Amniotic and Placental Injection Medicare Claims Clawbacks Begin

Credit: Shutterstock
It’s often said that the federal government is like a huge destroyer. It doesn’t turn quickly, but when it points its guns in your direction, you don’t want to be there. I’m sure that’s what thousands of clinics around the country that offered Amniotic and Placental “Medicare Covered” injections are thinking now. Why? The largest single Medicare contractor has announced clawbacks. Let’s dig in.
“Medicare Covered” Regenerative Medicine
Around 2019 we began to see clinics popping up that advertised that Medicare was now covering “stem cell” injections that were derived from Amnion and Placental tissue. It didn’t take a rocket scientist to figure out that this was a serious problem on two fronts. First, the research done by our lab and others showed that these products contained no living and functional stem cells. The second problem was that it is clear that even though some companies had been granted a Q-code for product reimbursement, the Medicare guidelines (LCDs) stated NO coverage. In Medicare land, that means that while you may fool some poor soul sitting in a room of cubicles to pay you, that money was coming back to the feds someday.
By the summer of 2021, we began to see a concerning signal that this Medicare Amniotic billing scam was blowing up. A legal site announced that the department of justice was beginning to send out Civil Investigative Demands (CIDs) to clinics that were billing and erroneously getting paid by Medicare. That coincided with my discussions with a Medicare fraud and abuse contractor who was already on to this scam.
What Is a Clawback?
Medicare is unique in that if it pays you in error, you are subject to a clawback. That means that they can send you a letter years later stating something like:
“Dear doctor,
We noted that we paid you $1,367,245.32 in error for the injection of an Amnion product (code Q1234) into knee joints and the spine. It turns out that those payments, upon further research, were in error. Please promptly repay that money in the next 90 days. If you dispute this, then we will see you in court. Just one little reminder, if you lose that court case and we believe that you knew that Amniotic injections weren’t covered, you may be sent to federal prison for a very long time. Thank you and have a nice day!”
Hence, there’s one rule in medicine, “Don’t screw with Medicare”!
The First Clawback Domino Falls
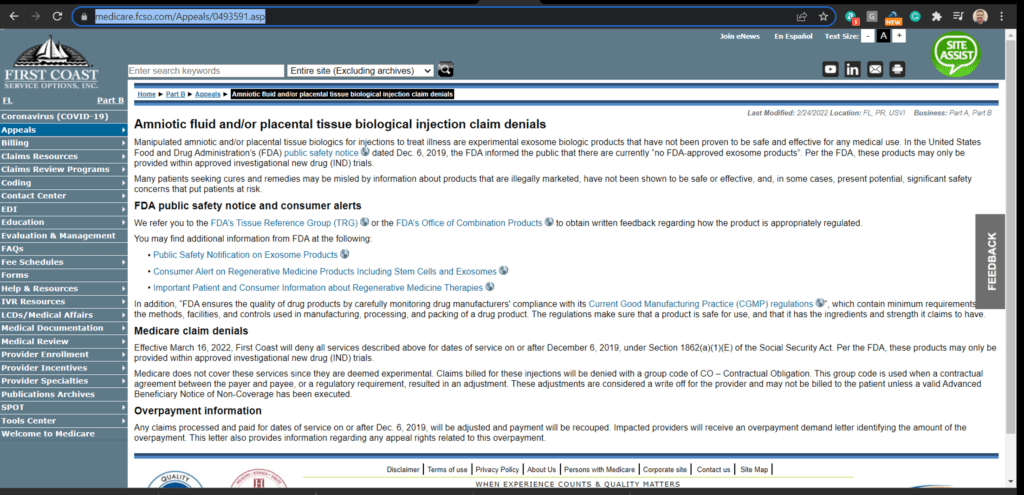
The highlights? Check this out:
“Medicare claim denials
Effective March 16, 2022, First Coast will deny all services described above for dates of service on or after December 6, 2019, under Section 1862(a)(1)(E) of the Social Security Act. Per the FDA, these products may only be provided within approved investigational new drug (IND) trials.
Medicare does not cover these services since they are deemed experimental. Claims billed for these injections will be denied with a group code of CO – Contractual Obligation. This group code is used when a contractual agreement between the payer and payee, or a regulatory requirement, resulted in an adjustment. These adjustments are considered a write off for the provider and may not be billed to the patient unless a valid Advanced Beneficiary Notice of Non-Coverage has been executed.”
Let’s unpack what this means:
- If you billed a Florida Medicare patient for an Amnio, Placental, or Exosome injection and got paid on or after December 6th, 2019, you owe that money back
- Medicare does not cover any birth tissue injection products
- You can’t bill the patient for the money that you pay back to Medicare (unless you had them sign an Advance Beneficiary Notice)
The Financial Impact of this Denial Notice
Given that the companies were selling these products in 2 cc vials for around $3,200-$4,000 and many clinics were billing and getting paid for multiple body parts, I would say the average amount per patient/per treatment owed back is around 8-10K. Let’s take the lower number and use the example of a clinic that was busy doing this:
- 3 patients a day or 15 a week-60/month
- December 6th, 2019 to Feb 6th 2022=26 months
- 60 x 26=1,560 procedures
- $8,000 x 1,560 procedures=12.48 million USD
As you can see, our hypothetical busy clinic now owes about 12 million USD to Medicare. In all practical reality, that means that this clinic is probably going to declare bankruptcy.
If the clinic only did 5 of these a month, 1.04 million USD owed back to Medicare. If you only ever injected one area (like only knees) and only did 1 a week, then you owe $332,800 back to Medicare.
Looking at these numbers, this will likely be the single biggest Medicare clawback in history.
Wait, the Company Gave Me a Reimbursement Guarantee!
I’ve seen Amniotic vendors use all sorts of “reimbursement guarantees”. Meaning that the companies either told the provider that they would give them free product or their money back if the product they bought got denied for payment by Medicare. However, you can easily see the problem here. These were mostly small fly-by-night vendors and not Merck or Pfizer. Hence in either scenario, the financial obligation of the company likely exceeds their annual revenue. Meaning I would expect that we will see many of these vendors skipping town with a burner phone about now.
As a Patient, Am I Now Liable for this Money?
It all depends on if you signed an advance beneficiary notice or an ABN. What’s that? An ABN must be signed by a Medicare beneficiary in order to bill that patient directly for services that aren’t covered by the program.
I would venture to guess that the smarter clinics probably slipped an ABN into the new patient paperwork for every new patient. Hence, if you signed that document, you are responsible for the full amount. How much? About $4,000 per body part injected. For example, if you had both knees and a shoulder, you owe the clinic around $12,000. In addition, don’t expect a payment plan as the doctor will probably have to pay this money back to Medicare in 90-120 days and your bank account is the mechanism to get that done.
What can you do to fight back if you suddenly owe $10,000 to the clinic down the street? I would recommend contacting your State Attorney General’s office. This is doubly true if you’re elderly, as the fact that you were misled by the clinic that this was a “stem cell” injection and was covered when there was ample evidence out there that it really wasn’t may qualify under specific fraud or elder abuse statutes.
The Bigger Problems for Providers and Companies
There’s an even bigger problem here. First, Florida is only 1/5th of the national Medicare market. That means the other Medicare contractors will now begin to fall like dominoes. I know that one midwest MAC is already in the process of doing the same thing. Given that reimbursement contractors get paid off a percentage of each Medicare dollar recovered, there are tens of millions to be made here by these companies. Meaning they aren’t going to leave a penny on the table uncollected.
The second problem is jail time. In big fraud takedowns like this one, which is likely one of the biggest in history, someone always has to go to prison. Hence, I expect that some of the CEOs, sales reps, and billing companies caught up in this massive fraud to be hauled in and charged. How many remains to be seen. However, you can bet that perp walks are coming.
What About Extradition?
In writing this article, I did a quick Google search of where a Medicare birth tissue scammer could flee that would be beyond the long arm of the US feds. While I expected to find all sorts of cool places that didn’t extradite back to the US, I was surprised that the list of countries wasn’t great. For example, Iran, and North Korea are on the list as well as Saudi Arabia. Now there is Viet Nam. I hear the condos on the beach there are quite lovely and all of that ill-gotten loot will go a very long way!
The upshot? The Medicare birth tissue house of cards has now officially fallen. If you billed this stuff to Medicare, you have two options: pay up or get out of dodge.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
