Overlapping Genetic Patterns Found in Four Psychiatric Diseases
Psychiatric diagnosis has been a bit of a medical black box. Meaning, we have guidelines for diagnosis in the DSM, but at the end of the day, there are few blood tests or imaging studies that can confirm these diagnoses. Now researchers are using genetic signatures to bring new tools to the process of severe psychiatric diagnosis.
Brain Neurons: Our Brain Cells
Neurons are nerve cells within our nervous system, including our central nervous system (the brain and spinal cord) and our peripheral nervous system (the rest of our body). The neurons are responsible for both transmitting and receiving signals between the two systems. Today we are going to focus on our brain neurons, the nerve cells in our brain.
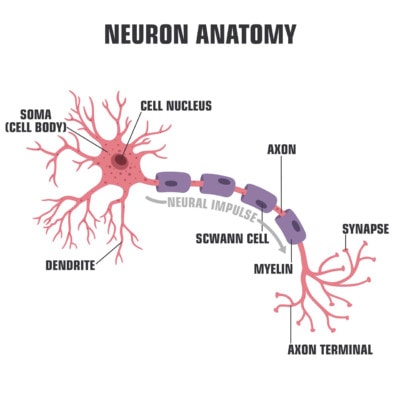
ShadeDesign/Shutterstock
Like every cell in the body, neurons have a specific job to do and as such are designed precisely to do that job. The body of the neuron consists of a nucleus, and multiple tree-like branching structures called dendrites encircle the cell body. A tail-like structure called the axon is also attached to the cell body, and at the end of the axon are axon terminals, or transmitters. These transmitters on one cell (senders) communicate with the dendrites of another cell (receivers) via a gap called the synapse. So signals are passed from one neuron’s axon terminals into the dendrites of another neuron where the signal passes through the cell body, down through the tail-like axon, into the axon terminals, and then across the synapses and into the dendrites of the next cell.
While it may make sense that brain neurons would communicate, or signal, differently in psychiatric diseases, our feature study today takes that a step further—discovering that brain neurons not only communicate differently (from the way brain neurons communicate in brains without a psychiatric disorder) but do so in a similar overlapping genetic pattern in four major psychiatric diseases.
Let’s take a look at the newest study.
Disruption in Brain-Cell Signaling: the Overlapping Genetic Pattern
Researchers in the new study analyzed the donated brains from 700 subjects. While living, 407 of the subjects were diagnosed with autism, schizophrenia, bipolar disorder, major depression, or alcoholism. The other 293 were control brains that had no psychiatric pathology. The results? Researchers found similar overlapping genetic signatures (specifically, disruptions in how the synapses between brain cells interact) in autism, schizophrenia, and bipolar brains. Additional similarities were found among the schizophrenia, bipolar, and major-depression brains. Overall the schizophrenia and bipolar brains had the most similar genetic patterns.
There were controls in place to account for antipsychotic medications, which were assumed in the brains with psychiatric disorders. The lack of genetic overlap with the alcoholism brains led researchers to conclude that the similarities in the other diseases—autism, schizophrenia, bipolar, and depression—were less likely due to substances or poor health. Researchers also concluded that these genetic similarities may be one reason it can be so difficult to diagnose a patient’s specific psychiatric disorder as many present in similar ways. As we learn more about these genetic connections through studies such as this one, however, it should make it easier for doctors to properly diagnose psychiatric disorders in the future.
What Else Do We Know About Neurons?
While one thing we do know is that there’s still a lot we don’t know about the nervous system, with every new study, we are learning more and more about our nervous system and the neurons that serve as its foundation. We’re even still today finding brand-new neurons we didn’t know existed.
Our nervous system is our sensation-signaling system, and as such pain and how and why we process it the way we do is a constant focus of study. Some of the more fascinating studies out there relate to pain and our neurons. For example, one study found that if we have chronic pain, our neurons that sense pleasurable touch can switch functions and start signaling these gentle touches as pain. There are so many solid studies today showing that pain is real that it has mostly buried the “pain is all in your head” theory (though a few “biopsychosocialists” are stubbornly poking their heads out again).
The upshot? Our knowledge of what’s wrong with the brain with regard to psychiatric diagnosis just got a whole lot more specific. What’s fascinating is that schizophrenia and bipolar disorder have genetic similarities. Not sure how that works or if that means that patients with a bipolar disease are in any way similar to those with schizophrenia. Also, it’s fantastic to see psychiatry entering the 21st century!

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
