What Are Important Back Pain Muscles?
If you or a loved one suffers from chronic low back pain and you’ve never heard of the multifidus muscle before, now’s the time to learn about one of the most important back pain muscles. This remarkably important muscle that stabilizes your spine, goes largely ignored by most doctors and surgeons. New research sheds even more light on just how this muscle goes about it’s business of protecting your back from catastrophic failure.
Why Is Spine Stability Important?
You have many muscles in your back. Most are there to hold you upright and to allow you to bend forward, to the side, rotate, or straighten up. Basically, most of them move the spine. But when your back “goes out”, it means that a different kind of stability muscle has failed to do it’s job.
Stability is a big deal in the spine. Think about it for a moment. Your back and neck are made up of a single column of vertebrae stacked like kids blocks, one on top of the other, 24 blocks high! Do you remember how hard it was to keep 10 or 15 blocks stacked without the whole thing crashing down, let alone 24?
To keep your vertebrae from falling apart, two systems are at play. One is passive and the other is active. The passive system which is made up of the ligaments, acts like duct tape to hold the blocks together. The active system is made up of stability muscles that keep the blocks aligned with micrometer precision as you move.
The stability muscles need to keep everything
The Multifidus Is the Major Spine Stability Player
Of all the spine stability muscles, the most important and best studied is the multifidus. This muscle lives at each level of the spine, stabilizing one vertebral block on another. While it’s very easy to observe this muscle on MRI scans as being smaller and weaker in patients with chronic low back pain, most radiologists and surgeons ignore it. Why? Certainly not because of the research, since there are tons of it showing that MRI evidence of atrophy of the muscle is bad news.
A new research study sheds some additional light on how the multifidus goes off line, and it turns out that all of this is pretty complex. The Canadian researchers looked at the muscle moving with ultrasound imaging and also measured brain activity with magnetic stimulation. What they found was that the maps of how we should activate various muscles that live in the brain for multifidus, were different for patients with chronic low back pain versus pain-free patients.
This is a really interesting finding, as most experts have believed that the loss of control of the multifidus muscles had more to do with irritated nerves or painful low back structures. Basically, a simple loop that when irritated or interfered with, shuts down the system. Now it appears the brain is also involved in why these muscles aren’t working.
The upshot? If you have chronic back pain and you’ve never before heard 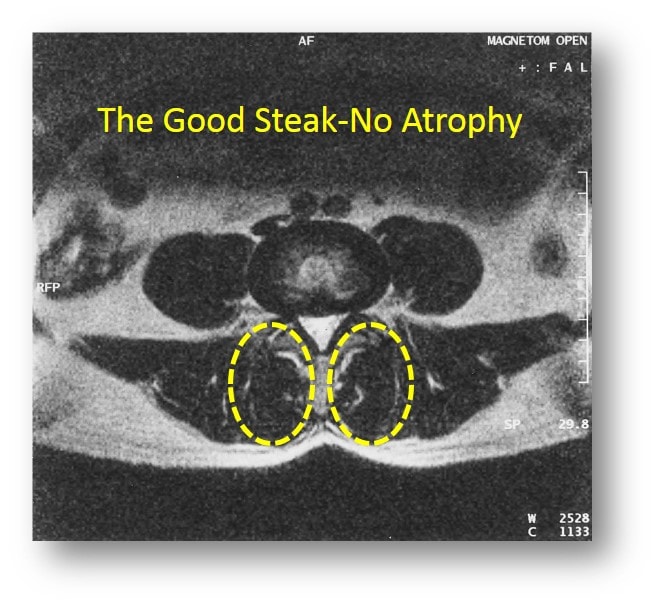
To read more about how that works, see our page on treating back pain with platelets and stem cells.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.