Patellofemoral Arthritis or Syndrome
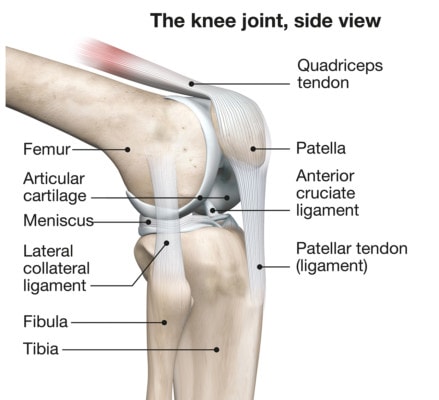
Axel_Kock/Shutterstock
The knee cap is an important structure that lives in the end of the quadriceps muscle and allows that muscle to better extend the leg and stay in track with the knee. The knee cap (patella) does all of this by sitting in a groove in the end of the femur bone known as the “trochlear groove”. When there has been an injury to the cartilage on the under surface of the knee cap or the cartilage has begun to wear away because of too much wear and tear arthritis, the patient can start to feel grinding under the knee cap and pain and swelling in the front of the knee. We’ve noted for many years that patients with a history of low back problems tend to suffer from more patellofemoral arthritis. The scientific research has shown a correlation between low back problems and problems in the knee cap. Treatment for patellofemoral syndrome can involve various types of physical therapy to help strengthen certain parts of the quadriceps muscle. In addition, taping of the knee cap may help better align it in it’s grove to prevent it being misaligned in the groove. Other types of care can include steroid shots (which likely hurt the knee), hyaluronic acid (HA) shots (SynVisc, OrthoVisc, Supartz, Hyalgan, etc..) which can provide better lubrication. In our experience, in order for HA shots to work reliably in patellofemoral syndrome, they should be injected using x-ray or ultrasound guidance into the pateloofemoral joint and not blind without any guidance. Other treatments include getting rid of trigger points in the quadriceps muscle and surgical approaches. The most common surgical approach is a lateral release, the concept being that releasing the fascial tissues on the outside of the knee will allow the knee cap to track better in it’s grove. Unfortunately, we havn’t seen good results with lateral release surgeries. Finally, more invasive surgeries can either try to restore lost cartilage (micro fracture) or replace the parts (anterior compartment knee replacement). Is there another way? We have injected the patient’s own stem cells into this area to improve the overall health of the cartilage (Regenexx-SD). Can it work? Here’s a statement from a middle aged patient who had failed surgery and had his own stem cells injected into the patellofemoral area about 2 months ago:
“Rt Knee Regenexx SD 99% no pain…I already took a couple runs skiing without difficulty.”
In conclusion, we have seen clinical evidence that injecting the patient’s own stem cells into the patellofemoral joint can reduce pain and increase function. We are publishing the results of a larger knee dataset, but it’s always nice to hear directly from patients that what you’re doing is helpful.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
