Understanding Platelet-Rich Plasma (PRP)

Medically Reviewed By:
For individuals experiencing joint pain or injury, surgery is not always the preferred option. Many seek non-surgical alternatives that support the body’s natural healing abilities and improve function. One such option is platelet-rich plasma (PRP), which has been widely studied for its role in orthobiologic applications.
Physicians in the licensed Regenexx network use PRP injectates processed with proprietary Regenexx lab methods to deliver a more precise and customized approach. This method is informed by extensive laboratory data and clinical insights, optimizing the concentration and composition of platelets to enhance treatment specificity.
What Are PRP Injections?
PRP refers to a concentrated mixture of platelets derived from a patient’s own blood. To create PRP, a small blood sample is drawn and processed using a centrifuge to separate and concentrate the platelets.
PRP injectates prepared using Regenexx lab processes are customized to optimize platelet composition and concentration, supporting the body’s natural healing abilities.
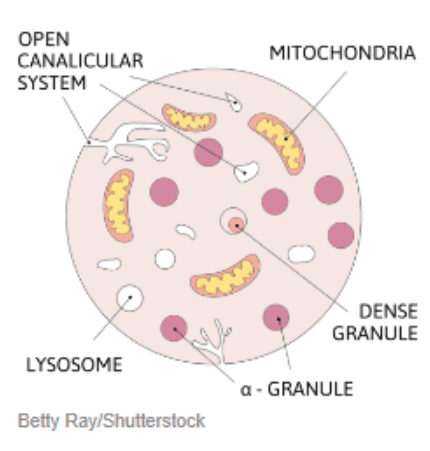
Platelets play a natural role in the body by helping blood clot and releasing growth factors—proteins that support tissue repair. These growth factors trigger the body’s natural healing response when an injury occurs.
Physicians in the licensed Regenexx network process PRP injectates using proprietary lab methods to optimize platelet concentration and composition for precise application.
PRP falls into different categories based on its cellular composition. Leukocyte-rich (LR) PRP contains higher amounts of white and red blood cells, giving it a reddish hue. In contrast, leukocyte-poor (LP) PRP has fewer white and red blood cells and appears amber in color.
In the U.S., most PRP comes from automated bedside machines, while more refined lab-processed PRP is more common in other regions. The centrifugation process separates blood into layers, and adjusting the spin intensity determines platelet concentration, allowing clinicians to customize PRP formulations based on patient needs.
Platelets release growth factors that signal local repair cells to respond and attract additional cells to the injured area. These growth factors are stored in alpha granules within the platelets and are released as needed to support the body’s natural healing response.
Is PRP A Stem Cell Therapy?
No, PRP is not a stem cell therapy. Blood contains very few circulating stem cells. Since PRP comes from a patient’s blood, it has only a minimal number of these cells. While PRP may contain some mesenchymal stem cells (MSCs), bone marrow holds a significantly higher concentration.
Most stem cells in the bloodstream originate from the bone marrow. In specific cases, clinicians may use medications to prompt the release of stem cells from the bone marrow into the bloodstream, where a process called apheresis can concentrate them.
Different Types Of PRP
Physicians commonly use two main types of PRP injectates:
- Leukocyte-rich PRP (LR-PRP): This PRP has a reddish hue and contains higher amounts of white and red blood cells.
- Leukocyte-poor PRP (LP-PRP): This PRP appears amber and has lower levels of white and red blood cells.
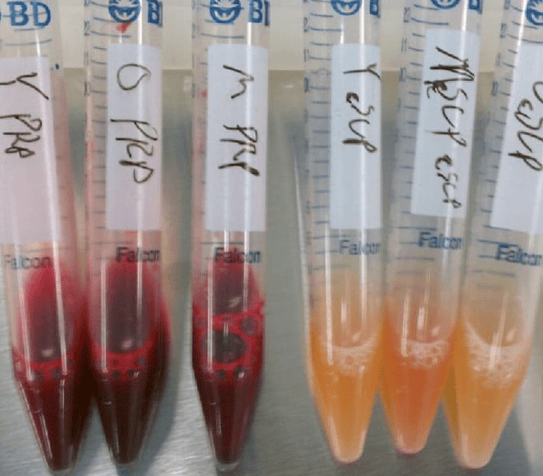
The red vial on the left contains leukocyte-rich PRP (LR-PRP), while the amber vial on the right holds leukocyte-poor PRP (LP-PRP). Both preparations have a high concentration of platelets, but LR-PRP contains more red and white blood cells, giving it a reddish hue.
Researchers continue to study potential clinical differences between these PRP types, and physicians actively discuss the topic in medical conferences.
For example, studies suggest that LR-PRP may damage synovial cells in the knee more than LP-PRP. Research also indicates that LP-PRP may better stimulate cartilage cells and provide more favorable effects for patients with knee arthritis. Additionally, removing white blood cells from PRP does not appear to reduce its ability to support the body’s natural healing response.
However, some laboratory studies suggest that LR-PRP may perform better than LP-PRP in cartilage repair. Another study found that both LR-PRP and LP-PRP support the growth of ligament cells from the ACL.
Are There Platelet Concentration Differences in PRP?
The concentration of platelets in PRP plays a crucial role. Low concentrations typically range from 1 to 3 times the natural platelet levels in blood, medium concentrations range from 3 to 7 times, and high concentrations fall between 7 and 20 times. Studies show that PRP’s ability to support cell growth varies significantly based on these concentrations.
For example, platelet concentration has less impact on younger tendon cells but plays a key role in supporting growth in older cells. As a result, physicians often use higher PRP concentrations for middle-aged and older individuals.
Common Conditions Treated With PRP Therapy
Physicians in the licensed Regenexx network use PRP injectates in various orthopedic applications that support the body’s natural healing response. Below are some of the most common conditions where PRP injectates are applied:
- Anterior Cruciate Ligament (ACL) Tears: An ACL tear is a partial or complete rupture of the anterior cruciate ligament in the knee, often caused by sudden twists or high-impact movements. It may lead to pain, swelling, instability, difficulty bearing weight, or changing direction. Read More About ACL Tears.
- Knee Osteoarthritis: Knee osteoarthritis occurs when the cartilage in the knee joint wears down over time, leading to pain, stiffness, swelling, and reduced mobility. Symptoms may worsen with activity, potentially affecting daily movements such as walking or climbing stairs. Read More About Knee Osteoarthritis.
- Annular Tears: An annular tear is a small rupture in the outer layer of a spinal disc, which may cause localized back pain or nerve irritation. Symptoms can vary, with some tears leading to radiating pain, numbness, or weakness if the disc presses on nearby nerves. Read More About Annular Tears.
- Herniated Discs: A herniated disc occurs when the soft inner portion of a spinal disc pushes through its outer layer, potentially compressing nearby nerves. Depending on the affected area, this may cause pain, numbness, tingling, or weakness in the back, neck, or limbs. Read More About Herniated Discs.
- Slipping Rib Syndrome: Slipping rib syndrome occurs when the lower ribs move excessively due to weakened or loose ligaments, leading to pain, tenderness, and a popping sensation in the chest or upper abdomen. Symptoms may worsen with certain movements or deep breathing. Read More About Slipping Rib Syndrome.
- Sacroiliac Joint Dysfunction: The sacroiliac (SI) joint connects the spine to the pelvis and helps transfer weight between the upper body and legs. Dysfunction or inflammation in this joint may cause lower back pain, hip discomfort, and stiffness, often worsening with movement or prolonged sitting. Read More About Sacroiliac Joint Dysfunction.
- Spondylolysis: The sacroiliac (SI) joint connects the spine to the pelvis and helps transfer weight between the upper body and legs. Dysfunction or inflammation in this joint may cause lower back pain, hip discomfort, and stiffness, often worsening with movement or prolonged sitting. Read More About Spondylolysis.
- TMJ Syndrome: TMJ syndrome, or temporomandibular joint disorder, occurs when dysfunction in the jaw joint causes pain, stiffness, clicking, or difficulty chewing. Symptoms may also include headaches, ear pain, or jaw locking, often worsening with jaw movement or stress. Read More About TMJ Syndrome.
- Shoulder Osteoarthritis: Shoulder osteoarthritis occurs when the cartilage in the shoulder joint wears down over time, leading to pain, stiffness, swelling, and reduced range of motion. Symptoms may worsen with movement, potentially affecting daily activities and arm function. Read More About Shoulder Osteoarthritis.
- Hip Osteoarthritis: Hip osteoarthritis occurs when the cartilage in the hip joint gradually wears down, leading to pain, stiffness, and reduced range of motion. Symptoms may worsen with movement or weight-bearing activities, potentially affecting mobility and daily function. Read More About Hip Osteoarthritis.
- Osteitis Pubis: Osteitis pubis is an inflammation of the pubic symphysis, the joint at the front of the pelvis. It may cause groin pain, stiffness, and difficulty with activities such as walking, running, or changing direction, often worsening with repetitive movements. Read More About Osteitis Pubis.
- Plantar Fasciitis: Plantar fasciitis is a common cause of heel pain, resulting from inflammation of the plantar fascia, the ligament that supports the foot arch. It often causes sharp pain, especially in the morning or after long rest periods. Proper treatment can help improve mobility. Read More About Plantar Fasciitis.
- Thumb Arthritis: Thumb arthritis, or basal joint arthritis, occurs when the cartilage in the thumb’s base joint wears down, leading to pain, stiffness, and reduced grip strength. Symptoms may worsen with pinching or grasping movements, affecting daily activities. Read More About Thumb Arthritis.
- Carpal Tunnel Syndrome: Carpal tunnel syndrome is caused by compression of the median nerve in the wrist, leading to numbness, tingling, weakness, or pain in the hand and fingers. Symptoms may worsen over time, affecting grip strength and fine motor skills. Read More About Carpal Tunnel Syndrome.
- Lateral Epicondylitis: Lateral epicondylitis, commonly known as tennis elbow, is a condition caused by overuse of the forearm muscles, leading to tendon irritation on the outer elbow. It may result in pain, weakness, and reduced grip strength, often worsening with repetitive arm movements. Read More About Lateral Epicondylitis.
What Makes The Regenexx-SCP Injectate Used in PRP Therapy Unique?
The Regenexx-SCP injectate is a specialized form of platelet-rich plasma (PRP) designed to optimize growth factor concentration. Regenexx lab processes can produce injectates with up to 20 times the growth factor levels found in typical PRP preparations, exceeding the concentrations achieved through standard bedside processing.
Physicians in the licensed Regenexx network may recommend SCP injectates for middle-aged and older individuals or based on the severity of a condition. This approach allows for a more tailored formulation to support the body’s natural healing response.
Regenexx-SCP injectates differ from typical PRP formulations available at many clinics. Regenexx research indicates that higher platelet concentrations may better support the body’s natural healing response, particularly in older individuals. As a result, physicians may recommend SCP injectates for those who could benefit from a more concentrated formulation.
Support Recovery With The Regenexx Approach
The Regenexx approach offers a non-surgical option designed to support the body’s natural healing response and promote function. Regenexx-SCP injectates—a highly concentrated form of PRP—are processed using proprietary lab methods to optimize platelet concentration based on individual needs.
Physicians in the licensed Regenexx network may recommend this approach for joint discomfort, tendon injuries, or arthritis to help maintain long-term joint and tissue health.
Frequently Asked Questions (FAQs)
When considering the Regenexx approach, individuals often have questions about how it supports the body’s natural healing response and how it differs from traditional options. Understanding these details can help people make informed decisions about their orthopedic care. Below are answers to common questions to provide clarity and guidance.
How Long Does It Take For A PRP Therapy To Work? How Long Does it Take to Recover From Platelet-Rich Plasma?
The timeframe for improvement after a PRP injectate varies depending on the condition being addressed. For example, in mild knee arthritis, individuals may experience an initial inflammatory response lasting a few days to a week, followed by gradual improvement over several weeks to a few months.
Joint-related applications may show quicker results, while tendon and ligament issues often take longer. In these cases, most individuals report improvement within two to four months. For instance, a study on tennis elbow found that more individuals noticed improvement at six months compared to three months.
Watch this video for more details on why tendon and ligament applications may take longer to show improvement.
How Much Does Platelet-Rich Plasma Therapy Cost? Is PRP Covered by Insurance?
Most health insurance plans do not cover PRP injectates, except for employers or groups that offer Regenexx Benefits. Some workers’ compensation or auto accident insurance policies may provide coverage in specific cases.
For individuals paying out of pocket, the cost typically ranges from $1,000 to $2,000 for a single joint application. Treating multiple areas may increase the total cost.
Is PRP Treatment Permanent?
For degenerative conditions like arthritis, which naturally progress over time, PRP injectates are unlikely to provide permanent effects. In cases of mild arthritis, individuals may experience improvement for one to two years, while more advanced arthritis may see relief lasting six months to a year.
For partial tendon or ligament injuries, PRP injectates may support the body’s natural healing response, potentially leading to longer-term improvements. However, outcomes vary based on the severity of the condition and individual factors.
Is PRP Better Than Stem Cells?
PRP injectates and bone marrow concentrate (BMC) serve distinct roles in supporting the body’s natural healing response. PRP injectates, processed using proprietary Regenexx lab methods, provide growth factors that help local repair cells function.
BMC, processed through patented Regenexx protocols, contains stem cells that help coordinate the body’s repair mechanisms and support overall tissue health.
Physicians in the licensed Regenexx network often use PRP injectates for mild arthritis and partial ligament or tendon injuries. They may consider BMC injectates for more advanced arthritis or larger tendon injuries, where additional cellular support may be beneficial.
Because PRP and BMC injectates may be used for a variety of conditions, consulting a licensed Regenexx network physician is essential to determine the most appropriate approach for individual needs.
Consult a physician in the licensed Regenexx network to determine if the Regenexx approach is right for you.

Medically Reviewed By:
