Spinal Fusion Complications
Spinal fusion complications are surprisingly common, yet it’s big business. So how successful are these surgeries? How long does it take to recover? What are the complications and how often do they actually happen?
What is a Spinal Fusion and Why Is It Done?
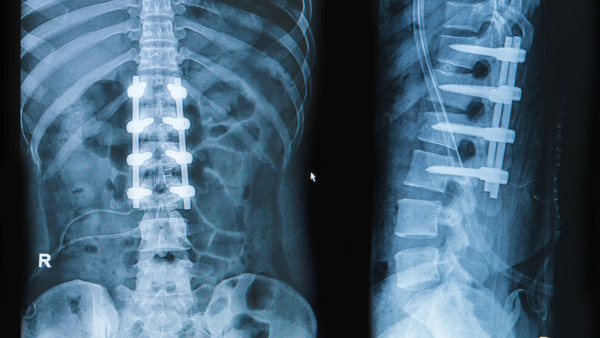
X-rays showing the results of spinal fusion surgery. Praisaeng/Shutterstock
Spinal fusion is a surgery where the surgeon uses bone and/or hardware to bolt certain segments of the spine together to prevent motion. The most common reason it’s performed is for degenerative disc disease and low back pain, but fusions are also performed in the neck.
What is the Success Rate of Spinal Fusion Surgery?
Before we get into spinal fusion complications, let’s talk about the success rate of spinal fusion surgery. In the largest investigation published to date that looked at the results of 65 studies and more than 300,000 patients, the research was mixed as to whether low back fusion worked better for low back pain patients who got surgery when compared to patients who opted to skip the surgery (1). In particular, for better studies included in this review, there was no difference in pain levels between those who got fusion when compared to those who didn’t. It did work better for patients who had a slipped vertebra otherwise known as spondylolisthesis. hence, given that most patients get fusion for chronic low back pain, fusion surgery didn’t work all that well.
Is Spinal Fusion Major Surgery?
In short, yes, spinal fusion complications are common, hence this is major surgery. First, you need to understand that research has demonstrated that surgeons can underestimate complications (3). Taking that into account, in an analysis that reviewed five large studies, the serious complication rate of spine surgery is 10-24% (4). Even minimally invasive fusions where smaller incisions are used have a reported complication rate of 19% with some studies reporting larger fusion surgery complication rates as high as 31% (10). Those side effects can include nerve damage, infection, increased pain, needing more surgery, and other problems.
How Long does it Take to Recover from a Spinal Fusion?
Generally, you’ll be in pain and on narcotics for between 2-9 weeks depending on the type of surgery (5-7). Time off work will be from as little as 7 weeks to more than 6-months (2). Most surgeons tell their patients that full recovery is about a year out.
What are the Symptoms of a Failed Lumbar Fusion?
One of the main spinal fusion complications is a failure of the procedure. There are a few main ways for fusion to fail and they fall into the following categories:
- Non-union
- Hardware loosening or breakage
- Hardware pain
- Adjacent segment disease
First, the segment being fused with bone can fail to grow together and this is called a non-union. How often this happens is highly dependent on the type of fusion surgery performed. For procedures that require more bone, like a posterior-lateral fusion, the non-union rates are as high as 26% to 36% (8, 9).
Hardware loosening, breakage, and pain are a common reason second surgeries are performed after fusion. Overall, about 13% of patients who have a low back fusion need a second surgery (11).
Adjacent segment disease (ASD) means that the vertebral levels above or below get worn out due to too much force on those areas because of the immobile fusion (12). At about 2 years after a low back fusion, 12% of patients will have ASD (16). In addition, 2-4% of patients will get this problem for every year after the fusion, so at 5-years, up to 20% of patients will have ASD (17). To learn more, watch my video below:
Newer Non-Fusion Approaches
A really big idea in the world of spine surgery has been that you can avoid spinal fusion complications by replacing the disc with a moveable piece of hardware and keep some motion. This should be better than fusing the area and losing all motion. This surgery is called an artificial disc replacement (ADR). However, the research to date hasn’t been convincing that this type of surgery prevents ASD (12- 15). Meaning, getting an artificial disc implanted seems to be no better than getting your spine fused.
There is another way to go that can avoid spinal fusion complications that we’ve been using for the last decade with great success. This is an off-shoot of our published work using platelet based therapies in the spine (18). This is the use of interventional orthobiologics and a fusion substitute that we created called the Perc-FSU procedure.
FSU here means the Functional Spinal Unit which consists of the disc, facet joints, ligaments, and muscles that all help to stabilize the spine. The goal of this procedure is to inject the growth factors from your blood platelets to help tighten ligaments, wake up atrophied muscles, and treat damaged joints and irritated nerves. Find out more below:
The upshot? It’s amazing that spinal fusion complications are so high and accepted. We help thousands of patients every year avoid spinal fusion for this reason.
_____________________________________________
References:
(1) Yavin D1, Casha S1, Wiebe S, Feasby TE, Clark C, Isaacs A, Holroyd-Leduc J, Hurlbert RJ, Quan H, Nataraj A, Sutherland GR, Jette N. Lumbar Fusion for Degenerative Disease: A Systematic Review and Meta-Analysis. Neurosurgery. 2017 May 1;80(5):701-715. doi: 10.1093/neuros/nyw162.
(2) Wang X, Borgman B, Vertuani S, Nilsson J. A systematic literature review of time to return to work and narcotic use after lumbar spinal fusion using minimal invasive and open surgery techniques. BMC Health Serv Res. 2017;17(1):446. Published 2017 Jun 27. doi: 10.1186/s12913-017-2398-6
(3) Ratliff JK, Lebude B, Albert T, Anene-Maidoh T, Anderson G, Dagostino P, Maltenfort M, Hilibrand A, Sharan A, Vaccaro AR. Complications in spinal surgery: comparative survey of spine surgeons and patients who underwent spinal surgery. J Neurosurg Spine. 2009 Jun;10(6):578-84. doi: 10.3171/2009.2.SPINE0935.
(4) Zaina F, Tomkins-Lane C, Carragee E, Negrini S. Surgical versus non-surgical treatment for lumbar spinal stenosis. Cochrane Database Syst Rev. 2016;2016(1):CD010264. Published 2016 Jan 29. doi:10.1002/14651858.CD010264.pub2
(5) Adogwa O, Parker SL, Bydon A, Cheng J, McGirt MJ. Comparative effectiveness of minimally invasive versus open transforaminal lumbar interbody fusion: 2-year assessment of narcotic use, return to work, disability, and quality of life. J Spinal Disord Tech. 2011;24(8):479–484. https://www.ncbi.nlm.nih.gov/pubmed/21336176
(6) Parker SL, Adogwa O, Bydon A, Cheng J, McGirt MJ. Cost-effectiveness of minimally invasive versus open transforaminal lumbar interbody fusion for degenerative spondylolisthesis associated low-back and leg pain over two years. World Neurosurg. 2012 Jul;78(1-2):178-84. doi: 10.1016/j.wneu.2011.09.013.
(7) Parker SL, Mendenhall SK, Shau DN, Zuckerman SL, Godil SS, Cheng JS, et al. Minimally invasive versus open Transforaminal lumbar Interbody fusion for degenerative Spondylolisthesis: Comparative effectiveness and cost-utility analysis. World Neurosurg. 2013. https://www.ncbi.nlm.nih.gov/pubmed/23321379
(8) Herkowitz HN, Kurz LT. Degenerative lumbar spondylolisthesis with spinal stenosis. A prospective study comparing decompression with decompression and intertransverse process arthrodesis. J Bone Joint Surg Am. 1991 Jul; 73(6):802-8. https://www.ncbi.nlm.nih.gov/pubmed/2071615/
(9) Tsutsumimoto T, Shimogata M, Yoshimura Y, Misawa H. Union versus nonunion after posterolateral lumbar fusion: a comparison of long-term surgical outcomes in patients with degenerative lumbar spondylolisthesis. Eur Spine J. 2008;17(8):1107–1112. doi: 10.1007/s00586-008-0695-9
(10) Joseph JR, Smith BW, La Marca F, Park P. Comparison of complication rates of minimally invasive transforaminal lumbar interbody fusion and lateral lumbar interbody fusion: a systematic review of the literature. Neurosurg Focus. 2015 Oct;39(4):E4. doi: 10.3171/2015.7.FOCUS15278.
(11) Greiner-Perth R, Boehm H, Allam Y, Elsaghir H, Franke J. Reoperation rate after instrumented posterior lumbar interbody fusion: a report on 1680 cases. Spine (Phila Pa 1976). 2004 Nov 15;29(22):2516-20. https://www.ncbi.nlm.nih.gov/pubmed/15543064
(12) Saavedra-Pozo FM, Deusdara RA, Benzel EC. Adjacent segment disease perspective and review of the literature. Ochsner J. 2014;14(1):78–83. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3963057/
(13) MacDowall A, Canto Moreira N, Marques C, Skeppholm M, Lindhagen L, Robinson Y, Löfgren H, Michaëlsson K, Olerud C. Artificial disc replacement versus fusion in patients with cervical degenerative disc disease and radiculopathy: a randomized controlled trial with 5-year outcomes. J Neurosurg Spine. 2019 Jan 11;30(3):323-331. doi: 10.3171/2018.9.SPINE18659.
(14) Yang X, Janssen T, Arts MP, Peul WC, Vleggeert-Lankamp CLA. Radiological follow-up after implanting cervical disc prosthesis in anterior discectomy: a systematic review. Spine J. 2018 Sep;18(9):1678-1693. doi: 10.1016/j.spinee.2018.04.021.
(15) MacDowall A, Skeppholm M, Lindhagen L, Robinson Y, Löfgren H, Michaëlsson K, Olerud C. Artificial disc replacement versus fusion in patients with cervical degenerative disc disease with radiculopathy: 5-year outcomes from the National Swedish Spine Register. J Neurosurg Spine. 2018 Nov 2;30(2):159-167. doi: 10.3171/2018.7.SPINE18657.
(16) Zhong ZM1 Deviren V, Tay B, Burch S, Berven SH. Adjacent segment disease after instrumented fusion for adult lumbar spondylolisthesis: Incidence and risk factors. Clin Neurol Neurosurg. 2017 May;156:29-34. doi: 10.1016/j.clineuro.2017.02.020.
(17) Tobert DG, Antoci V, Patel SP, Saadat E, Bono CM. Adjacent Segment Disease in the Cervical and Lumbar Spine. Clin Spine Surg. 2017 Apr;30(3):94-101. doi: 10.1097/BSD.0000000000000442.
(18) Centeno C, Markle J, Dodson E, et al. The use of lumbar epidural injection of platelet lysate for treatment of radicular pain. J Exp Orthop. 2017;4(1):38. Published 2017 Nov 25. doi: 10.1186/s40634-017-0113-5

NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.
