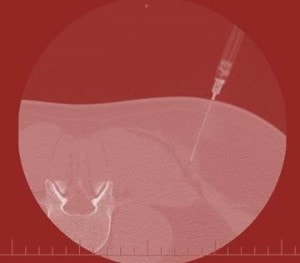
Never Use a Cannon to Kill a Fly: CT Guided Trigger Point Injection
Confucius said, “Never use a Cannon to Kill a Fly”…or…”Never do a CT guided trigger point injection.” Today’s picture above is an example of a physician who seems to have forgotten that maxim. There’s been much concern recently over the x-ray exposure caused by CT Scans. For example, new research shows that as many as 14,500 people a year may end up dying of radiation induced cancers caused by CT Scans. How much x-ray exposure are we talking? For the average CT Scan, likely about the equivalent of 100 chest x-rays. This brings up why we’re looking at this CT Scan above. I examined a new patient in the clinic this week for chronic low back pain who had had a bevy of procedures. He mentioned during his history that he had trigger point injections (TPI’s). This procedure is one where anesthetic is injected into an area of the muscle to treat a painful and knotted area. It can be quite effective in helping chronic pain that’s coming from the muscles. TPI’s are usually performed blind in the office, but if the area is difficult to reach and deep, sometimes the physician will use x-ray or ultrasound guidance. While there is some radiation exposure with fluoroscopy (real time x-ray), the patient is only exposed to approximately a single chest x-ray worth. If the doctor uses musculoskeletal ultrasound, there’s no radiation exposure. As this low back pain patient handed me his films on several CDs, I noted there was a CT Scan. I opened the films to find that the sole reason the CT Scan was performed was for a trigger point injection (see picture above with the needle going into the muscle). I was flabbergasted, as neither myself nor my colleagues had ever seen a trigger point injection performed under CT Scan guidance (for obvious reasons-i.e. radiation exposure). In addition, like MRI, a CT Scan is a static image, meaning that in order to see where the medication is flowing you have to take multiple still shots rather than seeing it flow that direction in real time (as you can with fluoroscopy or ultrasound). As a result of this slow response time between injection and imaging, we’ve seen at least one serious complication occur. We’ve also seen this technology used by radiologists to inject the spine, again a cannon to kill a fly. The upshot? CT Scan simply has too much radiation exposure and too many limitations (like the inability to see the injection medication flow into the right area) to be an effective way to guide a needle for a precision injection. If you get offered an injection using a CT Scan, look around for the cannon and the dead fly.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.