Flexor Hallucis Longus Tendon Pain: Is Surgery the Answer?
This is a story about Scott, a frustrated runner. One day in 2010 while out for a run, he suddenly heard a snap under his foot. He went from a normal, active life to trying years of different therapies without help. This is his story about how flexor hallucis longus tendon pain almost ruined his life.
What Is the Flexor Hallucis Longus Tendon?
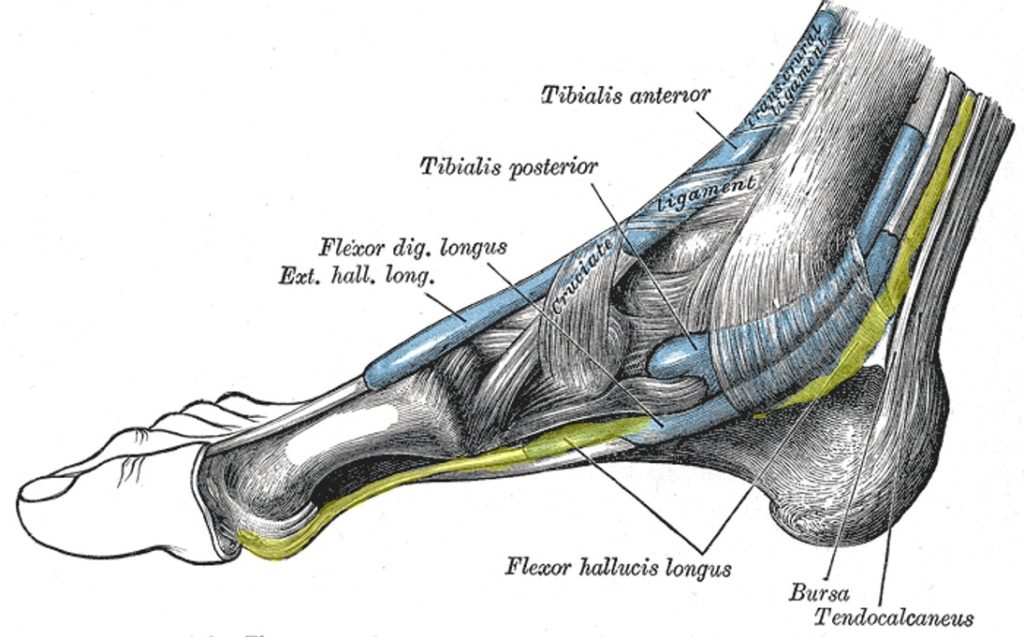
The flexor hallucis longus (FHL) tendon lives on the bottom of the big toe. I’ve highlighted the tendon in yellow in the picture to the right (click on the image to make it larger). The FHL flexes the toe and along with other tendons also helps to stabilize the ankle. It’s pretty unique in that it has many functions.
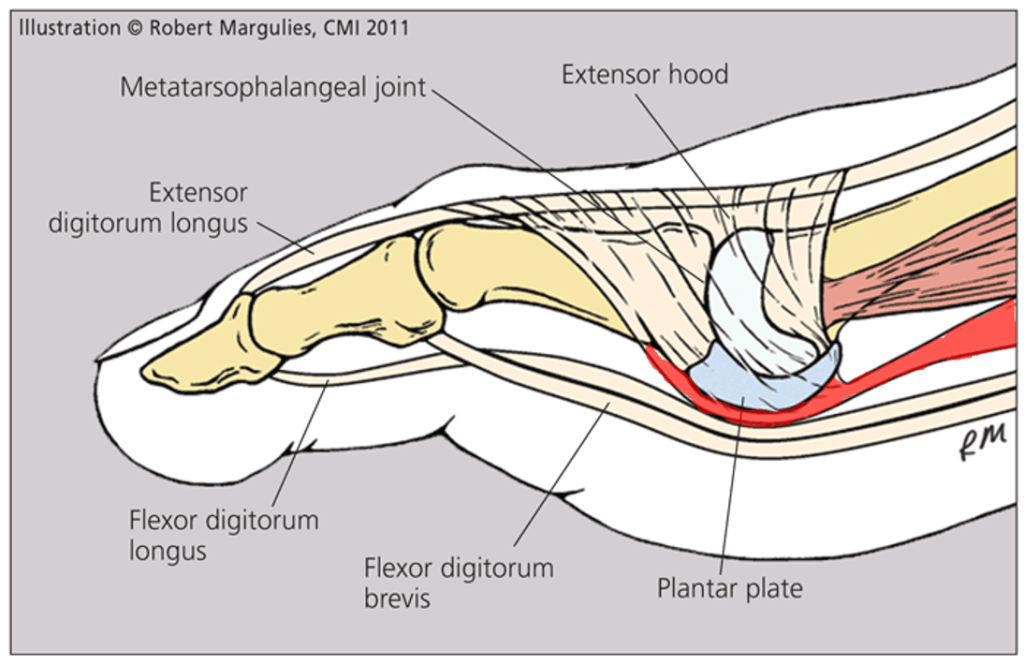
To understand all of Scott’s injuries, you have to understand how the FHL relates to the plantar plate (PP). The PP is a fibrocartilage plate that lives on the bottom of the big toe and other MTP joints. It helps protect the joint from impact forces, like running, similar to the meniscus in the knee. The picture shows how the FHL tendon attaches to the plantar plate just as other foot flexor tendons attach to other plantar plates in other MTP joints.
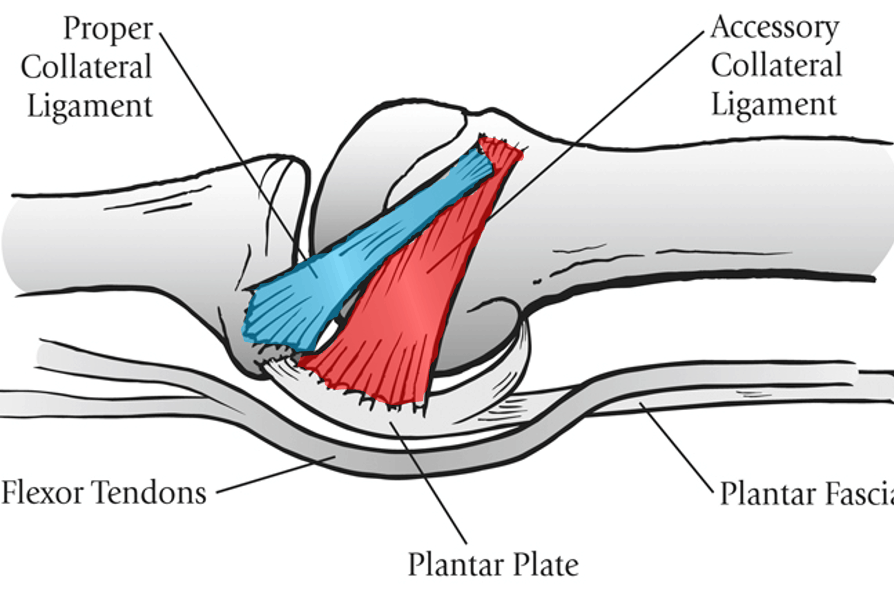
Finally, there are ligaments at play here as well. The image to the right shows that there are two ligaments at the side of the toe MTP joints, one that heads downward in red (accessory collateral ligament, or ACL of the toe) and the other in blue (proper collateral ligament, or PCL). For our purposes the ACL is important as it helps to stabilize that plantar plate and hold it in place.
A Runner with Flexor Hallucis Longus Tendon Pain
After feeling sudden pain in the bottom of his foot, Scott’s MRI showed FHL damage as well as small holes in the plantar plates in the second and third MTP joints. In addition to that issue, the first-through-third toe joints (MTPs) began to hurt. MRI also showed evidence of arthritis in his toe joints.
Scott tried a bevy of different treatments over five years, including a PRP injection into the FHL tendon, acupuncture, physical therapy, switching to barefoot, boot immobilization, massage therapy, Motrin, many different kinds of shoes, chiropractic manipulation, electrical stimulation, and ultrasound. In addition, he also saw three foot-and-ankle specialists and was told that he needed surgery. We were literally his last hope.
How Does This Patient’s Problems Showcase Precise Interventional Orthopedics?
I get asked all the time by patients to define what we mean by interventional orthopedics. Take a look at the complexity of the diagrams above of the big toe. Each of these structures—the multiple big toe joints, the plantar plates, the ACL and PCL, the flexor tendons (like the FHL)—is a target for precise, image-guided injections. Even just looking at the FHL alone, you can inject it in the tendon sheath, the tendon itself, or both. In a joint of this size, the difference between placing cells in one structure versus the other is often 1–2 mm (less than 1/16th to 1/32nd of an inch). The knowledge that you need to have to perfect accurately injecting these tiny structures is interventional orthopedics at its best—using ultraprecise, image-guided injections to help patients avoid surgery.
Interventional Orthopedics and Regenexx-SD to the Rescue
I treated the patient with a precisely placed same-day stem cell injection procedure (Regenexx-SD) in March of 2015. The number of physicians in the U.S. who have the level of expertise to place cells with this degree of accuracy using both ultrasound and fluoroscopy and who understand where they need to go, likely numbers less than 100. How did it turn out? This is what we got back from Scott at his one-year registry questionnaire:

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.