Unnecessary Knee Replacements Are a Surgical Epidemic
The sales tail has always wagged the dog in medicine. Meaning sales targets for drugs and devices and aggressive sales reps have always determined more about what care is offered to patients than actual medical need. One of the biggest areas of abuse has always been orthopedics. In addition, one of the biggest abuse areas in orthopedics is joint replacements, where a number of companies have sales reps in countless American operating rooms forcing product down the throats of surgeons. Hence, it’s no surprise that academics now believe that more than 1 in 3 knee replacements aren’t needed.
600,000-Plus Knee Replacements Per Year in the U.S. and Counting
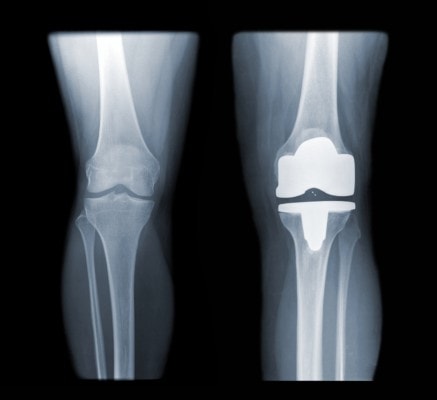
The knee on the right has been replaced. Skyhawk X/Shutterstock
Knee replacements have more than doubled in the last 15 years, and these invasive surgeries are being marketed toward and performed on younger and younger patients. A recent study also suggests that by the year 2030, on the current trajectory, we could see a 600% increase in the number of knee replacements (though I believe interventional orthopedics will reverse this trajectory and we will actually see a decrease in knee replacements by 2030). Why such a drastic increase in these surgeries?
While they should be reserved for only the worst cases (e.g., severe and debilitating bone-on-bone arthritis), the current surgical orthopedics trend is to perform these in less-severe cases, in patients who think getting a new knee is the answer to eliminating their pain and increasing their activity. After all, the device advertisements show “patients” doing just that after a supposed joint replacement. Unfortunately, especially in younger and more active patients, many are finding reality doesn’t mimic the marketing. Why? It seems many of these surgeries are unnecessary knee replacements as the patients don’t actually need a knee replacement.
How Knee Replacement Devices Get Sold
At a recent large orthopedics conference, one of the large medical-device companies bought out an entire street of restaurants to highlight its new robotic knee replacement system! Think about how much that costs to pull off and you’ll understand how much money is at stake if you can increase sales by more than one-third. Hence, knee replacement device companies have had in place large programs to push these surgeries into the only growth sector that exists for the industry—younger and more-active patients.
How this gets done is likely a mystery to most consumers. However, as a physician, I get to witness it firsthand. It’s been estimated that a third or more of the cost of a knee prostheses is the cost of aggressive sales tactics among company reps. These sales people will traditionally attend every case (if possible). Does the surgeon really need this help? Not usually. Which is why orthopedic sales reps are usually chosen to be easy on the eyes. In addition, a rep that can stay in front of a surgeon sells more product.
Another lynchpin in the sale chain is the creative ways that companies find to get money to doctors in exchange for using their devices. This can include “medical director” fees, money to fill out forms about prosthesis failure rates, or speaking fees. While this has become harder for companies to pull off due to government rules, this just means that companies tend to get more creative. An organization called Propublica records these payments, so you can look up your surgeon right now. As an experiment, I googled knee replacement in my town and then looked up the first surgeon who popped up on the Propublica website. He got $143.000 in payments from device companies in 2015! This is actually small potatoes as some of the bigger-named surgeons collect 3–4 times that much in consulting fees from device manufacturers.
More than One in Three TKRs Are Unnecessary Knee Replacements?
This study examined information from a large data set called the Osteoarthritis Initiative. Only those who’d undergone knee replacement were included in this study, which consisted of 205 patients. The purpose of the study was to determine whether each knee replacement was appropriate or not. Researchers studied each patient’s preoperative data, including pain, function, radiology images, range of motion, age, and so on and categorized each to one of the following categories: appropriate, inconclusive, and inappropriate.
The result? Over 34% of knee replacements were found to be inappropriate, leading researchers to conclude that better standard criteria need to be developed for determining the necessity of knee replacement. Think about that percentage! Over 34% of patients who get a knee replacement don’t actually need one! That’s more than one in three of knee replacement patients. And we don’t know what the “inconclusive” numbers represent (which accounted for 27% of knee replacements); however, it’s reasonable to assume that if all of the information had been available, some of those patients would have fallen into the “inappropriate” category as well, so the 34% of unnecessary knee replacements could likely be higher.
Knee Replacement and Its Mixed Bag of Side Effects
So maybe you’re in pain, and you just want that new knee, even if there is a chance you’re in that 34% category. After all, new is better right? Not in this case. Getting a new knee means potentially getting a mixed bag of dangerous side effects along with it…and it may still not address your pain.
Chronic knee pain is the biggest reason patients give for ultimately deciding to undergo knee replacement. Unfortunately, however, the most common complication reported by knee replacement patients is ongoing chronic knee pain, with nearly 40% averaging 3 out of 10 pain and some even reporting numbers as high as 5 out of 10. And the farther out from knee replacement surgery (two years or longer), the higher the pain levels seem to rise.
In addition, your knee pain may not be due to your knee arthritis at all. It could be due to a problem in your lower back. While you may or may not have pain with milder knee arthritis, a pinched nerve or other damage in the back can refer pain all the way down its nerve branch and into the knee. It could also be due to a loose knee ligament that simply needs to be stabilized.
Function is another problem following a knee replacement. Most patients believe they will be able to return to or even exceed their normal levels of activity. In reality, 19 out of 20 knee replacement patients never obtain the increase in function they expected. Another complication is for those younger patients (55 and under), 15 out of every 100 knee replacement patients will only get a maximum of five years out of their new knee (while the presurgery expectation is that their knee will last for at least 15 years). Younger patients are more active, creating more wear and tear and, therefore, faster breakdown of the device.
Additional risks following knee replacement include spinal fractures, hip fractures, heart attack, stroke, and blood clots, and much more, and the list keeps growing.
The upshot? We’re seeing an epidemic of knee replacements because we have a system that’s designed to push product and incentivize physicians to perform more and more procedures. Hence, it should be no surprise that this and other research studies show that there are way too many knee replacements happening. How can you avoid getting an invasive surgery you don’t need? Get an opinion from a doctor who doesn’t do knee replacements! If that physician still thinks you need one, then you probably really do need the surgery!

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
