SI Joint Injection Side Effects: PRP vs. Steroid Shots for SI Joint Syndrome
Steroid shots are the mainstay of current injection-based spine care. Why? Certainly not because steroid shots are the best therapy we have for reducing pain and helping an injured part of the spine heal. Also, while many online sources would have you believe that SI Joint injection side effects are minimal, that’s not been our experience. Hence, it’s always great to see physicians worldwide testing autologous biologics, like platelet rich plasma, against steroids for SI joint pain.
SI Joint Syndrome
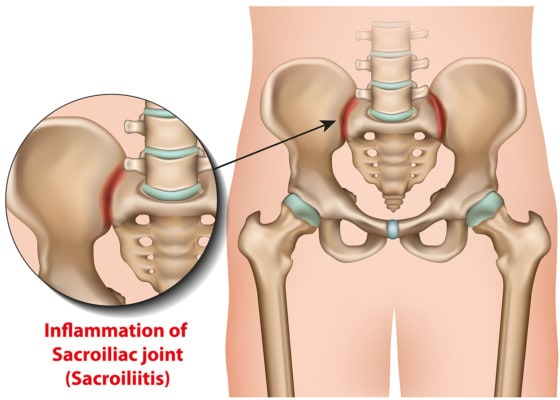
Medicalstocks/Shutterstock
The SI joint (sacroiliac joint) lives between the tailbone and the back of the hip and is critical for transferring energy between your legs and your spine. It’s not a hinge joint, like the knee, but instead works by giving in this direction or that. The joint can be injured via trauma (e.g., a car crash or a fall on the butt) or can get arthritic, like any other joint, through normal wear and tear. The joint can also be injured through overload from a low-back fusion.
When physical therapy fails, the mainstay of treatment for this problem is an X-ray–guided, anti-inflammatory steroid shot. The upside is that these injections can help some patients obtain months of relief. The downside is that SI Joint injection side effects from high-dose steroids are an issue. For example, these steroid injections can injure local ligament and cartilage cells as well as impact bone density in older women.
One way that’s been proposed to help chronic SI joint pain that won’t resolve with a steroid shot or can’t be effectively managed with conservative care is minimally invasive SI joint fusion. However, while the research for this new solution looks somewhat encouraging, the downside side effects appear to be no better than other fusions and even worse than SI Joint injection side effects. Hence, the world needs another option.
PRP SI Joint Injections
PRP means platelet rich plasma, a substance made by concentrating the patient’s platelets. We’ve injected several hundred SI Joint pain patients with one platelet-based procedure or another over the last decade. In fact, this works so well that it’s been a long time since I remember injecting an SI Joint with high-dose steroid. Hence, it’s great to see some research that backs up what we observe in the clinic every day.
The new study randomized 40 patients to get either a steroid shot or PRP injection via ultrasound guidance. The patients were then followed only short-term up to three months (which is a weakness of this study). Back pain was less with PRP at six weeks and three months. Only 25% of the patients who had a steroid injection were still experiencing significant relief at three months compared to 90% of the PRP group. Functional scores worsened at three months for the steroid group while these same scores improved gradually for the PRP group. In summary, PRP beat steroid in this small study.
The Older SI Joint Therapy Option—Prolotherapy
It’s hard to write this blog without giving a tried and true SI joint pain option a plug. While PRP is sexier, prolotherapy (prolo) is based on the idea that injecting a solution that causes a brief inflammatory reaction will facilitate healing. Also, there’s an even better study out there that shows that prolo works better than steroid injections.
The prolo study looked at a few more patients and for longer than the PRP study. One group was injected with dextrose prolotherapy solution in the SI joint and the other with high-dose steroid. The positive effects of prolo weren’t just seen for three months, but for 15 months where almost 60% of the prolo group had significant relief whereas only 10% of the steroid group reached that goal.
The upshot? While steroid injection for SI joint pain is a mainstay, it’s a not a great treatment for long-term relief when compared to simple treatments like PRP and prolo that focus on ramping up the body’s natural ability to heal versus suppressing it. So if you have SI joint pain, realize that what your insurance covers is likely a second-rate treatment. Also, SI Joint injection side effects are quite real, so based on this early research, avoiding the “roids” would likely be smart.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
