Thumb Arthritis Surgery Recovery: What a Mess…
We can help the majority of patients with thumb arthritis without the need for invasive surgery. However, we also see some patients we can’t help. One such patient tried a platelet injection to avoid a protracted thumb arthritis surgery recovery and this didn’t help. So rather than moving on to the next step in our care paradigm which is stem cells, I told her I would look at the surgical options being offered to her and write a blog about her choices.
First, almost all patients I have ever met who are offered surgery believe that since surgery is commonly performed for things like arthritis that there must be great research showing it works. In fact, with almost all surgical procedures being offered for pain today, the exact opposite is often the truth-the research is often very poor and conflicted or in some cases shows the surgery is completely ineffective. A great example of the latter is knee surgery for arthritis or a meniscus tear-the surgery is still commonly being performed and patients believe it must therefore work, but the research shows it’s completely ineffective.
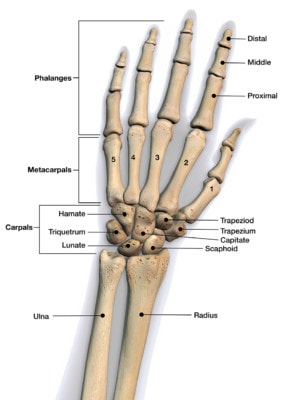
Bones of the hand and wrist. Hank Grebe/Shutterstock
Surgical options for thumb arthritis at the base of the thumb are pretty basic, although they sound quite complex. Basically, the most common surgery is removal of all or part of the wrist bone that makes up part of the base of thumb joint (trapeziectomy). Why would you surgically remove a wrist bone? The idea is that if the joint is painful, remove the joint. Since once you remove the joint between the base of the thumb and wrist the area will collapse under the pressure of the thumb, one option is to take a tendon from the hand and coil it up and stuff it into this space (tendon interposition). This sounds like a good idea, but a recent research review has shown that this is associated with double the side effects. In order to get around this, my patient was offered a “TightRope Suspensionplasty”. This basically means that a rubber band like device will be drilled into the bone of the thumb and adjoining structures to keep the area at the base of thumb from collapsing. So in summary, she has three traditional surgical options-remove the joint, removal plus stuffing a tendon into the void, or removal plus a rubber band doohickey.
So do we have any high level evidence that any of these invasive surgeries works well in most patients? In short-NO. The best document to date on this was written by an International research organization called the Cochrane Group. While we have some higher level studies on the seven different surgical options and procedural flavors, these are all very small studies. So the big study performed at many sites with a rigorous design for any one of them doesn’t exist. However, if we look at these small studies, what do we know?
Patients often believe that since surgery is often placed at the end of the clinical decision tree after more conservative things like drugs or physical therapy, that it must be definitive. Here this would mean that after the surgery, it’s highly likely that all thumb pain will go away and all normal hand function will return. Regrettably the little research we have on these surgeries for thumb arthritis don’t show that level of recovery. On average, after the surgery, patients still have mild to mild-moderate pain. Perhaps more concerning is that patients also continue to report mild to moderate loss of hand function. In addition, for the more common surgery of joint removal plus tendon insertion (trapeziectomy and tendon interposition), the complication rate is sky high at 22%! What do we know about the new surgery with the rubber band doohickey? It’s very experimental, with only one lower level study of 11 patients that I could find. Meaning, we know very little about it’s efficacy or it’s safety.
The upshot? Hand surgery research to treat thumb arthritis is a mess. Like most other surgeries to treat pain, we don’t have good evidence that it works. We have even less evidence that a rubber band doohickey will make the surgical results any better. What’s concerning is that the existing research shows that most patients still have hand function problems after a surgery that in one iteration, has a 22% complication rate!

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
