A Lateral Collateral Ligament Tear: Listen To The Patient

I often write about what I experience in the clinic. Today I’d like to tell you about a patient who has a specific injury to his lateral collateral ligament but instead was told he needed the wrong surgery. How did that happen? The surgeon paid attention to the bright shiny object on the MRI. Let’s dig in.
The Bright Shiny Object Syndrome (BSO)
This syndrome occurs when medical providers focus more on an MRI report rather than listening to the patient. The physician who started modern medical education, Sir William Osler, once said (I’m paraphrasing), “If you listen to the patient, they’ll tell you the diagnosis”. BSO is the opposite, you look at the report and ignore the patient. Let’s get into Mike’s story.
Mike’s Injury
Mike is an avid hiker. He loves being in nature and conquering 3-4,000 vertical feet several times a week. However, a few months back he slipped on black ice on a rock and fell awkwardly on one leg. He felt immediate pain on the outside of his knee just above the fibula bone.
Mike was used to things getting better on their own, as every avid hiker gets banged up from time to time. However, when months passed and this pain didn’t improve, he got an MRI and saw an orthopedic surgeon. Since the MRI report showed a medial meniscus tear that was bigger than a small lateral meniscus tear, after a cursory exam the surgeon told him that he needed meniscus surgery to remove the torn pieces. However Mike was smart, he had no pain on the inside of his knee, so how could a tear in the inside meniscus need surgery? He politely declined and never went back.
Meniscus Tears as Common as Wrinkles
The problem with the orthopedic surgeon’s diagnosis was that it made no common sense nor scientific sense. Meaning that Mike is in his 70s. The research clearly shows that many people Mike’s age have meniscus tears on their MRI despite no knee pain at all (1). Hence, it was more likely than not that Mike’s meniscus tears on MRI had nothing to do with his pain. That was made certain when the MRI showed a much more significant MRI tear on the inside of Mike’s knee while his pain was ONLY on the outside of the knee.
The Lateral Collateral Ligament
The LCL is like a piece of duct tape that’s on the outside of the knee. In the picture here, it’s shown in light blue. It goes from the outside of the femur bone to the fibula (outside small lower leg bone) and it stabilizes the outside knee.
Getting to An Actual Diagnosis
Mike pointed to a specific spot on his knee, nowhere near his meniscus, but just above the fibula bone (small outside leg bone). Hence, after performing a comprehensive knee exam, I looked at that spot with ultrasound. This is what I found:
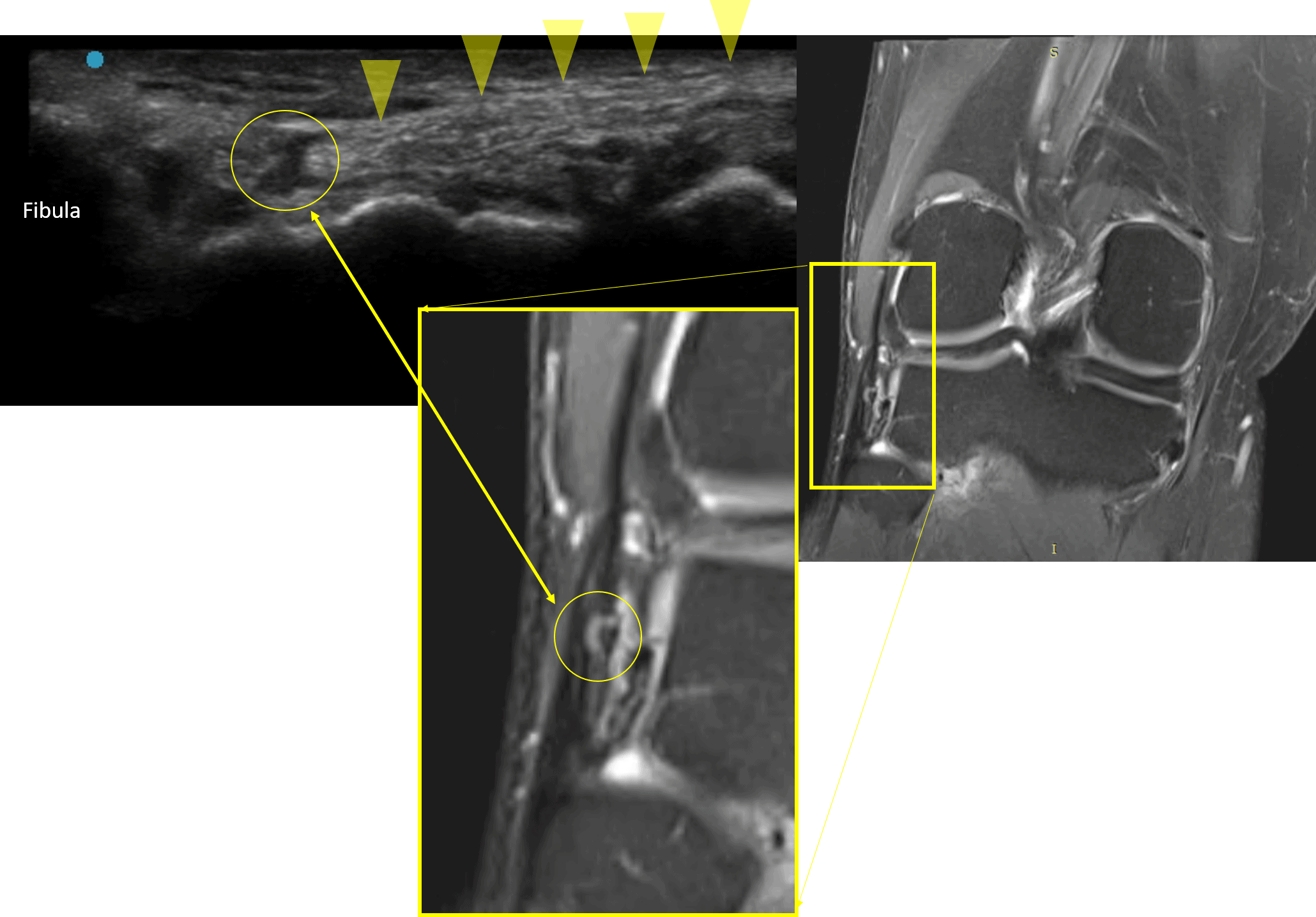
The ultrasound image above is of the lateral collateral ligament (LCL). The yellow triangle points to the healthy part of the ligament with fibers going right to left. The circle points to the exact spot where Mike has pain. This is a tear in the undersurface of the LCL which here is shown by the gap in the yellow circle. That was actually on his MRI, a finding which was missed by the reading radiologist.
How Can We Fix This?
Performing a meniscus surgery on this knee would be a disaster. This gentleman doesn’t need surgery. We will inject this area with high dose platelet-rich plasma (PRP). The goal is to prompt enough healing in this spot so he can continue to hike those great distances and elevation gains. We may or may not need to use bone marrow concentrate (a same-day stem cell injection procedure) at some point.
Because of Mike’s age, his tendon cells will need a much higher concentration of platelets than the simple bedside machines used by most doctors can muster. This is based on our published research looking at how older tendon cells respond to platelet dose (2). Hence, we’ll use our lab to create a very high-dose PRP which will hopefully stimulate his older tendon cells to mend the gap.
The upshot? Mike knew where his injury was located and thankfully he used his common sense to avoid a useless surgery. Now he’s hopefully well on his way to recovery because of one simple fact. Following in the steps of Sir William Osler, I listened to what Mike was saying. Mike was always willing to provide the diagnosis, all he needed was a good ultrasound and for someone to actually perform more than a cursory exam.
__________________________________
(1) Risberg MA. Degenerative meniscus tears should be looked upon as wrinkles with age–and should be treated accordingly. Br J Sports Med. 2014;48(9):741. doi:10.1136/bjsports-2014-093568
(2) Berger DR, Centeno CJ, Steinmetz NJ. Platelet lysates from aged donors promote human tenocyte proliferation and migration in a concentration-dependent manner. Bone Joint Res. 2019;8(1):32-40. Published 2019 Feb 2. doi:10.1302/2046-3758.81.BJR-2018-0164.R1

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.