Understanding what Happens when a Torn Knee Meniscus Displaces
©Regenexx
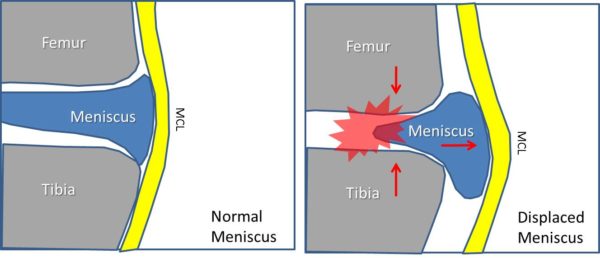
The knee has a shock absorber called the meniscus. When this structure is torn, it can often be operated using knee arthroscopy. In this surgery, many times parts of the meniscus are cut out. When this happens or when the meniscus gets smaller due to wear and tear, the knee meniscus displaces outside the joint (called displaced on an MRI report), robbing the knee of this valuable shock absorber and causing more trauma to the joint surfaces. In the pictures above, the left shows a normal knee. This is a cross section (front view) where the meniscus is acting as a spacer between the tibia and the femur bone. The yellow MCL (medial collateral ligament) acts like duct tape on the side of the knee, holding things together. Now look at the right picture. Here part of the meniscus has been surgically removed and the now much smaller meniscus is being spit out the side of the knee joint. In this case, the meniscus can no longer act as a shock absorber and the two joint surfaces now can easily crash together with every step. This loss of the meniscus as a spacer and shock absorber soon leads to more arthritis in this part of the knee. Also note that the MCL ligament is bowed out by the meniscus.
Now take a look at the picture above. It’s been turned 90 degrees so that now the MCL ligament on the side of the knee is facing up. This is what an image would look like if the patient was lying on his or her side. Again the meniscus is slipping outside of the joint because its just too small to act as a shock absorber.
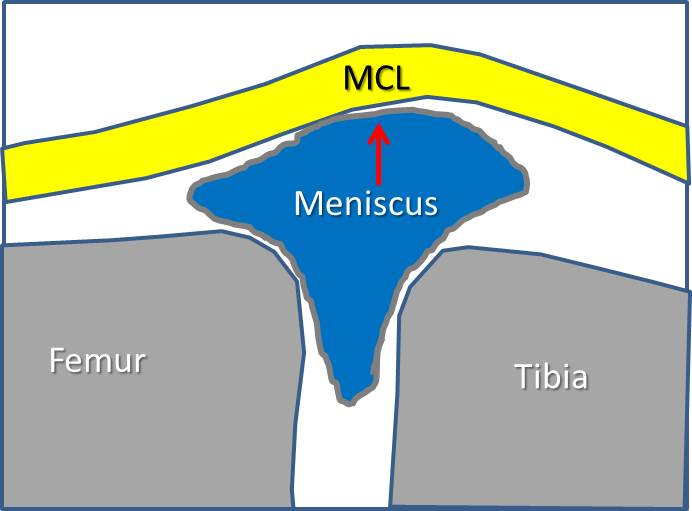
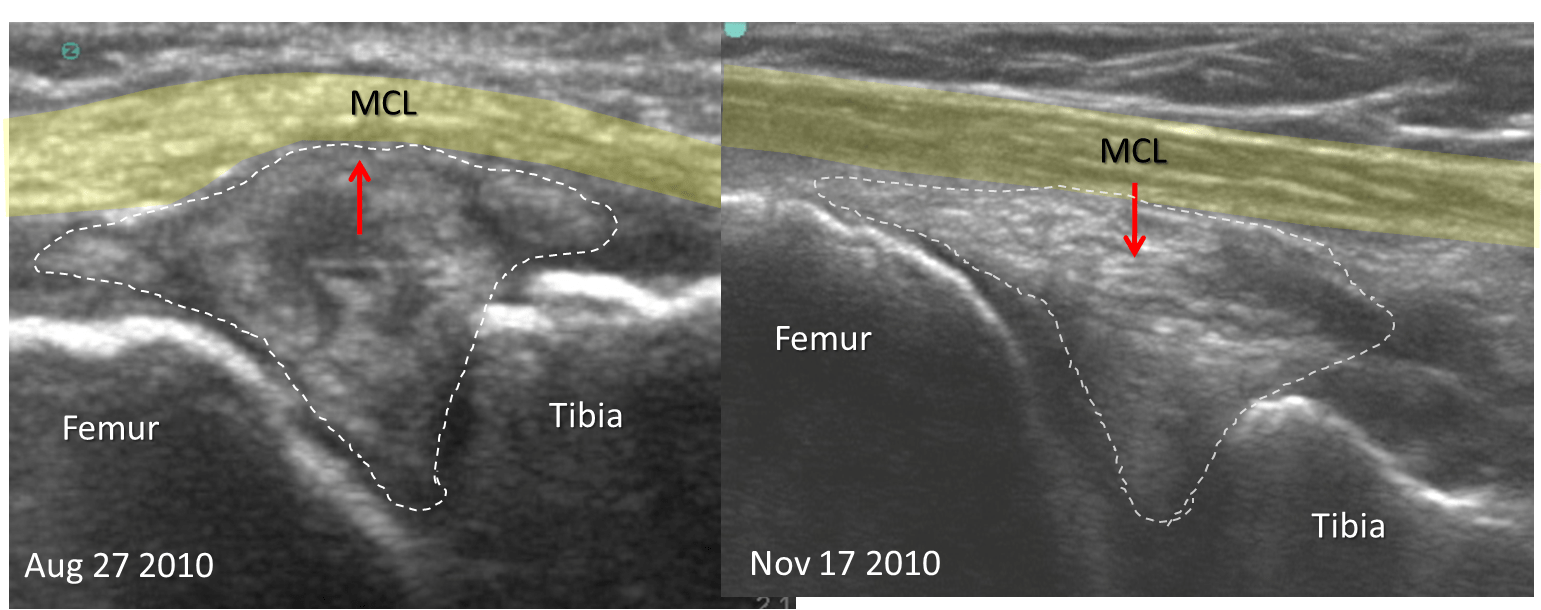
Now for the hard part. Ultrasound is one way of imaging the knee. Above you see two ultrasound images, one taken before treatment on the left and one on the right two months into treatment. You see all the same structures that I’ve outlined above (meniscus now inside the dashed line). Note that in the before treatment image on the left, the patient has a small meniscus being spit out of the joint. The MCL (in yellow) is bowed and inside the dashed line there are multiple dark areas (on an ultrasound of the meniscus, dark=torn). The patient was told she would likely need a knee replacement on this side, but instead opted for the Regenexx-SCP and Regenexx-PL procedures (no bone marrow draw or adipose collection, simply an IV blood draw). Here the patient recieved a stem cell plasma and platelet lysate injection under ultrasound to exactly place cells into this torn, damaged, and displaced meniscus. This was not just a blind injection into the knee, but the use of imaging guidance by a highly skilled clinic physician (Ron Hanson, M.D.). The cells were placed directly into these tears and into the loose MCL ligament with millimeter precision. There was no surgery and since this was an injection, recovery was much quicker than arthroscopy. The right image tells the story. We now see much fewer dark areas in the meniscus (inside the dashed line) and the MCL ligament (yellow) is no longer bowed by a meniscus which is being spit outside the joint. Here’s what the patient said:
I wanted to comment on the injections I received in both my right and left knees at the Centeno Schultz Clinic in Broomfield from Dr. Ron Hanson. I had a torn lateral meniscus in my left knee. Upon an MRI, it was discovered that the meniscus in my right knee had some problems as well. I had three injections in both knees. My left knee was in bad shape and terribly painful. I’m very active so wanted it repaired without surgery. Two years ago I had arthroscopic surgery on the left meniscus and shortly after, it tore again. Upon receiving 3 stem cell injections, (the stem cells extracted from my blood platelets), my right knee is 100 % and my left knee is close.
In summary, this is an example of what accurate placement of stem cells in a knee can do. It specifically doesn’t mean that every patient will get this result. However, this is a patient that had failed surgery and was in severe pain, now improved because of an innovative injection technique that can be performed without the need for surgery.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.