RIP Cervical Disc Replacement: Side Effects Same as Fusion
I’ll never forget when a local surgeon, who was being paid handsomely by disc replacement manufacturers, placed his new credo “friends don’t let friends fuse” on his website. The idea was that now that we had disc replacement technology, keeping some motion in the spine would reduce the side effects compared to fusion. For the last decade-plus, that’s been the big push for cervical disc replacement over fusion. I’ve even had new patients come into the office, very proud that they flew to Europe to get the latest state-of-the-art multilevel cervical disc replacement. What if this wasn’t true? If you were told that disc replacement was no better than fusion, would you still want a small hockey puck-sized device jammed in the front of your neck?
Rumruay/Shutterstock
Defining Cervical Disc Replacement and Cervical Fusion
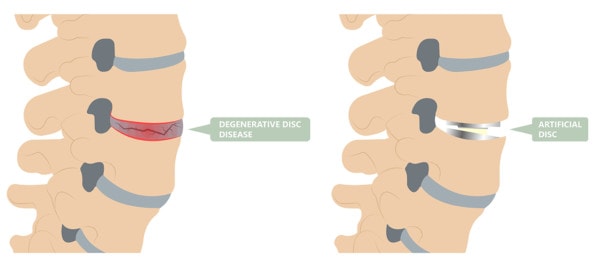
Cervical disc replacement involves removing the damaged disc, preparing the surfaces of the vertebrae, and installing a metal or plastic manufactured disc that, as mentioned, is shaped like a small hockey puck. With a cervical fusion, the damaged disc is also removed, but instead of replacing the disc, hardware is used to bolt the two (or more depending on how many levels are involved) vertebrae together. Within a few months, the vertebrae grow together, fusing into a solid mass of bone.
What sets cervical disc replacement apart from cervical fusion is that the disc replacement retains movement in the involved area of the neck while the fusion permanently and irreversibly disables movement. As a concept, disc replacement is supposed to be an alternative to fusion that will eliminate pain and won’t disrupt function, thereby lessening the risk of adjacent segment disease (ASD).
ASD is damage caused to the spinal segments both above and below the neck fusion, and this occurs when they become overloaded while trying to take on the extra forces the fused levels can no longer accomplish. Arthritis and bone spurs typically develop with ASD. As ASD advances, many patients will opt for more fusions in a desperate attempt to chase the damage and pain, but this will only make matters worse. Unfortunately, however, ASD doesn’t only occur following cervical fusion. Let me explain. To better understand ASD, see my video below:
Cervical Disc Replacement Side Effects and ASD
Cervical disc replacement certainly seems less extreme than a cervical fusion. It doesn’t eliminate movement. With the exception of the artificial disc device, no hardware (screws, rods, etc) is left attached to the spine. However, disc replacement is also a big surgery all on its own that’s associated with many side effects (e.g., metal ions in the blood due to wear and tear from the disc device, revision surgeries, chronic pain, etc.).
Last year I covered research that discovered another big problem in the list of cervical disc replacement side effects. Despite the push toward cervical disc replacement over cervical fusion due to fusion’s association with adjacent segment disease, ASD is also occurring is segments above and below disc replacements due to distorted movement in the spine. Why? Likely because an artificial disc simply can’t perfectly mimic the precise function of a normal biologic disc, so it’s understandable that abnormal motion in a segment of the spine is going to overwork adjoining segments that attempt to compensate.
Now, a new study seems to further support these findings on these specific cervical disc replacement side effects…
Cervical Disc Replacement Has the Same ASD Risk as Fusion
The new study was a meta-analysis, meaning many similar studies were aggregated to investigate like data, in this case the presence of ASD on radiology imaging following cervical disc replacement or fusion. After compiling all the data, researchers found no convincing evidence, based on radiology reports, that cervical disc replacement significantly decreased adjacent segment disease risk when compared to the fusion cases.
I can’t overstate the magnitude of this research finding! First, this is a meta-analysis that looked at data from many different studies, so this just isn’t just the finding of one study. Second, the main reason to get a disc replacement is that it’s motion preserving and that this is supposed to reduce the likelihood of ASD or eliminate it all together. In fact, if that’s true, I’m not sure why anyone would want a disc replacement.
The upshot? This meta-analysis should be the death knell for disc replacement. That’s because the only raison d’être for disc replacement was that it could reduce the ASD side effects compared to fusion. If it can’t do that, why would anyone want a disc replacement? Why is this still happening? A big neck surgery is a big neck surgery is a big neck surgery. They all end up destroying critical stabilizing structures in the neck.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
