4 year Follow-up on a Patient with Severe Knee Arthritis Treated with Stem Cells
We’ve been treating knee arthritis with stem cells for a long time with different knee arthritis stem cell injections. When other clinics that have popped up in the last year or two didn’t know what the word stem cell meant, we were diligently treating patients with our Regenexx-C and Regenexx-SD stem cell procedures in a clinical trial. While we’ve published many studies since then, our first was published in 2006 on a fore runner of today’s -SD stem cell procedure. We haven’t been shy about honestly reporting our results versus hyping them based on the fact that we were using stem cells. Today’s case is an example of that transparency.
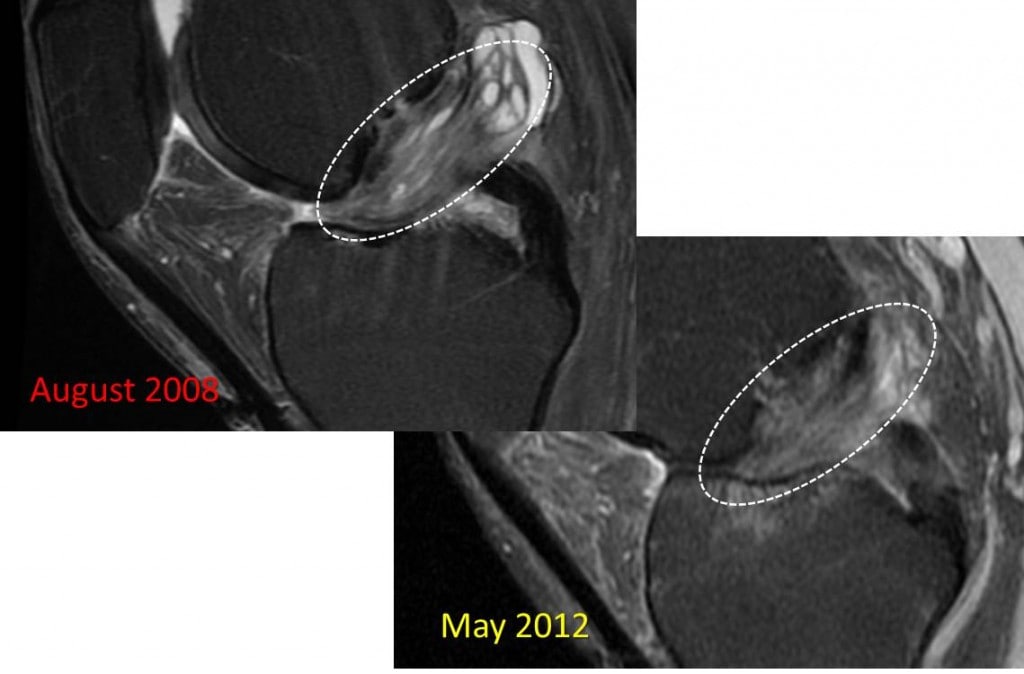
This is a then 57 year old woman from Arizona (JM) who received a knee arthritis stem cell Regenexx-C treatment in 2008 in the medial compartment-which had suffered from years of severe degeneration since the 1970’s, when she had her entire knee meniscus removed. When we first performed her Regenexx-C stem cell procedure in September of 2008, she went from non-functional, with difficulty walking to very little pain and dramatically more functional. A few months ago, she was pulling on a cowboy boot, she felt a pop in the lateral compartment (opposite the area we treated) and has had pain ever since. We’re now evaluating her for an update treatment. The medial compartment is holding up nicely and my best educated guess is that her pain is now being caused by a new lateral meniscus tear. Since she had an end stage arthritis knee when she was first seen in 2008, it’s not surprising that her lateral meniscus (which was under compression at the time due to being pinched by bone spurs), eventually tore. Did we grow her a new knee, despite her severe arthritis? NO. There’s no evidence that this happened. Despite the fact that she still has no pain in her medial compartment some 4 years after a single injection of her own stem cells, the biggest change is in the ACL ligament. While the 2008 and 2012 MRI’s are on different scanners with different parameters, the ACL changes are hard to ignore. Above you see the ACL in the dashed circle from the 2008 MRI and on the right a matching slice from the 2012 MRI. Note that the ACL has gone from a cystic and mucoid mess (bright rounded areas in the middle of barely visible ACL fibers) to consolidated and well formed in the 2012 MRI. Is her ACL perfect 4 years after stem cells? No. However, it’s much better than it was.
The upshot? You could view this result either as continued and holding improvement in the medial compartment or 3.5 years of relief after a single injection in an end-stage knee that has now shifted back toward degeneration. Again, our long-term focus is on continuously improving these procedures for our patients and the only way to do that is honest and accurate assessment of how well and how long all of this works. In addition, all of this takes years of evolution and tracking patients.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.