Spinal Stenosis Injections: Never Trust a Back MRI!
Patients considering spinal stenosis injections often come into the office with back pain with thier MRI CDs, believing that this shiny data disc holds the key to their salvation. This makes sense, as many are desperate at that point, their low back having betrayed them by leaving them unable to do what they need to or enjoy. But what if I told you that if you have a common low back condition called stenosis, new research shows that your MRI is basically worthless?
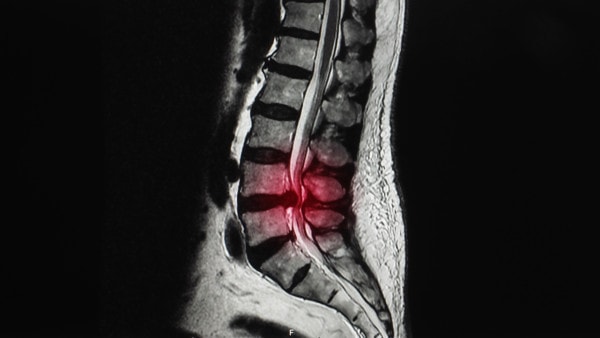
MRI of lumbar spine showing compression in the spinal canal. Yok_onepiece/Shutterstock
The term lumbar stenosis means that the low back joints, disc, and ligaments have all grown too big through wear and tear and now put pressure on the main bony tunnel in the back bones. This tunnel, called the spinal canal, is used by all of the important nerves that come from the spinal cord (which usually terminates just north of the low back) to travel to your legs. So in spinal stenosis, these nerves can become pinched causing leg weakness or numbness. Spinal stenosis patients love to sit, as the flexion opens up more space in the spinal canal, while they hate to stand or walk, as this closes off the space. If they do walk, they commonly use a shopping cart to lean forward as this feels better.
Our medical care system has become very dependent on MRI to make the diagnosis of spinal stenosis. It’s frankly not hard to see, as the normally round and wide spinal canal turns into a little triangle, compressing all of the nerves into a tight spot. However, given that low back MRI is so darn bad at predicting who should have pain in prior studies, some smart researchers tried to see if these common findings of spinal stenosis on MRI predicted who should have more pain and disability. For example, a smaller and tighter canal where the nerves looked pinched should mean more pain and inability to walk and a more open canal with more space should mean less back pain and better ability to walk. What did they find? NO CORRELATION BETWEEN THE SIZE OF THE SPINAL CANAL AND BACK PAIN OR WALKING ABILITY. While this finding is consistent with other studies, it’s sure to shake up the world of spinal stenosis, where physicians often put patients through big and risky surgeries solely based on an MRI and their symptoms.
The upshot? While an experienced physician taking and hour or so carefully teasing out what’s on your MRI that matches your complaints or your exam is likely helpful, the modern “5 minutes” with the surgeon who operates on what’s on the MRI is now being shown through research to be a massive waste of heath care dollars and a dangerous exposure of patients to unnecessary risk. Case in point-spinal stenosis. What ever is causing the symptoms in spinal stenosis it sure isn’t the amount of tightness in the spinal canal, which begs the question of why we’re operating on the spinal canal to open it up? On the other hand, this is likely why we see such solid clinical results with our Regenexx-DDD procedure as it takes a completely different approach, treating the multiple spine elements causing pain like joints and nerves while addressing the degenerative instability (the extra motions causing active nerve pinching) that’s likely at the heart of why patients with spinal stenosis hurt.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
