus functions as a spacer, distributing pressure within the knee joint.
When removed, the loss of this cushioning effect can overload the knee bones, raising the risk of SPONK. Research indicates that meniscectomy can contribute to arthritis, consistent with findings that removing parts of the meniscus may also contribute to SPONK.
By recognizing these contributing factors, especially in older adults, SPONK can be identified and managed early, potentially preserving knee function and reducing pain.
Common Symptoms Of SPONK
SPONK typically affects one knee, causing intense discomfort that limits movement and makes weight-bearing activities challenging. Recognizing symptoms early can support timely treatment to manage pain and protect knee function. Key symptoms include:
- Sudden Onset of Severe Knee Pain: SPONK often begins with sudden, sharp pain in the knee, particularly during movement or weight-bearing activities.
- Tenderness: The affected area may be tender to the touch, with increased sensitivity around the joint.
- Swelling: Swelling around the knee joint is common and may be accompanied by warmth or redness.
- Decreased Range of Motion: Pain and swelling can cause a reduced range of motion, making it challenging to extend or bend the knee fully.
These symptoms can vary in intensity but often worsen without treatment, impacting the knee’s stability and function over time.
Diagnosing Spontaneous Osteonecrosis Of The Knee
Diagnosing SPONK requires clinical evaluation and imaging tests to accurately assess the condition and determine the extent of bone damage. Early diagnosis is essential for guiding treatment and preventing further joint degeneration.
Physicians typically begin with a thorough clinical evaluation and specific imaging tests to confirm the diagnosis and identify the affected areas. Key steps in the diagnostic process include:
- Clinical Evaluation: The physician will assess symptoms, review medical history, and inquire about recent injuries. A physical exam helps identify tenderness, swelling, and limitations in knee movement.
- Imaging Tests: Imaging is critical in diagnosing SPONK and assessing bone health. X-rays, MRIs, and bone scans provide detailed images of the knee, confirming the presence and progression of SPONK.
- X-rays: Often conducted as the initial imaging test, X-rays can reveal bone changes and joint space abnormalities related to SPONK.
- MRI: MRI scans offer detailed images of soft tissues and bone marrow, allowing for early detection of SPONK before significant bone collapse occurs.
- Bone Scan: A bone scan detects increased activity in the knee, highlighting areas affected by SPONK and assessing the extent of bone involvement.
Together, these diagnostic tools provide a comprehensive view of the knee’s condition, allowing for a more tailored approach to treatment and management.
How Is Osteonecrosis Of The Knee Treated?
SPONK is often treated with surgery, especially in the advanced stages. However, non-surgical treatments may be better alternatives when SPONK is caught early and hasn’t yet affected the joint cartilage.
These conservative options focus on reducing weight-bearing on the knee, managing pain, and occasionally using osteoporosis medications, such as bisphosphonates, to support bone health. Standard treatment options include:
- Rest and Activity Modification: Limiting activities that strain the knee can reduce stress on the affected area, allowing the bone to heal and decreasing pain.
- Bracing: A knee brace can help stabilize the joint and relieve pressure on the damaged area, promoting better alignment and support.
- Non-Steroidal and Inflammatory Drugs (NSAIDs): Nonsteroidal anti-inflammatory drugs (NSAIDs) help reduce pain and inflammation in conditions affecting joints, muscles, and the spine. While they provide temporary relief, prolonged use may increase heart, kidney, and gastrointestinal risks, requiring careful management. Read More About NSAIDs.
- Physical Therapy: Customized exercises can strengthen the muscles around the knee, improving stability and range of motion while reducing pain.
- Core Decompression: In some cases, a minimally invasive procedure called core decompression can relieve pressure within the bone, potentially enhancing blood flow and promoting healing.
- Knee Arthroscopy: Arthroscopy may be recommended to clean out damaged tissue in the joint, providing pain relief and potentially delaying further degeneration.
- Joint Replacement: For severe or advanced SPONK, a joint replacement might be necessary to restore knee function and relieve chronic pain.
These treatment options provide a spectrum of approaches, from conservative care to surgical solutions, helping patients manage SPONK and improve their quality of life.
Can SPONK Be Treated Without Surgery?
SPONK is a serious knee condition that frequently requires surgery. However, newer techniques have reduced the need for more invasive procedures like knee replacement. An evolving approach to treating osteonecrosis involves using the patient’s own bone marrow concentrate containing mesenchymal stem cells to address the disease.
Bone marrow concentrate (BMC) therapy is a regenerative treatment that uses stem cells from the patient’s own bone marrow to promote healing and reduce inflammation. A small sample, typically taken from the hip, is processed to concentrate stem cells, growth factors, and other regenerative components.
These are then injected into the affected knee to support tissue repair, improve function, and potentially slow joint degeneration. This technique is available in the U.S. as BMC therapy and as culture-expanded cells in select locations outside the U.S. within the licensed Regenexx network, offering a less invasive alternative to surgery.
Percutaneous Intraosseous Injection (PII)
Percutaneous intraosseous injection (PII) is a minimally invasive procedure that delivers BMC directly into the SPONK lesion using live X-ray guidance (fluoroscopy). This precise injection method helps target damaged bone, supporting natural healing and potentially improving knee stability.
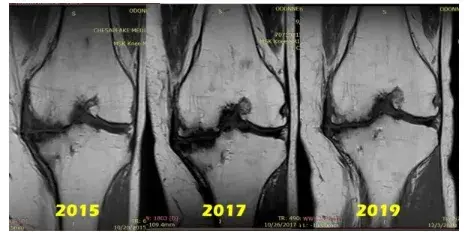
The image above shows a series of MRI scans tracking changes in the bone of a patient with SPONK who received multiple PII treatments. In these images, darker areas indicate damaged bone, while brighter areas suggest healthier bone.
Over time, differences in the bone’s appearance have been observed, showing changes after the procedure. While more research is needed to understand the long-term effects, these images help explore how PII may play a role in orthopedic and regenerative medicine.
Platelet-Rich Plasma (PRP) Therapy
PRP therapy, or platelet-rich plasma therapy, utilizes the body’s natural healing abilities by concentrating and reinjecting growth factors from the patient’s own blood. In this process, a small blood sample is drawn and processed to isolate platelets rich in growth factors crucial for tissue repair.
Once injected into the affected knee, these concentrated growth factors help stimulate the repair of damaged tissues, encourage cell regeneration, and reduce inflammation, ultimately easing pain.
PRP therapy aims to enhance the body’s healing process, accelerating tissue repair in areas with limited blood flow, such as the knee. For individuals with SPONK, PRP may aid in healing the affected bone and surrounding tissues, offering a supportive, non-surgical alternative that may delay or reduce the need for more invasive treatments.
Find The Right Option To Address SPONK
Many cases of SPONK may be managed with non-surgical interventions, particularly when diagnosed in the early stages. Interventional orthobiologic procedures may help support the body’s natural healing process and reduce pain without requiring invasive surgery.
If you have been diagnosed with SPONK or are experiencing knee pain, consider exploring all available options. Consulting with a physician in the licensed Regenexx network can provide valuable insights into whether this approach may be appropriate for your condition.
Schedule a consultation with a physician in the licensed Regenexx network to explore non-surgical treatments for SPONK.

Medically Reviewed By:
