Looking for Knee Replacement Alternatives? You Should Be!
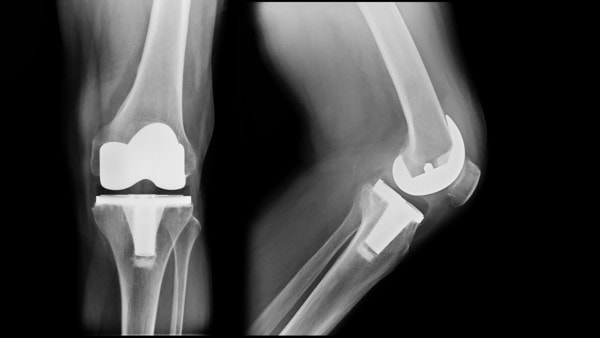
Total knee replacement on both knees. Tridsanu Thopet/Shutterstock
Knee replacement is a huge surgery as it involves amputating the knee joint and inserting a prosthesis. Hence, knee replacement alternatives have become popular. First, let’s dive into knee replacement and review the good, the bad, and the ugly. Then we’ll review some knee replacement alternatives.
What is Knee Replacement?
Knee replacement is also called total knee arthroplasty (1). This means that the doctor amputates or cuts out the existing knee joint, reams the bone, and inserts a prosthetic device in place of the natural joint. Instead of replacing the whole knee, small parts of the joint such as the medial, lateral, or anterior compartment can also be replaced.
Why Should You Be looking for a Knee Replacement Alternatives?
Pain After Knee Replacement
Patients get this surgery to reduce pain, so it comes as a surprise to many that a good chunk of knee replacement patients still have knee pain after this invasive surgery. For example, in one recent study, nearly 40% reported that they still had 3-5/10 despite getting a knee replacement (2). In a different study, some 44% of patients still had moderate pain 3-4 years after surgery (3). Hence, if you think that this surgery is a “sure thing” for solving your knee pain, you should be looking for knee replacement alternatives.
Knee Replacement Risks
There is no getting around it, this is a big surgery. Here are some of the more common risks:
- Dramatically increased risk of heart attack and stroke right after surgery (9,10)
- Metal ions in the blood (4-6)
- Allergy to the metal in the prosthesis (7,8)
- Infection (22)
Activity Levels After Knee Replacement-Not All It’s Cracked Up to Be
You can’t help but see commercials of smiling older people riding bikes, climbing mountains, or doing something else active with their new knee. However, is that reality? Not so much. For example, in one government-funded study, there was no increase in activity after knee replacement (11). Another study showed that if you weren’t running before a knee replacement you won’t run after one. Meaning, very few patients markedly increased their activity levels after knee replacement surgery (12).
RELATED
>> Regenexx Knee Patients’ Registry of Outcomes – Over 11,125 tracked nationally
>> Before and After MRI Knee Images
What are Knee Replacement Alternatives?
Steroid Injections
Steroids injections, also known as corticosteroids and “cortisone”, a likely one of the most common knee replacement alternatives. While steroids are potent anti-inflammatories, regrettably high-level research has shown that they destroy cartilage and don’t work as well as we once thought (13). Hence, this is not a viable long-term knee arthritis treatment option.
Viscosupplementation
Viscosupplementation is also one of the most common knee replacement alternatives. These are knee gel shots also known as hyaluronic acid with brand names like SynVisc, OrthoVisc, Supartz, and Euflexxa. Do these shots help? The research is all over the map, meaning some studies say that they help and other research says that they don’t help (14,15). However, the good news is that there is no research that supports that they hurt cartilage in the same way that steroid injections do and most studies point in the direction of HA helping arthritis (16). One caveat is that, in my experience, these injections tend to work for a few cycles, but then have diminishing returns. Meaning the first injection helps for 6-12 months, the repeat works for less time, and by the third or fourth repeat cycle of injections, the patient is no longer getting much relief.
Knee Nerve Ablation
One of the latest trends in knee replacement alternatives is ablating the pain nerves around the knee. This is a technology where the doctor places probes close to several nerves around the joint and electrical energy is used to destroy (ablate) them. These nerves take pain signals from the knee to the brain, so if the nerves are ablated, the pain goes away until the nerves grow back. The research showing that this treatment helps knee arthritis pain is made up of small studies (17,18). However, you should be aware that no high-level research studies have been done at this point. Meaning the research that we have on this procedure is still in the early stages.
Orthobiologics
Orthobiologics are substances that are used to promote the healing of or reduce the destruction of orthopedic tissues and consequently, they are also being used as knee replacement alternatives. These can be from the patient (autologous) or from a donor (allogeneic). The two main orthobiologics that are from the patient are PRP and Bone Marrow Concentrate. Another commonly used orthobiologic is derived from birth tissues (i.e. amniotic or umbilical cord), but since the research on using those tissues in actual knee arthritis patients is in its infancy, those won’t be discussed here.
Platelet Rich Plasma (PRP)
Platelet-rich plasma (PRP) is an injection of the patient’s own concentrated platelets. These platelets have healing growth factors that are believed to assist with cartilage repair, reduce inflammation, and improve the chemical environment of the knee. There is good quality and mature research that PRP injections can help patients with mild knee arthritis improve their pain and function. However, they don’t seem to work as well for more severe arthritis (19, 20).
PKA (Percutaneous Knee Arthroplasty)
When the arthritis is more severe, there is a newer procedure called PKA, which stands for Perc-Knee Arthroplasty. In this procedure, the doctor uses stem cell rich bone marrow concentrate from the patient to not only inject the joint but also lax ligaments, damaged meniscus tissue and tendons. This is a precise ultrasound and fluoroscopy-guided procedure and not a quick knee shot. This new procedure has been shown to be effective in a randomized controlled trial and unlike PRP it seems to work well no matter how severe the arthritis is or isn’t (21). In addition, the procedure generally has effects that last between 2-7 years, but then the PKA procedure often needs to be repeated.
The upshot? There are lots of knee replacement alternatives. Of these, orthobiologics like PRP and bone marrow concentrate seem to be choices that won’t hurt in the long-run more than they help.
_______________________________________________________
References:
(1) Medical Advisory Secretariat. Total knee replacement: an evidence-based analysis. Ont Health Technol Assess Ser. 2005;5(9):1–51. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3382388/
(2) Sakellariou VI, Poultsides LA, Ma Y, Bae J, Liu S, Sculco TP. Risk Assessment for Chronic Pain and Patient Satisfaction After Total Knee Arthroplasty. Orthopedics. 2016 Jan-Feb;39(1):55-62. doi: 10.3928/01477447-20151228-06.
(3) Wylde V, Hewlett S, Learmonth ID, Dieppe P. Persistent pain after joint replacement: prevalence, sensory qualities, and postoperative determinants. Pain. 2011 Mar;152(3):566-72. doi: 10.1016/j.pain.2010.11.023.
(4) Friesenbichler J, Maurer-Ertl W, Sadoghi P, Lovse T, Windhager R, Leithner A. Serum metal ion levels after rotating-hinge knee arthroplasty: comparison between a standard device and a megaprosthesis. Int Orthop. 2012;36(3):539–544. doi: 10.1007/s00264-011-1317-4
(5) Savarino L, Tigani D, Greco M, Baldini N, Giunti A. The potential role of metal ion release as a marker of loosening in patients with total knee replacement: a cohort study. J Bone Joint Surg Br. 2010 May;92(5):634-8. doi: 10.1302/0301-620X.92B5.23452.
(6) Savarino L, Tigani D, Greco M, Baldini N, Giunti A. The potential role of metal ion release as a marker of loosening in patients with total knee replacement: a cohort study. J Bone Joint Surg Br. 2010 May;92(5):634-8. doi: 10.1302/0301-620X.92B5.23452.
(7) Atanaskova Mesinkovska N, Tellez A, Molina L, Honari G, Sood A, Barsoum W, Taylor JS. The effect of patch testing on surgical practices and outcomes in orthopedic patients with metal implants. Arch Dermatol. 2012 Jun;148(6):687-93. doi: 10.1001/archdermatol.2011.2561.
(8) Hinarejos P, Ferrer T, Leal J, Torres-Claramunt R, Sánchez-Soler J, Monllau JC. Patient-reported allergies cause inferior outcomes after total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2016 Oct;24(10):3242-3246. https://www.ncbi.nlm.nih.gov/pubmed/26531183
(9) Belmont PJ Jr1 Goodman GP, Kusnezov NA, Magee C, Bader JO, Waterman BR, Schoenfeld AJ. Postoperative myocardial infarction and cardiac arrest following primary total knee and hip arthroplasty: rates, risk factors, and time of occurrence. J Bone Joint Surg Am. 2014 Dec 17;96(24):2025-31. doi: 10.2106/JBJS.N.00153.
(10) Waterman BR, Belmont PJ Jr, Bader JO, Schoenfeld AJ. The Total Joint Arthroplasty Cardiac Risk Index for Predicting Perioperative Myocardial Infarction and Cardiac Arrest After Primary Total Knee and Hip Arthroplasty. J Arthroplasty. 2016 Jun;31(6):1170-1174. doi: 10.1016/j.arth.2015.12.013.
(11) Kahn TL, Schwarzkopf R. Does Total Knee Arthroplasty Affect Physical Activity Levels? Data from the Osteoarthritis Initiative. J Arthroplasty. 2015 Sep;30(9):1521-5. doi: 10.1016/j.arth.2015.03.016
(12) Harding P, Holland AE, Delany C, Hinman RS. Do activity levels increase after total hip and knee arthroplasty? Clin Orthop Relat Res. 2014 May;472(5):1502-11. doi: 10.1007/s11999-013-3427-3.
(13) McAlindon TE, LaValley MP, Harvey WF, et al. Effect of Intra-articular Triamcinolone vs Saline on Knee Cartilage Volume and Pain in Patients With Knee Osteoarthritis: A Randomized Clinical Trial. JAMA.2017;317(19):1967–1975. doi: 10.1001/jama.2017.5283
(14) Rutjes AW, Jüni P, da Costa BR, et al. Viscosupplementation for Osteoarthritis of the Knee: A Systematic Review and Meta-analysis. Ann Intern Med. 2012;157:180–191. doi: 10.7326/0003-4819-157-3-201208070-00473
(15) Strand V, McIntyre LF, Beach WR, Miller LE, Block JE. Safety and efficacy of US-approved viscosupplements for knee osteoarthritis: a systematic review and meta-analysis of randomized, saline-controlled trials. J Pain Res. 2015;8:217–228. Published 2015 May 7. doi:10.2147/JPR.S83076
(16) Altman RD, Dasa V, Takeuchi J. Review of the Mechanism of Action for Supartz FX in Knee Osteoarthritis. Cartilage. 2018;9(1):11–20. doi:10.1177/1947603516684588
(17) El-Hakeim EH, Elawamy A, Kamel EZ, Goma SH, Gamal RM, Ghandour AM, Osman AM, Morsy KM. Fluoroscopic Guided Radiofrequency of Genicular Nerves for Pain Alleviation in Chronic Knee Osteoarthritis: A Single-Blind Randomized Controlled Trial. Pain Physician. 2018 Mar;21(2):169-177. https://www.ncbi.nlm.nih.gov/pubmed/29565947
(18) Gupta A, Huettner DP, Dukewich M. Comparative Effectiveness Review of Cooled Versus Pulsed Radiofrequency Ablation for the Treatment of Knee Osteoarthritis: A Systematic Review. Pain Physician. 2017 Mar;20(3):155-171. https://www.ncbi.nlm.nih.gov/pubmed/28339430
(19) Filardo G, Kon E, Buda R, Timoncini A, Di Martino A, Cenacchi A, Fornasari PM, Giannini S, Marcacci M. Platelet-rich plasma intra-articular knee injections for the treatment of degenerative cartilage lesions and osteoarthritis. Knee Surg Sports Traumatol Arthrosc. 2011 Apr;19(4):528-35. doi: 10.1007/s00167-010-1238-6.
(20) Southworth TM, Naveen NB, Tauro TM, Leong NL, Cole BJ. The Use of Platelet-Rich Plasma in Symptomatic Knee Osteoarthritis. J Knee Surg. 2019 Jan;32(1):37-45. doi: 10.1055/s-0038-1675170.
(21) Centeno C, Sheinkop M, Dodson E, et al. A specific protocol of autologous bone marrow concentrate and platelet products versus exercise therapy for symptomatic knee osteoarthritis: a randomized controlled trial with 2 year follow-up. J Transl Med. 2018;16(1):355. Published 2018 Dec 13. doi:10.1186/s12967-018-1736-8
(22) Peersman G, Laskin R, Davis J, Peterson M. Infection in total knee replacement: a retrospective review of 6489 total knee replacements. Clin Orthop Relat Res. 2001 Nov;(392):15-23. https://www.ncbi.nlm.nih.gov/pubmed/11716377

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
