New Research: An MRI with Stenosis Doesn’t Diagnose Your Pain
We have all been taught that what shows up on an MRI is incredibly important—so much so that countless invasive surgeries are launched based on a picture and a cursory exam. Despite this, study after study continues to show just how bad MRI is at predicting who’s in pain. However, one of the sacred cows of low-back-pain diagnosis has been that if an MRI shows signs of the nerves being compressed by arthritis (stenosis), then the patient must have pain. Now that sacred cow of determining treatment based on MRI with stenosis has been felled by a new study that shows again that using an MRI to diagnose pain is bad medicine.
What Is Lumbar Stenosis?
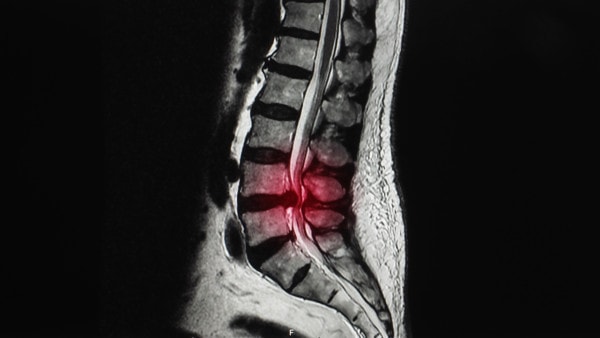
Yok_onepiece/Shutterstock
When the low-back joints, discs, and ligaments, through wear and tear, grow too big, they can put pressure on the spinal canal, the main tunnel through the back bones; this is called lumbar stenosis. The spinal canal houses the bundle of important nerves that branch off the spinal cord, and those that branch off the low back (the lumbar spine) travel to the legs. In lumbar spinal stenosis, weakness or numbness can occur in the legs when these nerves become pinched. In diagnosing spinal stenosis, our medical-care system depends on the findings of an MRI. Normally, the spinal canal is nice and wide and rounded; however, in spinal stenosis, the canal becomes triangle shaped, causing all the nerves to become tightly compressed.
Patients who have spinal stenosis find some relief in sitting because this position opens the canal space a bit. While standing or walking, patients will feel the need to lean forward a bit to relieve some tension on their spine.
What Other Studies Have Shown That MRI Is Useless in Diagnosing the Cause of Pain?
Before we dig into the new study, let’s look at a sampling of other studies we’ve covered here over the years that show the ineffectiveness of MRI when looking at pain.
- Knee pain isn’t always correlated to findings on MRI as some patients have a lot of knee pain with little to no MRI findings and some have little to no knee pain yet show severe issues on MRI.
- Shoulder MRI results alone are bad at accurately diagnosing the cause of shoulder pain.
- Way back in 2009 I covered a study showing that in patients where MRI shows meniscus tears, 60% have no history of active knee pain.
- Common findings of spinal stenosis on MRI can’t predict presence or degree of pain and disability.
Now, what does the new study show?
The Most Recent Study Showing That Using an MRI with Stenosis to Diagnose Who Has Pain Due to Stenosis Is Useless
The new study reviewed four published papers where two reported that there was no relationship between the degree of stenosis (i.e., less room for the nerves means more pain) and two that found a relationship. After taking apart the data from the four studies and putting it all back together again, using an MRI with stenosis to determine treatment would necessitate finding a relationship between the two, and the authors couldn’t find any relationship between the symptoms of compressed nerves and the degree of compression on the MRI images.
The upshot? We as physicians need to stop reinforcing a concept that no longer has robust literature support—that chronic nontraumatic pain can easily be diagnosed by looking at an MRI and that MRI is therefore an appropriate tool for us to base invasive surgery. This incorrect idea has bled into the minds of patients and popular culture and as such is responsible for countless walking wounded and complications due to unnecessary surgeries!

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
