Saving a Young Man’s Damaged Shoulder with Interventional Orthopedics
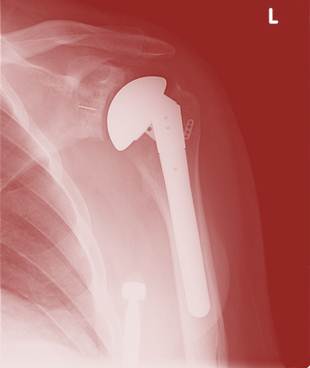
Shoulder Chrondolysis Treatment: KH is a 38 year old male whose shoulder problems began with a labral tear in 2004. He had surgery for the labral tear and they used a pain pump, which dissolved his cartilage (chondrolysis). He ultimately went to see another surgeon who told him he needed a shoulder replacement. When he was first evaluated in September of 2011, he felt his shoulder was unstable. This made sense, as they had performed a distal clavicle resection when they operated on his labral tear, a surgery that often leaves the shoulder unstable. He was getting pain from the shoulder up to his neck and had significant pain at rest, with nothing that would totally relive his pain which could be as high as an 8/10. While it was clear he had no cartilage and our only other option outside of shoulder replacement would be a Regenexx-SD or Regenexx-C shoulder stem cell procedure, more importantly, just fixing the obvious joint problem (if that were even possible-not certain due to the severe cartilage loss) may not solve his disability. This was because another key issue in the shoulder was also severe instability. Our interventional orthopedics philosphy (read Orthopedics 2.0 our practice’s book how interventional orthopedics will change musculoskeletal care) required that we first deal with the instability before using stem cells. This is because putting stem cells or any other biologic into an unstable shoulder joint is like putting new tires on a car with a wobbly rim, the tires will just quickly wear out again. As a result, I began using proliferant injections under ultrasound guidance into what was left of his coraco-acromial ligaments, AC joint capsule, and posterior inferior glenohumeral ligament. After four of those treatments plus cleaning up the trigger points in the neck and shoulder, his pain is way down and his function is way up. As an example, we recently had two feet a snow here and he was dreading having to shovel it, because he knew from experience that shoveling snow would put his shoulder out of commission for a week. After we stabilized the shoulder through injections, he shoveled the snow and while he felt sore that night, the shoulder felt fine the next morning. Now that the shoulder is stable, we can move onto step 2, trying to help the joint cartilage. While we’re just halfway through his treatment, he’s a good example of why an interventional orthopedics approach makes sense. Rather than “blindly injecting magic stem cells” into the joint and hoping the pixie dust works, understanding the biomechanics of why the shoulder hurts is as important as any stem cell therapy.
NOTE: Proliferent injections are a medical procedure, and like all medical procedures have a success and failure rate. Not everyone will experience the same results.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.