Tennis Elbow Surgery vs. Alternative Treatment Options
I get asked all the time by patients, “Should I have surgery for tennis elbow?” So let’s delve into what tennis elbow is and whether surgery is a good idea or the dumbest mistake you’ll ever make. The good news is that in the second decade of the 21st century, you have a lot of options.
What is Tennis Elbow?
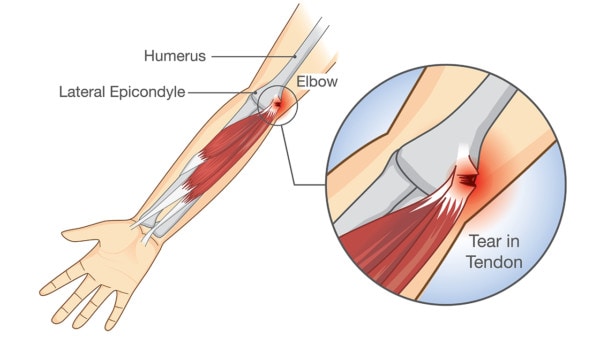
Solar22/Shutterstock
Tennis elbow is actually called lateral epicondylitis, which means that the bump on the outside of your elbow, which is where the muscle tendons that extend your fingers and wrist are attached, is irritated with small tendon tears. Research into this type of tendinopathy shows that the issue isn’t really swelling like we once thought, but is instead degeneration and small tears in the tendon.
You really can’t fully understand why you have tennis elbow before you understand a little bit about how the body works as one big machine, with the whole arm being a portion of that machine with specialized parts. Trying to consider only what’s happening at the elbow is like looking at your lone bald tire on your right front wheel and not considering the screwed up front end alignment that caused the problem. Your neck and shoulder complex are also part of the upper extremity machine, so any issues at the elbow must always include an examination of the neck and shoulder as well. If your orthopedic surgeon or some physician assistant only examines your elbow and then recommends care, it’s time to find a new doctor!
One of the more common things we see as a cause of tennis elbow is low level nerve irritation in the neck. This is because the nerves in the neck power the muscles that attach at the outside of your elbow. When the signals aren’t getting through, the muscles in your forearm don’t work properly and then they begin to yank too much at their attachment to the outside elbow bone. This leads to tennis elbow. What if you don’t really have a lot of neck issues? Take note, because your first warning sign that the neck nerves are being irritated or pinched may well be your tennis elbow.
Tennis Elbow Treatment Options
Steroid Shots – Avoid These!
Before they consider surgery, patients with tennis elbow are commonly sent to physical therapy or given a prescription of NSAIDs like Motrin, Mobic, or Celebrex. When this doesn’t work, a steroid shot is usually offered, but there are some good reasons you should skip this treatment. While a steroid shot is a potent anti-inflammatory, it can kill off healthy tendon cells, making the tendon weaker in the long run. Studies have also shown that while it can help for a few months, the pain will come back stronger than before the shot after it wears off.
Tennis Elbow Surgery – Quickly Becoming a Thing of the Past
Surgery for tennis elbow commonly involves using a scalpel to cut “fenestrations” or small holes or lines into the tendon. The idea is that these injuries will cause healing. While at some level this makes sense, surgery rates for tennis elbow have been plummeting for years due to new treatments that are much less invasive and much better studied as being effective.
Platelet Rich Plasma – Our Recommended Treatment for Tennis Elbow
This brings us to the quality, concentration and delivery of PRP used for treating tennis elbow. In our experience, PRP that is amber color and largely free of red and white blood cells, is more effective than the red PRP, which causes a much bigger inflammatory response.
Other Treatment Options
Prolotherapy, which is the injection of a solution that’s more concentrated than your body’s tissues and that causes a brief inflammatory healing reaction, is effective in our experience. ESWT (Extracorpeal Shock Wave Therapy) is a treatment where the arm is immersed in a water tank and sound waves that disrupt tissue are aimed at the injured area. While shock wave therapy has been touted as effective, a recent randomized controlled trial didn’t show any benefit to the therapy. Physical therapy exercises and stretches may also be a good option for alleviating pain and restoring function.
When All Else Fails
Some cases are recalcitrant to PRP injections. In those instances, treating the irritated nerves in the neck can often be the key to ensuring success. Sometimes tendons may just be too injured and torn up to allow the healing effects of PRP to work well. In these rare cases, our experience has found that injecting the patient’s own bone marrow stem cells may help.
The upshot? Surgery for tennis elbow is becoming a thing of the past, which is a good thing considering the invasiveness of the procedure. Avoiding steroid shots that can injure the tendon cells is important. PRP is definitely the way to go considering the excellent research that supports this newer procedure that uses the healing power of your own body!

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
