Back Pain a Predictor of Poor Knee Replacement Outcomes
One of the hardest things for the modern orthopedic surgeon to do is to look outside of the joint that he or she is treating to another area that may be involved in the pathology. As an example, to see how a back problem can lead to knee or hip arthritis. To some degree this is a bad side effect of our overspecialization, as you often have surgeons who focus solely on the knee, hip, foot, shoulder, or spine. However, the research of the last decade really doesn’t support that these joints should be considered in isolation. Take, for example, a study published last week that shows back pain is a good predictor of poor knee replacement outcomes.
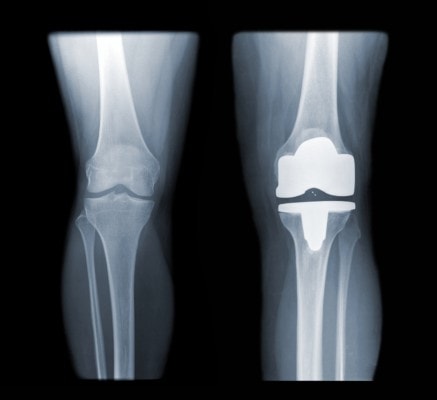
The knee on the right has been replaced. Skyhawk X/Shutterstock
The Body Is Connected
My life as a physician is so much simpler when all I think about and examine is one joint. For example, the right knee. The office visit is quicker, the options for therapy defined, the number of questions limited. If only it were really that simple.
The body is one machine. There really is no such thing as a hip or a knee or a spine. These are simply specialized parts of the whole machine. What impacts the spine affects the hip, and this influences the knee and so on. In particular, since the nerves that tell every muscle how to move each joint and that carry position-sensor information (e.g., my knee is bent at 80 degrees) live in the spine, it would make common sense that anything that impacts these nerves could and should impact a joint. So chronic back pain causing irritation of the nerves impacts the hip, knee, and hip. However, to most orthopedic surgeons, this common-sense idea is like speaking ancient Greek. They simply don’t often draw this connection. The good news is that the reality of the scientific literature is beginning to smack them upside the head with data that they hopefully will be hard-pressed to ignore. Take, for example, this new study linking back pain to poorer knee replacement outcomes.
Your Back Pain Impacts Your Knee…and Knee Replacement Outcomes
The new study looked at more than 1,000 knee replacements over two years. In almost 700, the patients were asked to fill out a spine-function questionnaire. Fifty-four percent of the knee replacement patients questioned had daily low-back pain. While patients without back pain demonstrated good results on their functional knee questionnaires (Oxford and Knee Society), patients with low-back pain reported significantly poorer knee replacement outcomes. In addition, the study showed that patients with back pain also had more pain and lower knee function before the knee replacement.
Despite these findings, I can count on both hands the number of times that I have seen an orthopedic surgeon talk to a prospective knee replacement patient about his or her low-back issues or even ask whether the patient has back pain. Far fewer times has a surgeon imaged the low back as part of his or her work-up for the knee. Why does this happen? See above. In our managed-care, hyperspecialized world, the physician looking at the knee often doesn’t really believe it’s his or her job to look at the low back.
The upshot? We have a big problem. Unlike our clinic where we frequently perform an exam on the low back, hip, knee, and ankle in a patient presenting with knee pain—the average orthopedic surgeon has between 5–15 minutes face time booked with a new patient. There simply isn’t the time or the inclination to look. So if you’ve been told you need a knee replacement, be aware that back pain can be a predictor of poor knee replacement outcomes! In addition, in our experience, newer regenerative-medicine techniques can often get rid of the need for the knee replacement, but often by also treating issues that may live in the low back!

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
