Ask Dr. C – Episode 5

This is another blog where I answer selected patient questions in a long format. So here goes:
Interested in seeing mri evidence that stem cells injected into knee heals meniscus tears and how long it takes.
There are two issues here. The first is what I called the meniscus fetish. The second is the MRI evidence we’ve collected over the years.
The research shows that degenerative meniscus tears are about as important as wrinkles. In fact, there’s a medical journal article with that title:

What is a degenerative meniscus tear? That’s a meniscus tear that occurs in someone over 35. Why did this author take that position? Because the research shows that meniscus tears are common in patients over that age who have no knee pain and likely will never have any future knee pain. Meaning that meniscus tears are part of the normal aging process. Hence in most middle-aged or older patients who have a meniscus tear seen on MRI after some injury or random start of pain, the cause of their pain is NOT the meniscus tear. We also have multiple high-level research studies that show that operating on these tears is no better than no surgery. In summary, being worried about a meniscus tear if you’re over age 35 is like being worried about the mounting wrinkles as you age. Learn to love aging and not fear it.
On the other side of this coin is evidence of stem cell based meniscus healing. Here are some images:
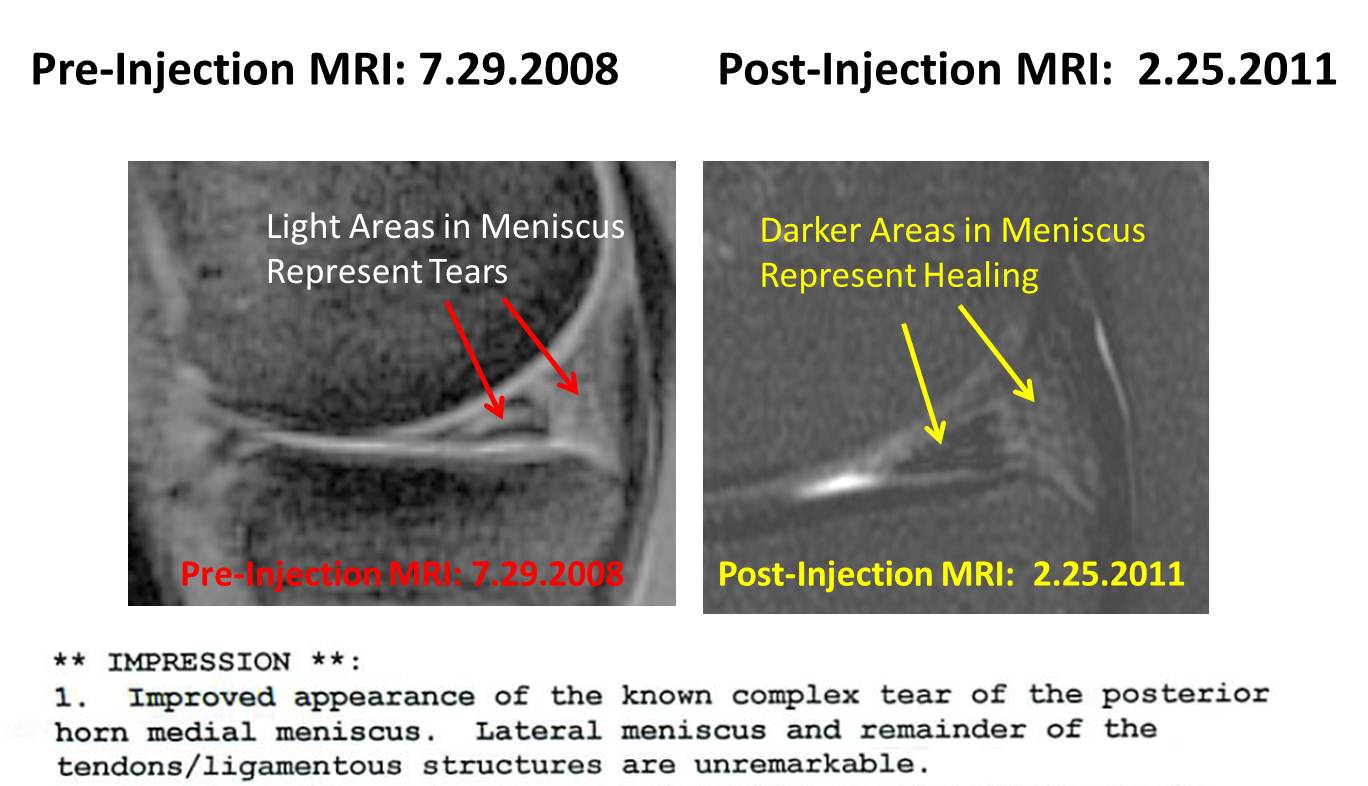
We have other images that we’ve collected, like those in this published paper:
What are objective results for improvements from using orthobiologics to improve stability besides what the patient reports for pain? Would the physican that did the injection be able to have a subjective or objective opinion for improved stability later on?
Instability in a joint means that the ligaments that are supposed to hold the joint together and align the surfaces are loose or damaged. We commonly treat these ligaments by injecting PRP or bone marrow-derived stem cells (bone marrow concentrate) into those ligaments via precise imaging guidance. We do that in lots of places like in knees with blown-out ACLs and the ligaments that support the spine or hold on the head.
Our first data showing that this was possible was in the neck and we published those results:
We have measured reductions in instability in other ways as well:
We also routinely measure instability before and after ACL stem cell procedures. That’s on physical exam and now part of a randomized controlled trial that’s ongoing. Here are those MRI results:
We also routinely treat ankle ligaments and look at before and after stress ultrasound showing the return of stability. Hence, we are very comfortable with the idea that we can enhance ligament based stability in patients who are good candidates.
The upshot? I hope these answers help. I have more to answer and should get to some of those tomorrow.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.


