Loose Hip Joint? It Could be Your Ligamentum Teres
Since we invented orthopedic stem cell injections at Regenexx, we still do a lot of inventing. Our physicians are constantly innovating so that we can replace invasive surgeries with precise injections. This morning I’d like to discuss how a precise X-ray guided injection of the ligamentum teres can help patients with a loose hip joint.
The Hip Joint and the Ligamentum Teres
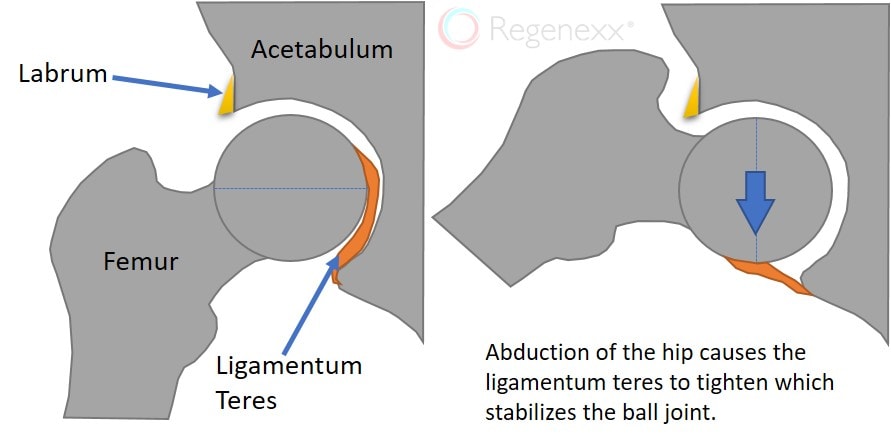
The hip joint consists of the femoral head (the proximal “ball” part of the femur) and the acetabulum (the “socket” part of the pelvis) as well as supporting structures, such as the labrum for guiding the joint and ligaments and muscles for stability and motion control. Any of these structures can become injured, but today we’re focusing on a specific ligament, the ligamentum teres, and how it can cause a loose hip joint.
The ligamentum teres lives deep inside the hip joint and connects the transverse ligament at the acetabulum to a notch in the femoral head, holding the ball in place in the socket. The ligament is really engaged when you lift your leg out and up, similar to what we see ballerinas do. Think of the ligament as a fail-safe that allows the hip to stay in the socket when the joint moves in certain ways.
If your hip pops or cracks, or even if it just feels loose, this could be due to a stretched or damaged ligamentum teres. When the ligament’s tension becomes loose, the ball lacks sufficient control and can wobble too much in the socket, especially with certain motions. This loose ligament may start out as a small problem, but over time it can create excessive wear and tear and break down the labrum, causing arthritis in the hip joint (something I call an arthritis-causing event, or ACE). It can also cause bone spurs, either a cam or a pincer lesion, which studies have shown typically form to try to protect the joint from additional damage. In severe cases of ligament laxity or damage, the hip can even become dislocated, with the ball popping out of the socket, requiring manipulation to reposition the joint in place. However, this is rare.
What Causes the Ligamentum Teres to Stretch?
While the hip is a deep ball-and-socket joint, some people are born with more-shallow hip sockets. This can cause stress on ligamentum teres as it has to work harder and constantly stretch farther to keep the ball in place within the socket. In addition, there are certain sports or activities, such as ballet, dance, figure skating, and martial arts. that require a large range of motion of the hip. Over time, this can stretch or tear the ligament. Hip arthroscopy surgery itself uses substantial traction to access the joint that can also severely and permanently stretch or injure the ligament as well as the muscles around the joint. Additionally, traumatic injuries can stretch or damage the ligamentum teres, and these injuries can go unnoticed for years until a loose hip joint becomes uncomfortable or begins to crack or pop.
Treatment for a Loose Hip Joint Caused by a Torn Ligamentum Teres
Surgery for a loose hip joint often focuses on ligamentum teres repair. While a damaged ligament can be helped with surgery; this is a massive procedure. This surgery involves either partially or fully dislocating the joint and then either stitching the torn ligament or reconstructing it with a graft. There is obviously massive downtime and all of the big risks associated with a big surgery.
There is another way to help the ligament heal in cases where the ligament isn’t torn and retracted (most tears). This is a fluoroscopy-based injection procedure that uses the patient’s stem cells to try and ramp up healing in the damaged structure. However, it’s critical to note that in our 12 years of injecting hips with stem cells, we have learned that unless this ligament is specifically targeted, it can’t be fixed. There are many clinics who are using blind injections without guidance who can’t replicate what you see here. It would also be almost impossible to replicate this procedure with ultrasound guidance because the ligament is buried deep in the joint. So if you were a master at ultrasound-guided injections, you might be able to catch one small part of the ligamentum teres, but you could never confirm that you injected the whole ligament as that can’t be seen using this type of technology.
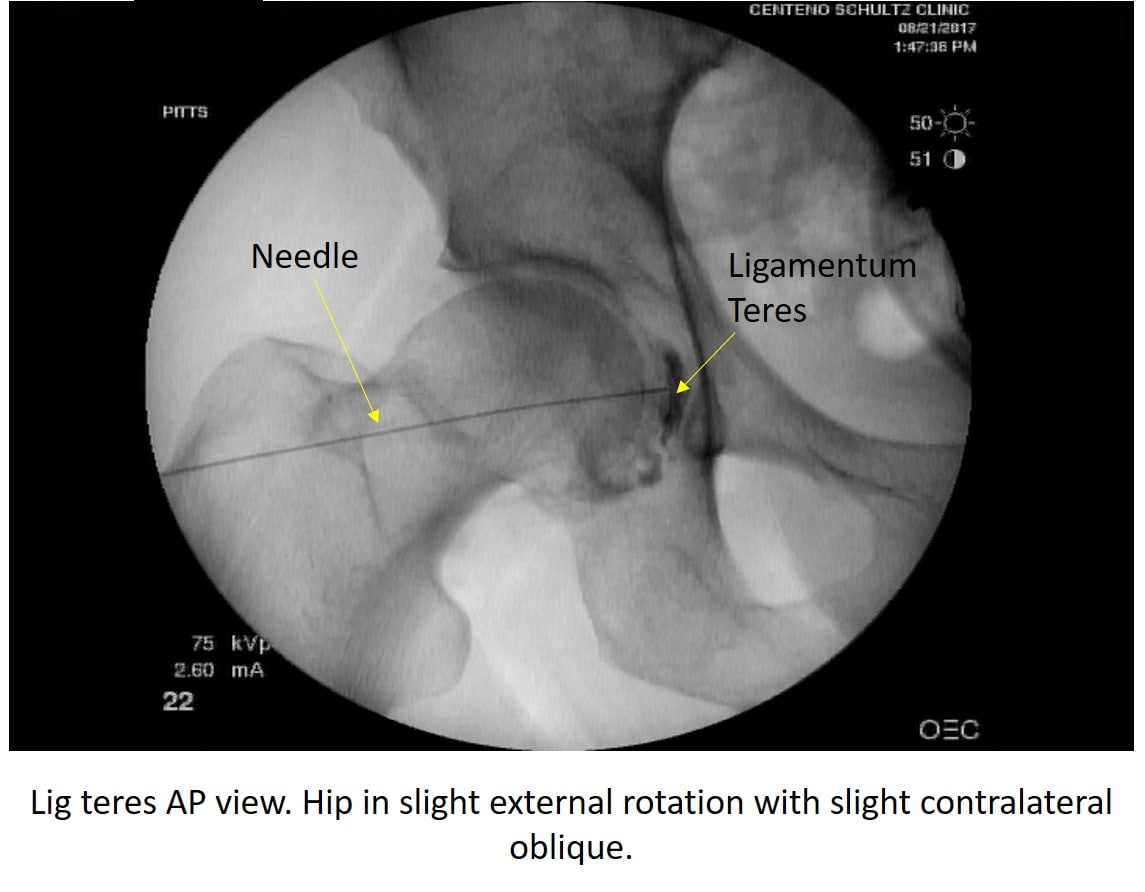
Real-time X-ray–guided injections (fluoroscopy) can target the damaged ligament with a precise injection, as shown below. This is a technique that was pioneered at our Colorado clinic last year and has evolved in accuracy since that time. In fact, I put together the first injection performed, which was interesting as there was no textbook to review. Since that time, Dr. Pitts and Dr. Markle have competed to produce better and better procedural variations. Below is a recent injection performed by Dr. Pitts:
The upshot? We continue to advance the high art of interventional orthopedics. The ligamentum teres procedure is a technically demanding and precise injection but one that can save many patients with a loose hip joint a massive surgery. We will continue to advance this field, and we look forward to sharing more breakthroughs and discoveries on the blog!

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.