Radiofrequency Neurotomy of the Knee: What Could Go Wrong?
Radiofrequency is a technology I’ve covered many times on this blog. It’s basically a way for doctors to burn away the nerves causing pain. It’s becoming increasingly popular in the knee, so let’s review that today. In addition, we’ll review combing RF of the knee nerves with orthobiologics and whether that makes sense.
What is RFA or RFN?
RFA stands for Radiofrequency Ablation, and RFN for Radiofrequency Neurotomy. In the context of pain medicine, these are both the same procedure where the doctor guides a needle called a “probe” to a nerve that transmits pain and uses radiofrequency energy to heat the tip of the probe to destroy the nerve. How does that help? The nerve is cooked and ablated, so its cells cannot carry pain signals. That generally means that the body part innervated by those nerves is no longer painful, but that only lasts until the nerve grows back.
RF of the Knee
The knee has geniculate nerves that take most of the pain signals, as shown below:
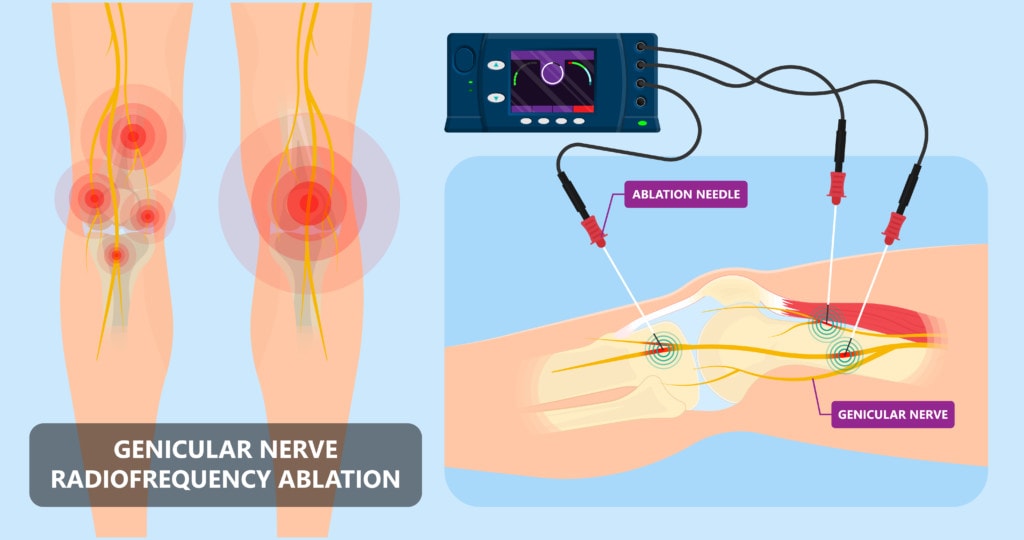
Credit: Shutterstock
These nerves can be “cooked” using RF, and this can reduce knee pain. In general, the research shows that this procedure works but is of low quality (1).
How well does this work? There is only one randomized trial with a small number of 19 patients who received either RF or a sham, and only 59% of those patients reported more than 50% relief at three months (2). Other studies were of lesser quality, including one that compared RF to knee steroid injections which showed that it worked better at six months, but half of the patients were lost to follow-up because they had other procedures like knee replacement by 12 months (3). Other studies have been sponsored by industry or have lacked blinding (4-8).
So, in summary, the research we have that supports that RFA works is of lower quality with only one placebo-controlled trial. Compare that to PRP for the treatment of knee OA with three dozen RCTs and six successful placebo trials.
What Could Go Wrong?
It’s well known that if you denervate a joint that the structure deteriorates more rapidly. In medicine, this is called a Charcot joint (9). In the third world, we know that this can be caused by venereal disease that destroys the knee nerves, and in the first world, diabetes does the same thing. In fact, you can create diabetes in a rat by feeding it a high-fat diet and running it on a treadmill, which destroys the nerves in the leg through diabetic peripheral neuropathy, which ultimately destroys the joints in the legs (10).
In summary, we know that the destruction of the nerves in the knee leads to a mess of a knee joint. So rather than increasing the time before the patient needs a knee replacement, we’re likely accelerating the need for that surgery by using RFA/RFN.
RFN+Orthobiologics?
It recently came on my radar that several Florida clinics are offering knee RFN and then combining that with a PRP shot. So putting those concepts together, the RFN likely accelerates arthritis while the PRP may help arthritis? That’s like buying better tires for your car and then driving them over a bed of nails. As a physician-patient, I would never sign up for that treatment.
The Divide in Pain Medicine: What Insurance Will Cover vs. What’s Good for the Joint
I’ve blogged many times on the problem with high-dose knee steroid shots. We know they destroy the knee joint and make that patient more likely to get an infection once the joint gets replaced. However, steroid shots are still very common because they’re widely covered by insurance. So physicians are choosing to destroy the joint rather than using something like PRP, which could help the joint.
It’s the same game with RFN of the knee; only the reimbursement is much better. For example, for a knee steroid shot, the doctor is typically paid about $70 in the office. For a knee RFA/RFN, if you own the surgery center where the procedure is done, the total reimbursement between professional and facility fees can be several thousand dollars.
In both cases, the physician is choosing to do something that physicians have been taught will wreck the joint in exchange for a 6 in 10 chance of helping the knee pain. Why? The answer will be the same old adage, “because it’s covered by insurance.”
The upshot? As I get older and my knees need treatment, I won’t be signing up to have anyone destroy my geniculate nerves. I’ll stick with PRP, which has much better evidence supporting it works, and because, more likely than not, it will decelerate the progression of arthritis rather than accelerate it like RFA/RFN!
_____________________________________________________
(1) Li G, Zhang Y, Tian L, Pan J. Radiofrequency ablation reduces pain for knee osteoarthritis: A meta-analysis of randomized controlled trials. Int J Surg. 2021 Jul;91:105951. doi: 10.1016/j.ijsu.2021.105951. Epub 2021 Apr 18. PMID: 33882358.
(2) Choi WJ, Hwang SJ, Song JG, Leem JG, Kang YU, Park PH, Shin JW. Radiofrequency treatment relieves chronic knee osteoarthritis pain: a double-blind randomized controlled trial. Pain. 2011 Mar;152(3):481-487. doi: 10.1016/j.pain.2010.09.029. Epub 2010 Nov 4. PMID: 21055873.
(3) Aaron Conger, DO, Jeremy Gililland, MD, Lucas Anderson, MD, Christopher E Pelt, MD, Christopher Peters, MD, Zachary L McCormick, MD, Genicular Nerve Radiofrequency Ablation for the Treatment of Painful Knee Osteoarthritis: Current Evidence and Future Directions, Pain Medicine, Volume 22, Issue Supplement_1, July 2021, Pages S20–S23, https://doi.org/10.1093/pm/pnab129
(4) Chen AF, Khalouf F, Zora K, DePalma M, Kohan L, Guirguis M, Beall D, Loudermilk E, Pingree MJ, Badiola I, Lyman J. Cooled radiofrequency ablation provides extended clinical utility in the management of knee osteoarthritis: 12-month results from a prospective, multi-center, randomized, cross-over trial comparing cooled radiofrequency ablation to a single hyaluronic acid injection. BMC Musculoskelet Disord. 2020 Jun 9;21(1):363. doi: 10.1186/s12891-020-03380-5. PMID: 32517739; PMCID: PMC7285532.
(5) Chen AF, Khalouf F, Zora K, DePalma M, Kohan L, Guirguis M, Beall D, Loudermilk E, Pingree M, Badiola I, Lyman J. Cooled Radiofrequency Ablation Compared with a Single Injection of Hyaluronic Acid for Chronic Knee Pain: A Multicenter, Randomized Clinical Trial Demonstrating Greater Efficacy and Equivalent Safety for Cooled Radiofrequency Ablation. J Bone Joint Surg Am. 2020 Sep 2;102(17):1501-1510. doi: 10.2106/JBJS.19.00935. PMID: 32898379.
(6) El-Hakeim EH, Elawamy A, Kamel EZ, Goma SH, Gamal RM, Ghandour AM, Osman AM, Morsy KM. Fluoroscopic Guided Radiofrequency of Genicular Nerves for Pain Alleviation in Chronic Knee Osteoarthritis: A Single-Blind Randomized Controlled Trial. Pain Physician. 2018 Mar;21(2):169-177. PMID: 29565947.
(7) Ray D , Goswami S , Dasgupta S , Ray S , Basu S. Intra-articular hyaluronic acid injection versus RF ablation of genicular nerve for knee osteoarthritis pain: A randomized, open-label, clinical study. Indian J Pain 2018;32(1):36.
(8) Sari S , Aydin ON , Turan Y , et al. Which one is more effective for the clinical treatment of chronic pain in knee osteoarthritis: Radiofrequency neurotomy of the genicular nerves or intra-articular injection? Int J Rheum Dis 2018;21(10):1772–8.
(9) Babazadeh S, Stoney JD, Lim K, Choong PF. Arthroplasty of a Charcot knee. Orthop Rev (Pavia). 2010 Sep 23;2(2):e17. doi: 10.4081/or.2010.e17. PMID: 21808708; PMCID: PMC3143972.
(10) Stauch CM, Fanburg-Smith JC, Walley KC, King JL, Murie B, Kim M, Koroneos Z, Waning D, Elfar JC, Aynardi MC. Animal model detects early pathologic changes of Charcot neuropathic arthropathy. Ann Diagn Pathol. 2022 Feb;56:151878. doi: 10.1016/j.anndiagpath.2021.151878. Epub 2021 Dec 16. PMID: 34953234.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
