Looking for Safer Stenosis Back Surgery Recovery? Skip the Fusion!
Can a safer stenosis back surgery recovery can be had by skipping the fusion? When I began practicing medicine 25 years ago, a low back fusion was rare. However, over the last two decades low back fusion rates are exploding. Despite more widespread use, the practice is far more dangerous than the older style surgery it replaced.
Rumruay/Shutterstock
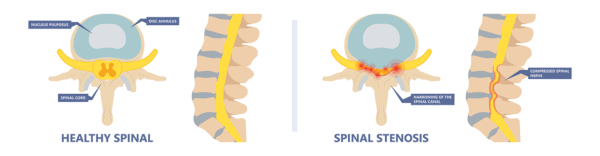
Spinal stenosis happens when bone spurs and arthritis crowd out the nerves and the spinal cord, putting pressure on these delicate structures. This can cause numbness, pain, weakness, and spasms. Many patients can be managed without any surgery. However, in the few that need surgery, the bone needs to be cut away from the nerves (hopefully as little as possible). This is called a decompression surgery. Surgeons over the last 10-20 years have added a new wrinkle; bolting the spine together with rods and screws to try and make sure the operated area doesn’t move too much. However, while the first method seems to work, does the bigger fusion surgery carry bigger risks?
A recent study in the European spine journal sought to answer that question. This spine surgery treatment registry looked at the results of more than a thousand surgeries. The less invasive, smaller decompression surgeries did pretty well with the larger surgeries not working as well. These smaller decompression surgeries produced about 60% fewer surgical complications and about 90% more general complications when a fusion procedure was added. In addition, there was a 70% lower chance of some medical intervention being needed as a result of the surgery if there was no fusion. The authors concluded that while fusion may work a bit better, it’s general use can’t be recommended due to the higher complication rates.
The upshot? If you have spinal stenosis causing pinched nerves, these days it’s highly likely you’ll be offered a fusion with the decompression surgery. Do your homework, skip the fusion! If it were my relative or my patient, I would always advise against fusion unless it’s absolutely necessary.

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
