Shoulder Labral Tear Surgery Pros and Cons
Quick links:
- What is a shoulder labral tear?
- What are the causes of labral tears?
- What is shoulder instability?
- How is a labral tear related to shoulder instability?
- What happens if you have shoulder instability after labral tear surgery?
I evaluated a patient this week who shows off the warts of our modern orthopedic care system; he was diagnosed with a shoulder labral tear and offered surgery. Why? His shoulder labral tear was the bright, shiny object, and nobody ever asked how he got the tear in the first place.
As he considered shoulder labral tear surgery pros and cons, I made the decision easy for him. Like many patients with a shoulder labral tear, the real diagnosis and its treatment was missed by the five-minute visit with the orthopedic surgeon. Let me explain.
What Is a Shoulder Labral Tear?
Think of the shoulder labrum as a lip around the socket of the ball-and-socket shoulder joint. It’s there to help guide the shoulder joint in movement and to make the shallow socket a bit deeper, allowing for better stability.
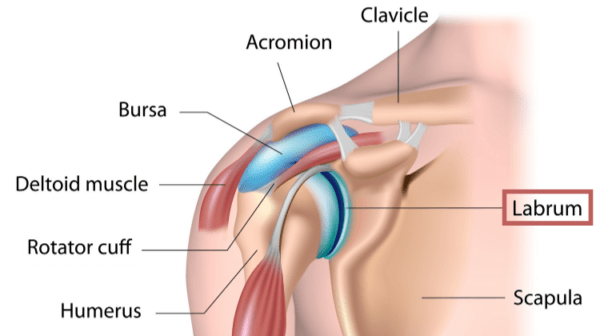
Image credit: Shutterstock
A tear in the labrum used to be ignored, considered just part of the spectrum of shoulder-joint arthritis, but then orthopedic surgeons figured out they could sew it together and an industry was born.
This isn’t to say that one doesn’t need to worry about healing a labral tear, but for most patients, surgically sewing it back together is likely not the right choice.
What Are the Causes of Labral Tears?
In our modern orthopedic surgery system, dictated by insurance contracts and managed care, most patients spend more time with an assistant than the surgeon. If they do see the surgeon, they’re one of 30 to 40 patients seen that day, each of which garner 5 to 10 minutes of attention. In this world of factory-type, high-volume medicine, asking how the labrum was torn in the first place just slows down the manufacturing line, so the question is rarely asked and answered.
While labral tears can occur in big traumas, like a car crash or a serious fall, many just kind of happen with seemingly innocuous activities. Why? The answer is simple, but it is often completely ignored by surgeons—hidden shoulder instability (1).
What Is Shoulder Instability?
The shoulder is a strange joint in that it has to allow for maximum movement in many directions, but it also has to remain stable at the same time. There’s a symphony of millisecond-timed and millimeter-oriented precision that allows the ball to stay in one tight region in relation to the socket as you move. While the rotator cuff and other muscles play a big role in this, there are also strong ligaments that make sure the ball joint stays perfectly seated in its shallow socket.
Surgeons usually pay attention to these ligaments only when the joint has been dislocated out of its socket, and everything else might as well be invisible. However, for each patient who has dislocated a shoulder and is left with a horribly unstable joint, in my experience there are five or six patients who also have an unstable shoulder that goes undiagnosed — hidden shoulder instability. Oftentimes this is from an old injury that the patient may have long since discounted.
However, at some point that unstable shoulder that seems fine comes back to bite them in the form of a labral tear (2). Hence one of the biggest cons in evaluating shoulder labral tear surgery pros and cons is hidden shoulder instability.
How Is a Labral Tear Related to Shoulder Instability?
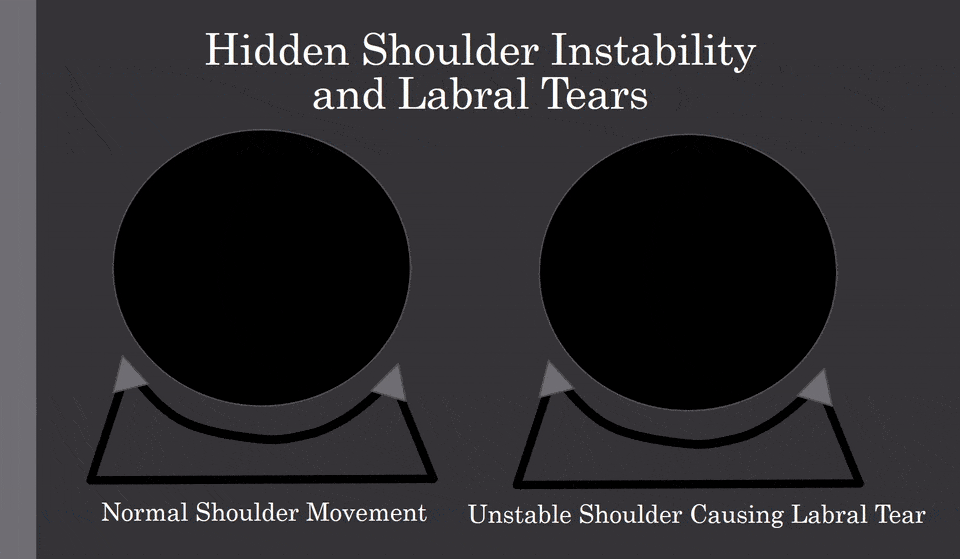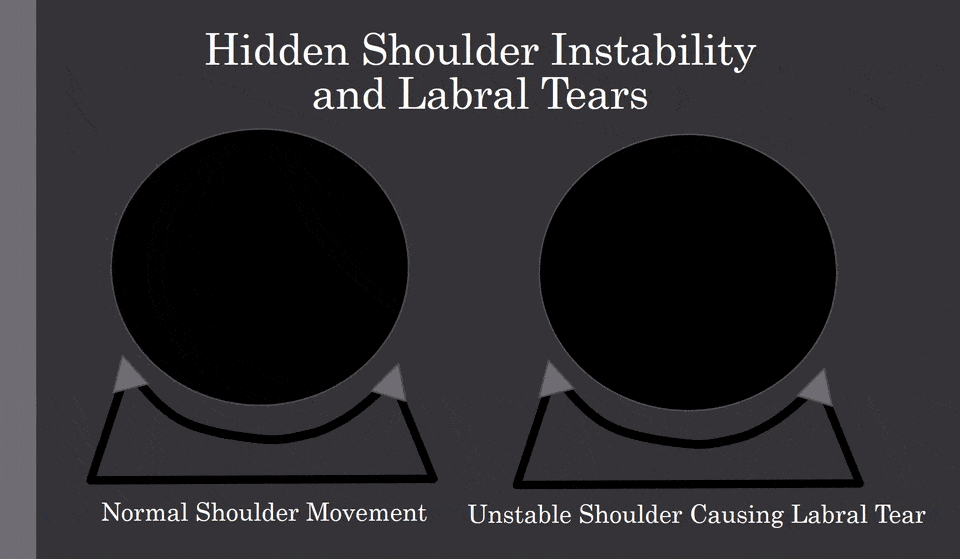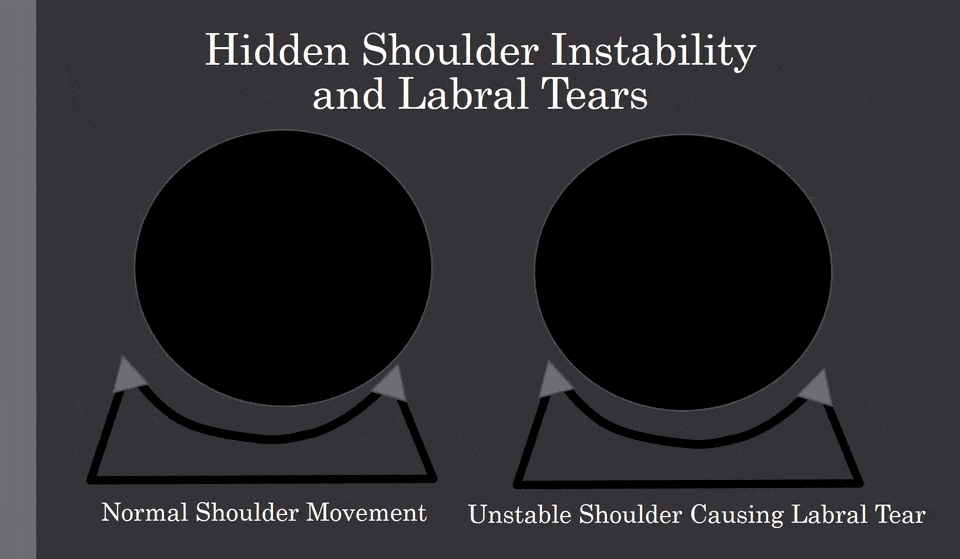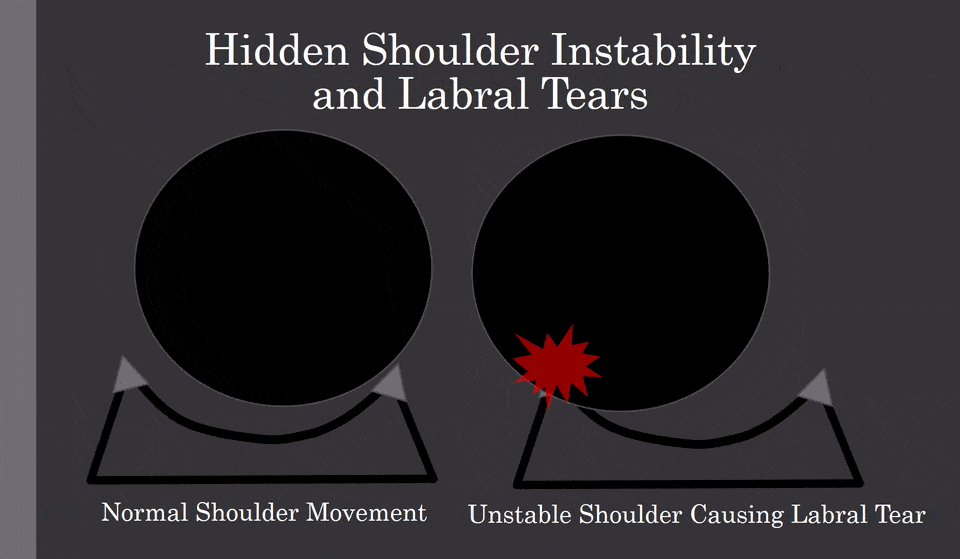
Check out the animated GIF above. The left shows the ball in a shoulder socket that is stable. It moves a little, bit it doesn’t bang into the labrum (lip of the socket, represented by the little triangles). The image on the right shows what can happen when the ligaments are loose (hidden shoulder instability) and the ball moves too far out of the socket and crashes into the labrum. Ouch! While you would think you would know if your shoulder is unstable, it rarely works out that way.
Two Patient Stories
Hidden shoulder instability is very common and is almost always missed by orthopedic surgeons. Case in point is two patients I evaluated this week. Both saw me because they were evaluating shoulder labral tear surgery pros and cons.
One was a patient in his 20s who rock climbs, and during a workout, he felt a tearing sensation in his shoulder and then had chronic pain. He was diagnosed with a torn shoulder labrum in the front and the back, and the recommendation was surgery. Nobody asked why a normally healthy guy would suddenly get a labral tear doing what everyone else does without injury.
On exam his shoulder ball was unstable in its socket, a fact the orthopedic surgeon missed. So hidden shoulder instability is why the ball suddenly shifted out of its socket and banged his labrum. How did he get the instability? He remembered a bad mountain-bike fall 7 years ago where his shoulder hurt, but he’d never had it checked out.
The second active guy I evaluated in clinic this week was similar. He tore his left shoulder labrum while dead-lifting 450 pounds. His right shoulder had no issues and was also loaded with the same weight. Why did he tear his left shoulder labrum and not his right? He, too, saw an orthopedic surgeon who told him he needed surgery.
On exam his left shoulder joint was unstable and knew immediately when it happened. While in a mixed martial arts (MMA) fight, his opponent wrenched his shoulder (the “Kimura Lock” as shown above) the year before the dead lift. He, too, had shoulder pain for a few weeks, but blew it off. Again, the hidden shoulder instability was completely missed by the orthopedic surgeon.
What Happens if You Have Shoulder Instability After Labral Tear Surgery?
It doesn’t take a rocket scientist to understand that if you have hidden shoulder instability and someone surgically repairs the labral tear, as soon as the shoulder gets into a weird loaded situation, the socket will shift out of place and the labrum will tear again.
How can you prevent this? By skipping the 20th-century orthopedic surgery and using 21st-century interventional orthopedics (3). This means placing precise imaging-guided injections of your own advanced platelet and stem cell mixes directly into the labral tear and also into the weak ligaments. The downtime is a fraction of that of surgery, and in our experience of treating hundreds of shoulders, the results are as good as or better than surgery—and with the hidden shoulder instability issue fixed.
The upshot? Hidden shoulder instability is very common and almost always missed by surgeons who spend 5-10 minutes with a patient. So if you’re looking at shoulder labral tear surgery pros and cons, a huge con is that you may have hidden shoulder instability that was undiagnosed, meaning that this shoulder labral tear repair will be your first of many shoulder surgery rodeos.
Save yourself the brain damage and get a good exam (which means a 60-minute evaluation by the doctor-not the assistant). In addition, why go with 20th-century technology when addressing your labral tear? Why not go with advanced interventional orthopedics and skip the surgery?
__________________________________________________
References
(1) Van Blarcum GS, Svoboda SJ. Glenohumeral Instability Related to Special Conditions: SLAP Tears, Pan-labral Tears, and Multidirectional Instability. Sports Med Arthrosc Rev. 2017 Sep;25(3):e12-e17. doi:10.1097/JSA.0000000000000153
(2) Clavert P. Glenoid labrum pathology. Orthop Traumatol Surg Res. 2015 Feb;101(1 Suppl):S19-24. doi:10.1016/j.otsr.2014.06.028
(3) Schrøder CP, Skare Ø, Reikerås O, Mowinckel P, Brox JI. Sham surgery versus labral repair or biceps tenodesis for type II SLAP lesions of the shoulder: a three-armed randomised clinical trial. Br J Sports Med. 2017;51(24):1759–1766. doi:10.1136/bjsports-2016-097098

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.