Do Shoulder Labral Tears Need Surgery?
Do shoulder labral tears need surgery? What happens if a labral tear goes untreated? Can you fix a labral tear through injections? Let’s dig in.
What is a Shoulder Labral Tear?
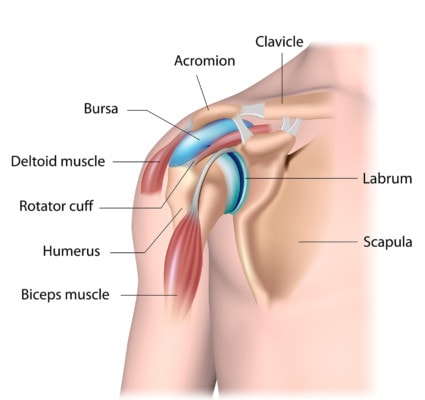
Shoulder joint structure labeled.
The labrum is the lip around the socket where the ball of the shoulder bone fits. It provides stability along with the shoulder ligaments and rotator cuff tendons. The primary cause of labral tears is shoulder instability (1). This is a critical concept that I’ll review later, as fixing the shoulder instability is critical in healing a labral tear.
The labrum can be torn or become degenerated (2). When the tear is in the upper part of the labrum, the area where the biceps tendon attaches to the lap of the socket is also commonly torn. When this happens, it’s called a SLAP lesion (Superior Labral Tear from Anterior to Posterior). When a shoulder dislocation occurs, the bone where the labrum attaches can also be associated with a small fracture of the bony lip of the socket, which is called a Bankart lesion. There can also be a small fracture on the head of the humerus and this is called a Hill-Sachs lesion.
Do Shoulder Labral Tears Need Surgery?
The most common type of shoulder labral tear is a SLAP lesion (type II). Is this surgery effective? There has only been one high-level study that compared surgical labral repair compared against a fake surgery. It did not show any difference in outcome between the labral repair surgery and the fake procedure (3). In another study looking at posterior shoulder instability, surgery edged out physical therapy, but the patients knew what procedure they were getting (unlike in the sham surgery study) (4). So do shoulder labral tears need surgery? We don’t have much solid evidence that a shoulder labral repair procedure works.
Labral Tears: Are They Really a Problem?
What if people without shoulder pain had labral tears on MRI? Given that’s how many patients are diagnosed and end up in surgery, how would that change things? In 2016, a study performed MRIs on patients without shoulder pain who were 45-60 years old, a staggering 55-72% of these people had labral tears (5)!
What Happens if a Labral Tear Goes Untreated?
The biggest issue is shoulder instability. What does that mean? The shoulder is a shallow socket with a ball that must be stabilized. When there is sloppy movement, which can cause the ball to bang into the labrum, as shown below:
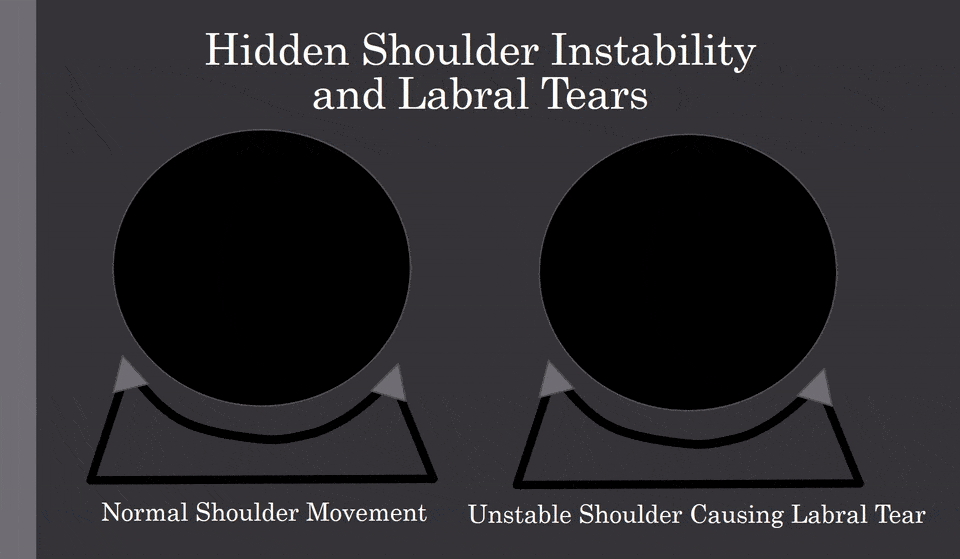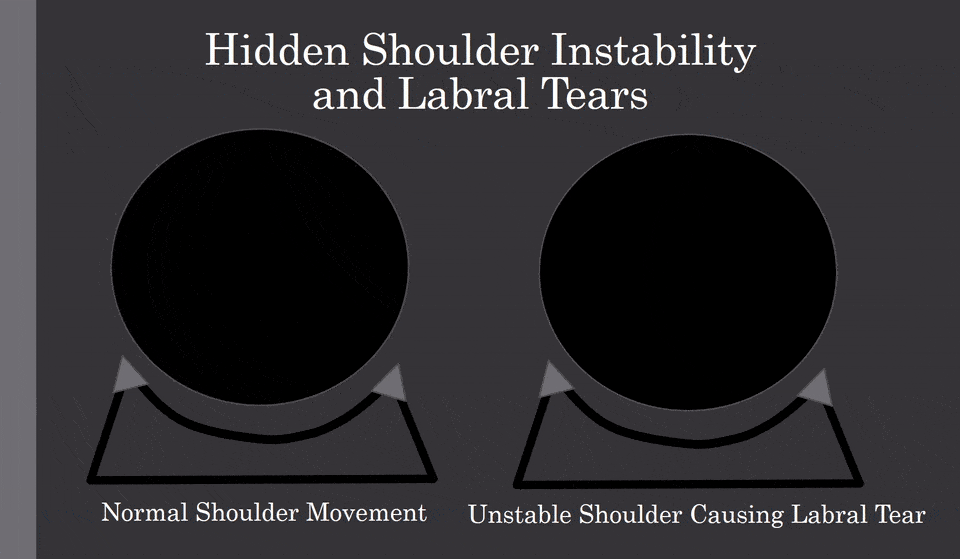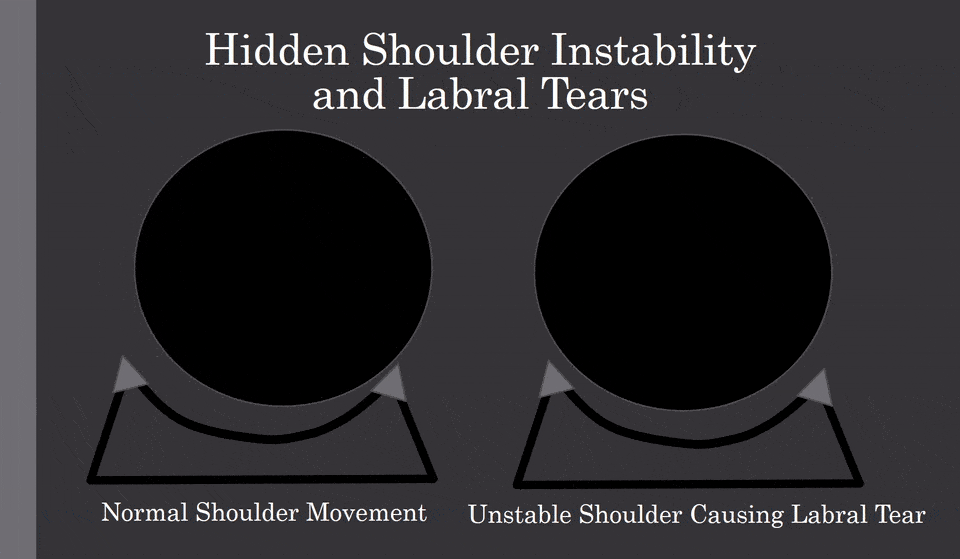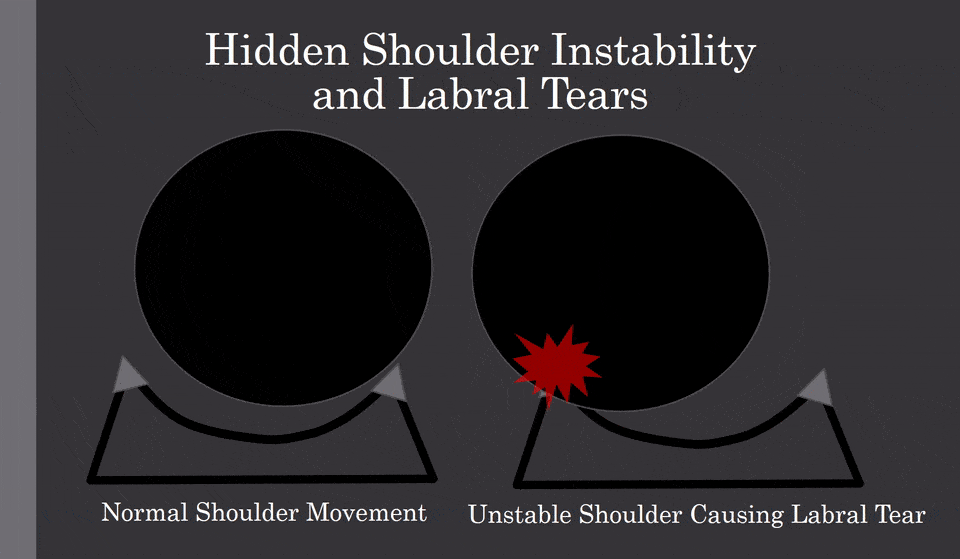
How can you improve instability?
- Build stronger rotator cuff muscles
- Tighten loose shoulder joint ligaments
Stronger rotator cuff muscles will help keep your labrum from getting reinjured, but sometimes the loose ligaments that allow too much motion will still need to be tightened.
Can You Fix a Labral Tear Through Injections?
Loose ligaments can be treated surgically either through suturing the folds of the capsule that surround the joint or by heating those tissues to get them to scar down (6). However, what would happen if you could skip the surgery and instead get an injection that would tighten these ligaments and prompt healing in the torn labrum? That procedure is called Percutaneous Shoulder Labroplasty (PSL). It uses orthobiologics (your own platelets or stem cells) and precisely injects them into lax ligaments and torn labral tissues using ultrasound guidance.
The upshot? The vast majority of shoulder labral tears do not need surgery. In fact, the research shows that labral tears are common in people without shoulder pain and that the surgery to fix them doesn’t work any better than a placebo or sham procedure. There are also newer treatments to consider that don’t involve surgery.
___________________________________________
References:
(1) Van Blarcum GS, Svoboda SJ. Glenohumeral Instability Related to Special Conditions: SLAP Tears, Pan-labral Tears, and Multidirectional Instability. Sports Med Arthrosc Rev. 2017 Sep;25(3):e12-e17. doi: 10.1097/JSA.0000000000000153.
(2) Clavert P. Glenoid labrum pathology. Orthop Traumatol Surg Res. 2015 Feb;101(1 Suppl):S19-24. doi: 10.1016/j.otsr.2014.06.028.
(3) Schrøder CP, Skare Ø, Reikerås O, Mowinckel P, Brox JI. Sham surgery versus labral repair or biceps tenodesis for type II SLAP lesions of the shoulder: a three-armed randomised clinical trial. Br J Sports Med. 2017;51(24):1759–1766. doi:10.1136/bjsports-2016-097098
(4) Cruz-Ferreira E, Abadie P, Godenèche A, Mansat P, Clavert P, Flurin P; French Arthroscopy Society. Posterior shoulder instability: Prospective non-randomised comparison of operative and non-operative treatment in 51 patients. Orthop Traumatol Surg Res. 2017 Dec;103(8S):S185-S188. doi: 10.1016/j.otsr.2017.08.004.
(5) Schwartzberg R, Reuss BL, Burkhart BG, Butterfield M, Wu JY, McLean KW. High Prevalence of Superior Labral Tears Diagnosed by MRI in Middle-Aged Patients With Asymptomatic Shoulders. Orthop J Sports Med. 2016;4(1):2325967115623212. Published 2016 Jan 5. doi:10.1177/2325967115623212
(6) Rolfes K. Arthroscopic treatment of shoulder instability: a systematic review of capsular plication versus thermal capsulorrhaphy. J Athl Train. 2015;50(1):105–109. doi:10.4085/1062-6050-49.3.63

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
