Treating Low Back Pain During and After Pregnancy
Credit: Shutterstock
I’ve seen many patients after pregnancy who have chronic low back pain. In addition, low back pain during pregnancy can also be disabling. So what are the options for treatment? I’ll review that today and go over a recent patient that was treated by our Washington, DC Metro area Regenexx affiliate. Let’s dig in.
Low Back Pain in Pregnancy
There are two main types of low back pain that occur in pregnancy (1). The first is simple, which involves the pressure of the baby on the spine and/or the biomechanical changes that happen with weight gain. The solution here is simple, which is delivery of the baby and the weight loss that should occur in a nursing mother. When things get more complex is when low back pain is caused by the pelvic ring and SI joints. Let’s review that topic.
SI Joint Pain and Pregagancy
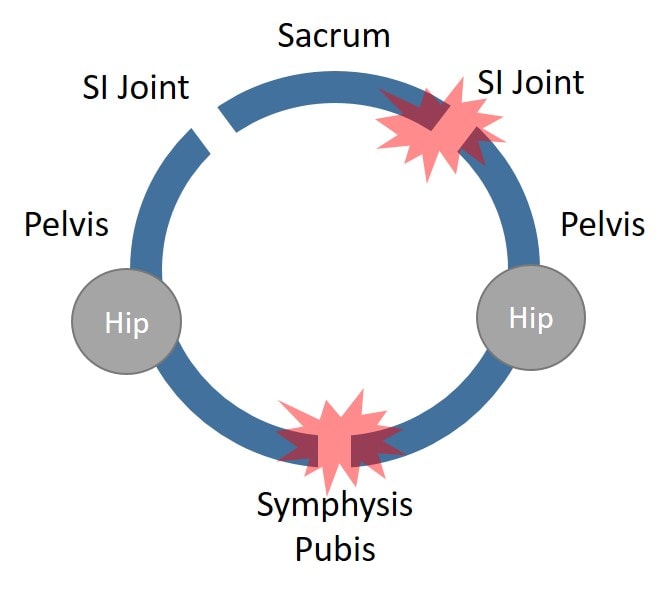
That ring above is an abstract representation of the “pelvic ring” shown from above. It’s made up of two joints in the back called the SI or Sacroiliac joints and one in the middle up front called the Symphysis Pubis. The Iliac bones make up the left and the right and the Sacrum or tailbone makes up the back part of the ring.
In women, the baby’s head must pass through this pelvic ring. From an evolutionary standpoint, that can be problematic, especially given our big brains and heads, so nature has figured out a workaround. In the last trimester, there’s a hormone called Relaxin that’s released that loosens the ligaments that hold the three joints together (both SI joints and the Symphysis Pubis). That allows the extra room needed to make vaginal delivery possible as these joints can now stretch.
During pregnancy, the laxity in the SI joints for the last 3 months can be a problem, especially if the joints of the pelvic ring were lax or injured previously. In those women, pain can happen in one or more of the SI joints or the Symphysis Pubis and is caused by the extra abnormal joint motion allowed by the loose ligaments. Also, during pregnancy, the baby can damage any one of these three joints and/or ligaments, leading to continued post-partum laxity that causes pain.
SI Joint Pain in Pregnancy
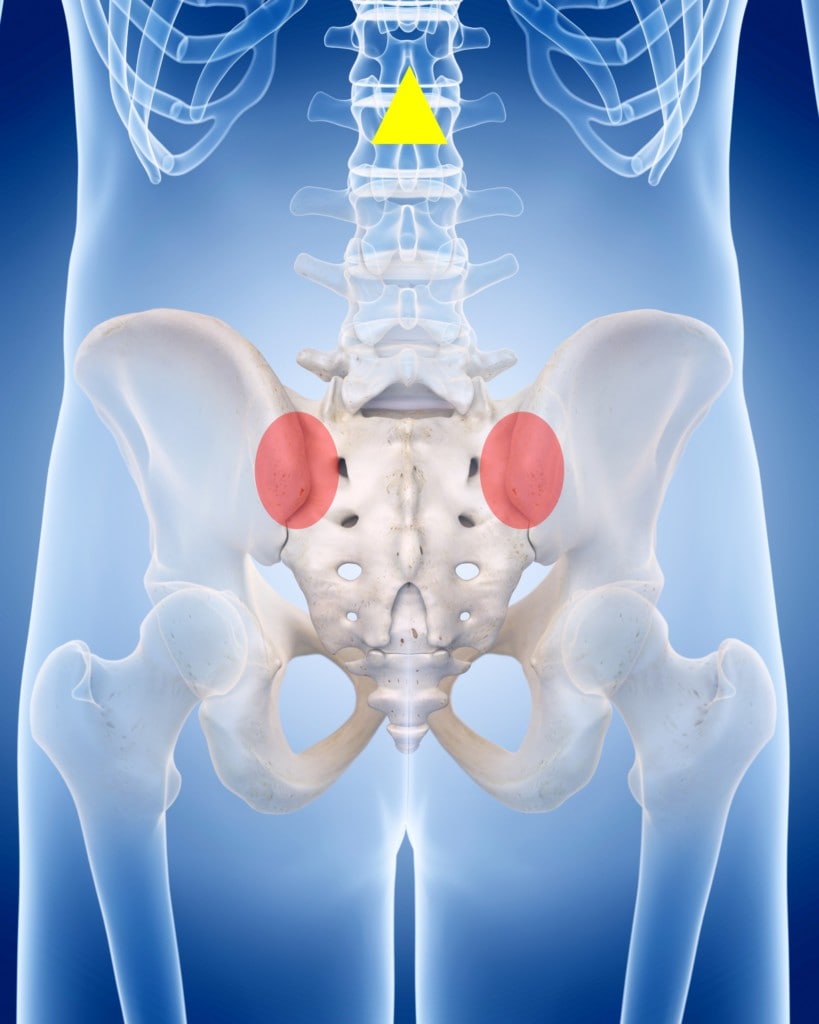
Credit: Shutterstock with edits by author
The most common area where the pain is located if it is the SI joint is shown above in red. That’s located at the back of the PSIS or in an area near the Dimples of Venus. The pain can be either side or both. In addition, Si joint pain can also cause either pain in the front of the hip and/or down the leg, often mimicking a pinched nerve in the low back (Sciatica or Radiculopathy).
How Is SI Joint Pain Diagnosed?
The most common way that SI joint pain during pregnancy is diagnosed is through an exhaustive hands-on physical exam. The patient is usually tender to the touch over the SI joint and the PSIS areas. The mobility of the painful joint is also increased. MRI’s can also show swelling in the bone around the SI joint (2). A diagnostic numbing injection or “block” of the SI joint is also possible by using pregnancy-friendly anesthetics like Ropivacaine. This eliminates the pain for a few hours to confirm the diagnosis.
The Epidural Problem
Before we go on and dive deeper into how low back pain during or after pregnancy is treated, it’s worth mentioning chronic low back pain that can be caused by a botched epidural. As you may know, epidural anesthesia is often used to help the pain that happens during childbirth. This involves taking a needle and injecting an anesthetic into the epidural space around the spinal nerves.
Injuries can happen when the epidural needle is inserted too deeply or when there are multiple attempts at trying to establish the epidural flow of the medication. This can cause localized damage to the dura, or the pain-sensitive covering of the spinal cord and nerve roots. I’ve seen countless women through the years with chronic post-pregnancy back pain due to the epidural site. Given that the epidurals are usually given at L2, that pain is often higher than pain from the SI joint pain as shown by the yellow triangle above.
How Is Low Back Pain Treated Before and After Delivery?
Most low back pain goes away with delivery. Hence, the number one treatment is symptomatic. That might include taking pregnancy-safe over-the-counter meds and physical therapy.
However, there are patients with severe and disabling low back pain during pregnancy. For that problem, I’ll describe a case report below.
Finally, there’s chronic low back pain after pregnancy. That’s again most commonly due to SJ joint ligaments that were injured during delivery. That treatment is usually injections of the ligaments that hold the joints together. Finally, I’ve treated chronic epidural pain with a platelet-based precise x-ray guided epidural injection right at that L2 spot to break up scarring and help that area heal.
A Case Report
While most pregnancy-related pain happens in the last trimester at 24-38 weeks, this is the case of a woman who had severe back pain earlier. However, her problems were caused by the same issue that plagues women before and after delivery, SI joint pain. This case comes from our Washington, DC metro area provider, Mayo Freidlis, M.D., and his Stem Cell Arts practice.
This is the case of a 37-year-old woman who was 10 weeks pregnant. She was having left-sided low back pain and Sciatica down the leg and was unable to ride in the car, sit very long, and had difficulty sleeping. Her MRI showed bulging low back discs at L4-L5 and L5-S1. Prior to becoming pregnant, she had been treated with epidural steroid injections with reasonable results. However, now that she was 10 weeks pregnant, the high-dose epidural steroids delivered with x-ray guidance may have an impact on the baby, so these were not recommended. Hence, she was told to tough it out, despite having disabling back pain.
The patient went to see Dr. Freidlis and his examination showed ligament laxity as well Radiculopathy (irritated spinal nerves). As with most pregnant women, her exam localized to the Sacroiliac joint. She was treated with precise ultrasound-guided PRP injections to all her lumbar ligaments and a Caudal epidural using her own platelets. She reported 90% improvement.
PRP Use in Pregnancy
As you can see from the case above, using many prescription medications in pregnancy is problematic. However, there is a natural solution for low back pain derived from your own body. That’s called PRP. To learn more about what that is and how that works, see my video below. That video also covers PRP’s helpful cousin, called platelet lysate (which was used in the epidurals described above):
So is PRP safe for use in pregnancy? It’s been used as a fertility treatment for years and a recent study showed when used that way, it actually increased the odds of getting pregnant and was safe (3-5). Given that PRP involves using the mother’s own platelets, this would be considered a natural therapy that doesn’t expose the mother or baby to anything that isn’t normally used by the body every day.
The upshot? Low back pain in pregnancy is common. When it’s disabling during or after pregnancy and conservative care doesn’t work, natural injection-based solutions that use the mother’s own platelets may help. These treatments can use ultrasound guidance and in my experience, are very effective for women with chronic low back pain.
_____________________________________
References:
(1) Katonis P, Kampouroglou A, Aggelopoulos A, et al. Pregnancy-related low back pain. Hippokratia. 2011;15(3):205-210.
(2) Kiil RM, Arnbak BA, Zejden A, Schiøttz-Christensen B, Hendricks O, Jurik AG. Pregnancy-related sacroiliac joint findings in females with low back pain: a four-year magnetic resonance imaging follow-up study. Acta Radiol. 2021 May 17:2841851211017108. doi: 10.1177/02841851211017108. Epub ahead of print. PMID: 34000822.
(3) Zamaniyan M, Peyvandi S, Heidaryan Gorji H, Moradi S, Jamal J, Yahya Poor Aghmashhadi F, Hossein Mohammadi M. Effect of platelet-rich plasma on pregnancy outcomes in infertile women with recurrent implantation failure: a randomized controlled trial. Gynecol Endocrinol. 2021 Feb;37(2):141-145. doi: 10.1080/09513590.2020.1756247. Epub 2020 May 2. PMID: 32363968.
(4) Chang Y, Li J, Wei LN, Pang J, Chen J, Liang X. Autologous platelet-rich plasma infusion improves clinical pregnancy rate in frozen embryo transfer cycles for women with thin endometrium. Medicine (Baltimore). 2019 Jan;98(3):e14062. doi: 10.1097/MD.0000000000014062. PMID: 30653117; PMCID: PMC6370111.
(5) Nazari L, Salehpour S, Hosseini S, Sheibani S, Hosseinirad H. The Effects of Autologous Platelet-Rich Plasma on Pregnancy Outcomes in Repeated Implantation Failure Patients Undergoing Frozen Embryo Transfer: A Randomized Controlled Trial. Reprod Sci. 2022 Mar;29(3):993-1000. doi: 10.1007/s43032-021-00669-1. Epub 2021 Oct 14. PMID: 34651260.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
