Is Our Disc Fetish Hurting Regenerative Spine Care?
Modern spine care has a disc fetish. While the spine has many parts, surgeons and interventional-pain physicians seem to look at the disc as the cause of pain and trouble more than anywhere else. As a result, it’s become the defacto place to inject orthobiologics, like PRP and stem cells. However, does this view hurt patients? Where did this begin? How does regenerative medicine change things?
Where Our Disc Fetish Began…
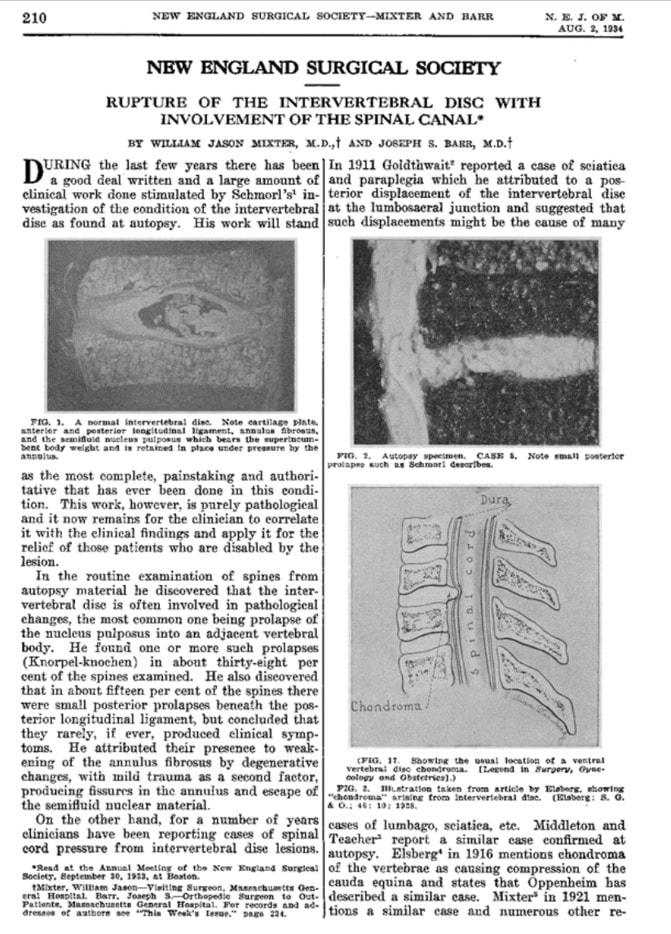
The year was 1934 when Mixter and Barr published a seminal paper on how a ruptured disc could cause nerve or spinal cord compression and pain. Around the same time, there was another technique focused on injecting ligaments. One of these concepts won the day as surgeries were invented to treat disc bulges that were compensable through newly popular health insurance. Below is the actual paper:
In the ’30s and ’40s, there were many competing theories for how the spine should be approached therapeutically. Mixter and Barr’s became the disc-surgery approach. George Hackett, a Midwest physician, focused on the injection of tendons and ligaments. James Cyriax of London took a similar, but unique hands-on exam approach, complaining that X-rays weren’t able to diagnose most of what was wrong with the spine. He and James Evans introduced the concept of caudal epidural injections to treat back pain. Cyriax also extensively injected muscles, tendons, and other areas. However, not all of these concepts survived as traditional medical approaches to see the ’50’s, ’60. and ’70s. Why?
With the advent of World War II came strict government controls on wages. This led to employers using health insurance as a way to compete for scarce US labor in factories ramped up to supply the war effort. This nascent form of health insurance and the large amounts that could be reimbursed for surgical care versus conservative care is one factor that helped establish disc surgery as the defacto standard. Another was that the 60s and 70s were dominated by surgical breakthroughs that came on the heels of surgical trauma care in the Korean and Vietnam wars. Hence, the disc became the center of our spine treatment universe based on many factors, only some of which had to do with the science of why patients have back and neck pain.
The Concept of the FSU
To understand why the disc shouldn’t be the center of our regenerative-medicine universe in 2017, you first need to learn about the FSU. Arguably, the father of modern spinal biomechanics is a Yale professor by the name of Manohar Panjabi. Dr. Panjbi published extensively on the concept of the functional spinal unit (FSU) throughout the ’80s and ’90s. The concept was simple: we have a disc, facet joints, and ligaments that all make up an FSU (the muscles were purposefully excluded because they couldn’t be modeled in cadaveric studies).
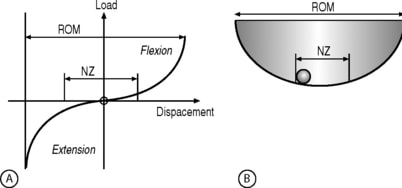
Panjabi put forth the idea of the “neutral zone.” This was the “happy place” of spinal stability where very little energy was needed to maintain that position. As a normal and healthy FSU is moved out of the neutral zone, more energy is needed to move the vertebrae, one on the other. Basically, the concept is best understood by a ball in a cup:
While diagram A will confuse you if you didn’t study engineering, B is more intuitive. A ball in a shallow cup has its “happy place” where not much energy is required to move it along the bottom of the container. This is the neutral zone, as a similar thing happens in the spine. Because of the constraints of the disc, shape of the facets, and nature of the ligaments, there is a small amount of movement in the middle of the normal range where the spine likes to live. Getting back to our example, you can also add energy to the ball and push it up the side of the cup. The same happens with spinal range of motion (ROM). You can bend the spine and stretch the ligaments and move the vertebrae out of their “happy place” by adding more energy. What does all of this have to do with our disc fetish?
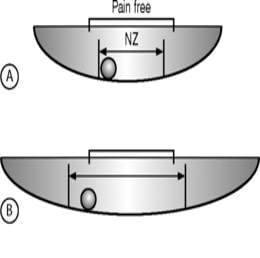
Remember that in Panjabi’s 1980s model, there is a disc, facet joints, and ligaments that all maintain the neutral zone. However, damage any one of these or all three, and the size of the neutral zone increases. Meaning the movement of the ball becomes sloppy:
Note that in B, our neutral zone has increased. Applying this to the spine, this sloppy range of motion will eventually lead to burnt out facet joints, stretched out ligaments, and a fried disc. In fact, still today, if you want to create a degenerative disc in an animal for research purposes, all you have to do is to injure the disc or facets or ligaments and one will form.
After Panjabi retired, a new element was added to the FSU—the muscles that stabilize and move the spine. This includes the all-important multifidus muscle. In addition, since a sprig of the spinal nerve innervates and tells the multifidus what to do, the spinal nerves become as important as an atrophied multifidus. For more info about the multifidus, see the video below:
How the FSU Relates to Regen Med
Right about now, you’re likely saying to yourself, “OK, dude, I appreciate the biomechanics lesson, but what does this have to do with stem cell therapy?” In fact, the FSU helps us pick our therapeutic targets. Let me explain.
To review, the four things that we know are responsible for maintaining spinal stability are: the disc, facets, ligaments, and multifidus muscle. Hence, at its simplest, all four are possible places where stem cells should be deployed. Why? Because restoring the normal FSU, or one that operates in the normal “neutral zone,” is what we should be trying to do, as this is what happens in a healthy spine.
Why would we become obsessed with the disc in this model? The disc is certainly an important player, especially when it has small problems, like tears and bulges, and if stem cells can heal those issues, we may help restore the FSU. This is likely why stem cell treatments and PRP injected into discs with good height and small tears seems to work well (ref 1, ref 2).
However, if the disc is collapsed, given that no stem cell therapy or biologic in 2017 will ever restore its normal height or biomechanical properties, then our priorities must shift to other parts of the FSU that may be helped: the facets, ligaments, and muscles. Hence, in a patient with degenerative disc disease where the discs have lost their height and are “bone on bone,” the disc is not the primary place to deploy stem cells if we want to help restore the FSU.
The Risks of the Disc
The disc is, by far, the riskiest of the common places to inject anything in the spine. That’s not to say that it shouldn’t be treated to maximize outcome in the right patients, but each disc injection should come with careful thought. Robert Heinlein once wrote that “War is the last resort of the incompetent.” Meaning that practically everything should be tried short of war. In the same way, given that a disc infection requires IV antibiotics and usually surgery, avoiding a disc injection unless there is a significant chance of helping the patient is wise.
The Other Regen Med Targets in the Spine
Given that the other parts of the FSU can also help to control spinal stability, it only makes common sense that if the disc can’t be salvaged, we turn our attention to these extradiscal areas. As we have demonstrated, regenerating the facet joints is possible (see video below). Tightening ligaments through injection was shown to be possible in our 2005 study. Finally, regenerating the multifidus may be feasible based on a recent study where PRP was injected.
How Pain-Generator Studies Throw Us off the Trail of Regenerative Spine
The spine literature is filled with what I call “pain generator” studies. When all we could do was inject anesthetic/steroid or burn the nerves that carried pain signals, knowing where the pain came from was important. Hence, these studies would generally inject noxious substances or use pressure into the part of the spine being tested to determine what percentage of patients reported pain. However, regenerative medicine allows us to begin restoring spinal function; hence, where the patient hurts is only part of the equation. Why the patient hurts (e.g., due to abnormal spinal stability eating away at structures, like the disc and facet) becomes critical. Hence, trying to hang our hat on these pain-generator studies from the ’90s throws us off the trail of what’s possible with regenerative spine care.
Hope for the Future
Obviously, we all want to be able to inject something into a severely degenerative “bone on bone” disc and grow a new one. In addition, this would help to restore the FSU. However, while this works well in rabbits, it doesn’t seem to happen when stem cells are injected into human discs. Nor does it happen on a long-term basis when we inject fibrin into discs. One day this will happen and we will be able to address the FSU in these patients who have lost disc height. However, all we can do for now in severe DDD patients is to address the other parts of the FSU.
The upshot? Understanding that regenerative medicine, when used properly in the spine, should move us away from our long-standing disc fetish and force us to focus on other parts of the FSU is critical. This is why physicians who are merely replacing what they used to inject with orthobiologics, like PRP and stem cells, and not rethinking where they inject are missing the proverbial boat. Regenerative spine injections, therefore, should target all parts of the spine that may help a patient, including irritated nerves, loose ligaments, arthritic facet joints, and atrophied muscles!

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.