Spondylolysis Recovery Time: Avoiding the Knife
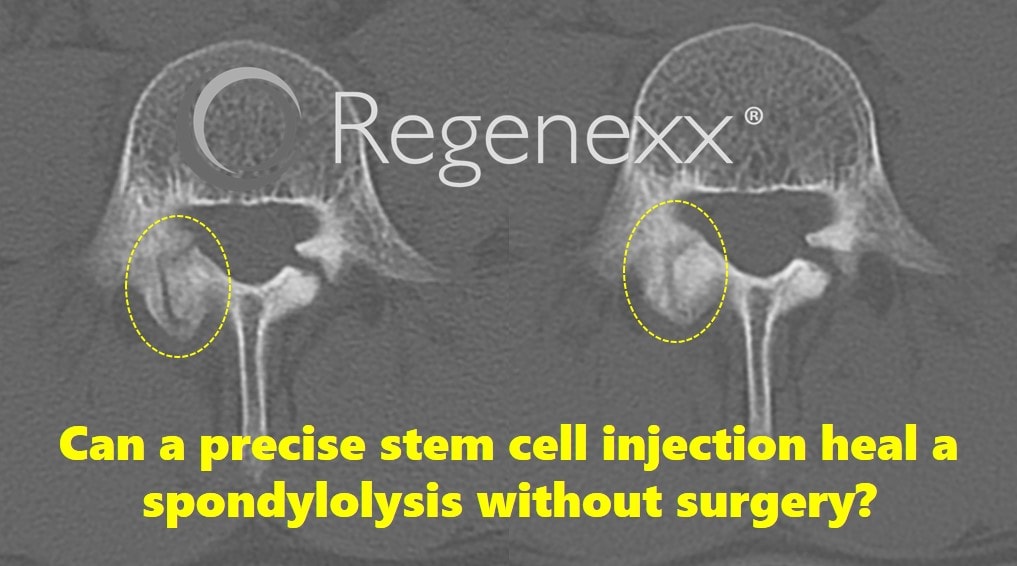
Spondylolysis is common in disturbingly young athletes who are born with weakened or disconnected areas of their spine. Sometimes this break in the spine bone heals, and sometimes it doesn’t. When the spot doesn’t mend, the patient usually undergoes a big surgery that can cause serious problems. So if your spondylolysis recovery time is taking too long, how can you ramp up your body’s ability to heal without major surgery? By getting an ultraprecise injection of your stem cells, just like the collegiate wrestler whose CT scans I’ve included above.
What Is Spondylolysis?
Some of us are born with extra backbones, some with holes in the spine, and some with weak areas in our spines. When this happens and a lot of force is placed on the weak area in sports, like gymnastics, football, wrestling, and others, the weak area can break. This condition is called spondylolysis.
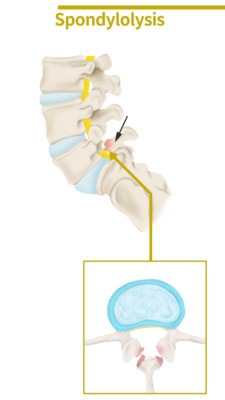
Chu KyungMin/Shutterstock
The part of the spine that most commonly breaks is called the pars interarticularis (aka pars), which means in Latin, “the part between the articulations.” It’s named this because it’s the piece of bone between the joints in the back of the spine (facet joints). Many times, one side of the spine will be disconnected while the other has only weakened bone. When this happens, the weak side can break during exercise, causing chronic pain. Sometimes this fracture will heal on its own, but when it doesn’t, often the patient gets an invasive surgery.
What is spondylolysis recovery time? The fracture should heal, like any other, in about 6–12 weeks. If you still have pain after this period despite being in a back brace to stabilize the area, then the fracture is called a delayed union (meaning slow healing). If it’s still there at six months, it’s called a nonunion and is very unlikely to heal on its own. In this situation, patients are often treated with surgery.
Why Operating on a Pars Fracture Causing Spondylolysis Is a Bad Idea
Let’s face it, modern spine surgery is like a bull in the proverbial china shop of this delicate structure. Why? There is no way to install hardware to fuse the spine without destroying the critical muscles (multifidus) that stabilize it. Also, damage also occurs to the key muscle covering (thoracodorsal fascia) that helps provide additional spine stability. So even if all the surgeon is trying to do is to bolt together the fracture to give it a chance to heal, this still damages these structures.
What’s the best way to fix the fracture? Put away the carpentry tools and augment your body’s natural ability to heal. How is this possible? A very precise injection of your body’s stem cells.
Our Wrestler’s Spondylolysis Story
I’ve already blogged on much of the details of NH’s spondylolysis nightmare and his subsequent treatment without surgery; he learned the hard way about spondylolysis recovery time. This patient injured his back wrestling and had a spondylolysis break that wouldn’t heal, which forced him out of collegiate competition. He was faced with invasive surgery or trying a new technology. He chose the latter by using his stem cells carefully injected into the break with fluoroscopic guidance.
Percutaneous Pars Defect Repair (Perc-PDR)
Our clinic has pioneered percutaneous pars defect repair (Perc-PDR). The procedure involves using high concentrations of the patient’s bone marrow stem cells precisely injected with demineralized bone matrix into the pars defect using a micro trocar. C-arm fluoroscopy is used to guide the injection.
Since the procedure avoids hardware and open surgery by using a micro trocar, which is about the size of a standard needle, it doesn’t damage the muscles or important fascia. Perc-PDR also focuses on using the innate healing potential of your body to close the fracture naturally. I personally performed the procedure on this collegiate wrestler in June of 2016.
The result? You can see above (top of page) that three months later, the right-sided pars fracture (which is on the left of the image and inside the white-dashed circle) healed. The left-sided break shown is the side of his spine that was never connected. His pain promptly went away after the first month, and he skipped having a surgeon permanently muck up his stabilizing back muscles and fascia.
The upshot? We’ve healed many non-healing fractures with precise stem cell injections. We’ve also published on some of these patients. Now we’re using an advanced form of the same technology to help young athletes heal their spondylolysis fractures without surgery. These kids get to avoid the serious long-term side effects of surgery while hastening their spondylolysis recovery time.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
