Craniocervical Instability Measurements
Did you know that some people have problems with the ligaments that hold their head on? These patients often become like a pinball in the great arcade game of medical specialists, going from one to the other without a diagnosis. They can sometimes find a diagnosis if they meet a doctor who knows which tests to order or which measurements to take. So today we’ll explore all of this a bit.
My Experience with this Diagnosis
When I was a young doctor, I was asked to treat many patients who had been injured in car crashes. Through that experience, I noticed there was a subpopulation of patients with headaches and dizziness or imbalance. Eventually, I met a friendly audiologist who could use a test called ENG to identify them. I also eventually learned that I could successfully treat some by focusing on their upper neck. Finally, we adopted methods to measure their instability and then a novel technique to treat the problem.
What is Upper Neck Instability?
Upper neck instability goes by a few different names including craniocervical instability (CCI) and craniocervical junction (CCJ) instability. Instability just means that the ligaments that hold something together and stable are damaged and loose. This causes the joints in this area to move abnormally and this can increase the wear and tear on that joint. In this case, these are the ligaments that hold the head onto the spine.
Upper Neck Ligaments
There are a number of upper neck ligaments including the alar, transverse, accessory, and other ligaments (1). These are shown below:
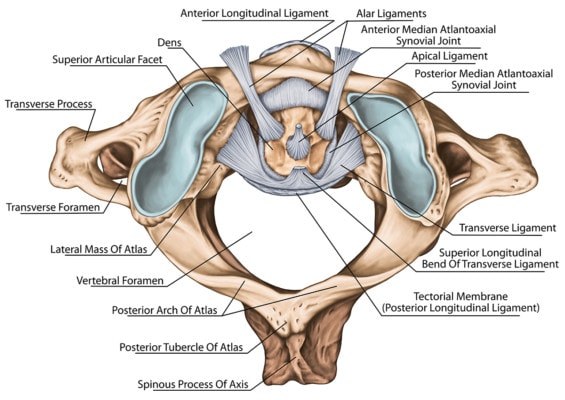
Stihii/Shutterstock
Basically, these ligaments connect the first two neck bones (C1 and C2) to the skull or to each other.
CCJ Instability Cause and Symptoms
The ligaments that hold the head on can be injured with trauma or can become loose with wear and tear. Many patients with this problem have had trauma like a car crash and/or hit on the head. However, sometimes patients also have abnormal ligaments and less trauma. This is usually called Ehler-Danlos Syndrome or EDS (2). These patients are at more risk for many joint problems, but their upper neck instability is often disabling.
These patients often have a collection of common symptoms like:
- Headaches
- Neck and other pains
- Dizziness or imbalance
- Cognitive problems
- Rapid heart rate
To learn more about this condition, watch this video:
CCJ Instability Tests
There are a number of different imaging options for craniocervical instability like real-time video x-rays, CT Scans, and MRI. All of these have different positives and negatives. Let’s dig in below.
X-rays
As far as x-rays are concerned, a moving x-ray that can monitor the bones and their relationships is called a DMX or Digital Motion X-ray. This is not a standard x-ray, but uses specialized equipment:
Pros: The test can show side to side instability and what happens with real-world dynamic motion
Cons: Often not covered by insurance, less published data on norms
CT Scan
A specialized Rotatory CT Scan can also help diagnose craniocervical instability (3). This is NOT a routine CT Scan, but one where the patient’s head is turned to the right or left and the movement between C1 and C2 are measured.
Pros: Some published norms
Cons: Higher x-ray exposures, not dynamic
MRIs
There are two different types of MRIs that can diagnose upper neck instability. This includes a static high-field MRI and a lower field strength movement MRI. The former is a 3T MRI which is performed using a very specialized protocol, In particular, a routine MRI does not image this area. To learn more about that type of MRI, see below:
Pros: Some published norms, static measurements can be applied
Cons: Can see the morphology of the ligaments, not dynamic
There is also a movement-based MRI that is also called a “Stand-up MRI”. This is a specialized machine that allows the patient to sit or stand-up and allows for motion. So for example, you can bend your neck forward, backward, or sideways:
Pros: Some published norms, static measurements can be applied
Cons: Higher x-ray exposures, some movement is allowed, but not “live” movement
Measurements
There are measurements that can be performed on x-rays or preferably MRIs. The two most common are the Grabb-Oakes and the Powers Ratio. Both look at the position of the skull versus upper neck bones. Here’s how these two are measured:
Grabb-Oakes
Powers Ratio
Getting a Diagnosis
Obviously, you need the right imaging and measurements. However, you also need a physician who has diagnosed and treated many patients with upper cervical instability. The problem is that most of these physicians are spine surgeons who generally only have one option, which is the fusion of the upper neck bones, which is an invasive and risky surgery. Physicians who understand this diagnosis and who can offer injection-based treatments are very rare. in fact, even on our highly trained network, we generally only offer diagnosis and treatment at a few sites, with our Colorado HQ site having the most expertise.
Non-Surgical Treatment?
As I discussed above, getting a diagnosis is hard. However, navigating treatment options can be a nightmare. For example, physical therapy can often be difficult in this group of patients, often causing flare-ups. Upper cervical chiropractic like NUCCA and chiropractic curve restoration techniques can help, but the worst patients only respond temporarily to these therapies.
Upper neck prolotherapy can help somewhat as well as upper cervical facet injections. However, neither of these address the deep ligaments we discussed above. To get those injected, only one procedure exists called the PICL (Posterior Implantation of Cranialcervical Ligaments) procedure:
Please note that the PICL procedure is COLORADO ONLY.
The Upshot? Getting a diagnosis can be difficult, but many patients who have had these strange symptoms and tried many therapies and who have not responded are relieved to finally know what’s wrong. Hopefully, this guide helps you understand better how a CCJ instability diagnosis is made and what options exist for help.
_________________________________________________
References:
(1) Offiah CE, Day E. The craniocervical junction: embryology, anatomy, biomechanics and imaging in blunt trauma. Insights Imaging. 2017;8(1):29–47. doi:10.1007/s13244-016-0530-5
(2) , , , , , , ,, , , , , . 2017. Neurological and spinal manifestations of the Ehlers–Danlos syndromes. Am J Med Genet Part C Semin Med Genet 175C: 195– 211.
(3) Patijn, J., Wilmink, J., ter Linden, F. et al. CT study of craniovertebral rotation in whiplash injury. Eur Spine J (2001) 10: 38. https://doi.org/10.1007/s005860000212

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
