Why Back Surgery Side Effects Are so Common: BFH Syndrome
I write about what I see in clinic and around me. One of the interesting things from this week was a low back pain patient who had surgery that was so invasive it left a hole in his low back. I coined the term BFH syndrome (Big [Insert Expletive] Hole) to describe this back surgery side effect. Let me explain.
What Is a Laminectomy/Discectomy?
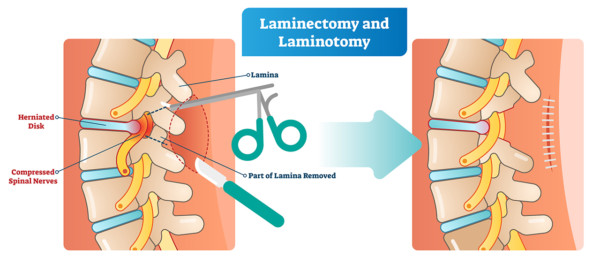
VectorMine/Shutterstock
Back surgery is often performed when there is a bulging disc that’s pressing on a nerve. The surgeon will remove a part of the disc (discectomy) and then sometimes, to give the nerve more room, the lamina (laminectomy). The lamina is the bony back part of the spinal canal.
Why Does Back Surgery Have Such a Bad Rep?
Just about everyone knows someone or knows of someone who has had a back surgery disaster. Hence, back surgery side effects are up close and personal. In the case above, while removing the disc to take pressure off a nerve can help reduce nerve pain in the short run, it weakens the structure of the disc and makes it more likely to fail (recurrent disc herniation). In addition, while taking out the back wall of the spinal canal may seem like a good idea at the time as it gives the nerve more room, critical stabilizing muscles that attach there are usually destroyed. Since these muscles protect the disc, facet joints, and nerves, removing them just means more problems down the road. Basically, a short-term solution turns into back surgery side effects.
BFH Syndrome
Most people have no idea that spinal surgery is damage to accomplish a goal. Meaning, I look at MRIs all day that show the serious damage done by back surgery. In this patient’s case, a “hole” where critical tissues should be. Let’s dive deeper into what caused this void.
The images above show the issue. On the left-hand side, you see a side image of the spine. Note that the yellow-dashed line represents the hole caused by surgery. You can easily see dark bones and muscles above and below the hole, but that area looks white. Now, look at the image on the right. This is a view looking down on the tissues (axial or “saw you in half” view). The yellow-dashed line again outlines the hole. You see the dark low back muscles surrounding the white void. In fact, the hole is exactly where the critical stabilizer of the low back, called the multifidus, should live. Meaning, at this level that muscle has been obliterated, causing serious back surgery side effects.
Why is the multifidus critical? See my video below for more information:
Why did the surgeon leave a hole? He placed retractors to open up a tunnel from the skin to the lamina, which he then removed. By removing the muscles and bone in the way, he yanked out the multifidus.
Is the Hole a Problem?
Yep, without the critical multifidus stabilizer, this level (and now the one below it) are unstable. The patient has chronic low back pain because the tissues that are normally protected by the multifidus are getting beat up. Also realize that while I can help heal some of the damage and reduce the nerve irritation using precise orthobiologic injections, I can’t fill the hole.
How You Can Avoid a BFH
Regrettably, the term “minimally invasive” in spine surgery is often more of a marketing tool than based in reality. Pretty much all of the surgeons who claim to be able to perform minimally invasive spine surgery leave a BFH or an SMH. However, there are a handful of surgeons around the country who do perform true minimally invasive low back surgery, which is done through a portal the size of a ballpoint pen, and this type of procedure will spare the critical stabilizing muscles.
In addition, the best way to avoid a BFH is to avoid the surgery altogether. In 90+% of our patients with these issues, we treat them with precise X-ray–guided platelet and stem cell injection or platelet procedures. However, please be wary of con artists offering “stem cell” injections for back pain, which more often than not take these forms:
- A nurse in a chiropractor’s office injecting dead amniotic or umbilical cord tissue blindly into the back muscles. See my video for info on this scam:
- A plastic surgeon or orthopedic surgeon who uses fat stem cells and starts an IV claiming that the stem cells will magically find their way to the site and also performs blind low back muscle injections.
- A pain management doctor offering dead amniotic or umbilical cord tissue injections using X-ray guidance. Why do I say this is dead tissue? Because we took the time and spent the money to do the research that these doctors don’t have the ability to do. See my video below for more information:
The upshot? Avoid having a big hole carved in your low back. One way to do this is to skip the surgery by getting precise, real stem cell injections. In addition, many patients do just as well with advanced platelet procedures. Finally, if all of that fails, find that very rare surgeon to whom the term “minimally invasive” is more than a marketing sales tool.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
