Should You Treat One or Both Arthritic Knees with Stem Cells?
There’s little published data on the use of a same day stem cell treatment for knee arthritis. What is published on knee arthritis stem cell therapy is focused on small numbers of patients with outcome measures-i.e. did this small number of patients report that they got better or not? I recently found amusing one adipose based stem cell site that claims to be collecting registry data and performing “research”. Yet the data shown looks more like what you would expect from a comment card found in a car dealership. Patient satisfaction with the office staff seems to take precedence over whether the patient reports less pain, better function on standardized questionnaires, or subjective improvement. It’s in that context that I present a new data analysis by our bio statistician. We have amassed a huge clinical registry of information that in many areas like the knee is getting big enough for us to do some really cool stuff.
Patients often come in to see us with knee arthritis on both sides. They always want to know if they can get both knees treated. We’ve often answered this question based on cell yield. Unlike a bedside centrifuge used by 95% of the doctors performing stem cell treatments, we have a lab where we can measure the cell number. This gives us a rough metric to at least provide some counsel on this issue. For example, if the stem cell yield is low, don’t get both knees injected. If it’s high, then do get both knees treated. However, is there a difference in outcome when one knee is treated versus both knees?
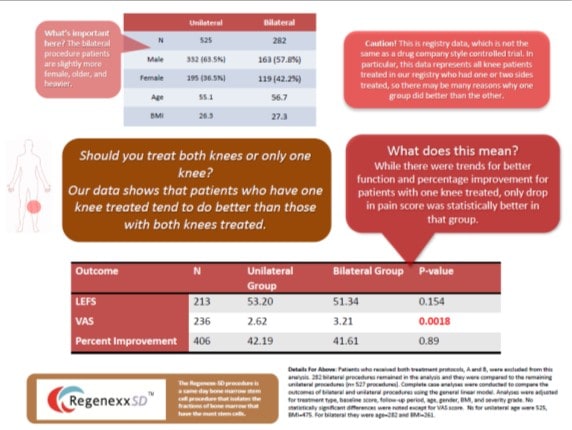
For this analysis, we looked at the data available on 525 patients who had only one knee treated and then compared them to 282 patients who had bilateral procedures. Our statistician then adjusted for treatment type, baseline score, follow-up period, age, gender, BMI, and arthritis severity grade. There was a statistically significant difference of about 20% for a better VAS 1-10 pain score when only one knee was treated. Click here for a bigger PDF of this knee stem cell infographic.
What does this mean? The other two scores we measure (LEFS functional scale and Likert % improvement) weren’t statistically different. However, since many patients come to us for pain in their arthritic knee, we should probably take note when the pain relief is lower in one group of patients versus another. Hence, at a 30,000 foot view, it means we will counsel patients to avoid bilateral procedures. Having said that, I can’t say yet whether the cause of the lower pain relief is performing procedures on both sides or whether it’s due to something else. For example, these bilateral patients may have a more severe form of arthritis than patients with problems in only one knee.
The upshot? If you have arthritis in both knees and are trying to figure out whether you should treat one or both knees, don’t despair, the effect we saw was small and in only one metric (i.e. there was no difference in function and reported % improvement between the groups). Having said that, for now, I would counsel patients to avoid bilateral procedures if feasible. In addition, the whole analysis points out how we’re quite different than other practices performing stem cell therapy for arthritis. We’ve been at this for almost a decade and have the largest repository of clinical outcomes information in orthopedic stem cell treatment that grows larger each day. Our goal is to use this information to give our patients rare insight into how they can make the best decisions about their care. There simply isn’t another practitioner of orthopedic stem cell therapy on earth who can say that right now.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.