A Shoulder Stem Cell Procedure 6 Year Follow-up
One of the benefits of being the first physician in the U.S. to use stem cell injections to help orthopedic patients is that every once in a while, an old patient will come back. While we track everyone in a registry, it’s not the same as a patient sitting in front of you telling you how the procedure changed his or her life. Adriana is a dentist from California who just returned to get her knees treated after a successful shoulder stem cell procedure for her rotator cuff tear in 2010. Let’s review what happened with that shoulder.
Shoulder Rotator Cuff 101
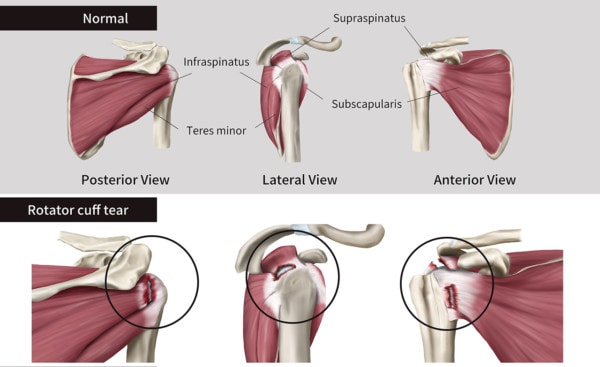
Chu KyungMin/Shutterstock
The shoulder rotator cuff is a collection of muscles that help stabilize the shallow socket of shoulder joint. They can be torn through trauma or sometimes just through degenerative wear and tear. While physical therapy is often recommended for partial tears, patients with a complete tear of one or more of the muscles usually end up in surgery. That procedure focuses on sewing back together the torn parts. However, the results from surgery aren’t fantastic:
- In patients over 60, about one in three rotator cuff surgical repairs fail.
- In one study, this shoulder surgery didn’t beat the results of physical therapy.
- Lost range of motion isn’t fully restored by rotator cuff repair.
In addition, strangely enough, the shoulder rotator cuff surgery results the patient reports don’t have anything to do with whether the shoulder heals on a subsequent MRI, which begs the question, why are we sewing the torn bits together? In addition, the pain the patient feels is much more related to the local levels of nasty inflammatory chemicals than it is to the size of the rotator cuff tear.
Adriana’s Story
Back in late 2010, I evaluated Adriana at our Colorado clinic. She was miserable. She had injured her left shoulder and knew things were bad because the pain was waking her up at night. In addition, at a recent wedding, she wasn’t even able to zip up her own dress. She was a dentist who used that hand all day to hold mirrors and other things, which meant keeping the shoulder in a raised position. Her MRI showed a complete rotator cuff tear, but, thankfully, it wasn’t retracted (meaning it wasn’t pulled back like a snapped rubber band). Most patients with complete tears don’t know which type they have—retracted or not—and this is often not discussed in the radiologist’s report. In November 2010, I injected Adriana’s own stem cells precisely into the rotator cuff tear using imaging guidance in a same-day procedure.
So how did she do? She reports today that after some initial soreness, the shoulder was 100%. She returned to full range of motion without pain and could work all day without discomfort. Zipping dresses? No problem! In fact, this shoulder stem cell procedure lasted for almost six years with just a little bit of return of soreness this past few weeks. Her ultrasound yesterday showed just a small partial-thickness degenerative tear in the infraspinatus. What happened to the full-thickness tear? Not seen on ultrasound yesterday.
The upshot? Since we’ve been injecting stem cells so long, we have the longest experience in how patients fare. So it’s not unusual for us to see patients back 4, 5, 6, or even 10 years later who are still doing quite well. In this case, a very grateful dentist who dodged the surgery bullet with a shoulder stem cell procedure!

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
